Questions and Answers about Infertility and its Treatment
- This is also available in a PDF Version (PDF, 1.3MB, 76pg.)
Who wrote this guidebook
The New York State Task Force on Life and the Law was created in 1985 to develop public policy on issues arising from medical advances. Task Force members include leaders in the fields of law, medicine, nursing, philosophy, consumer rights, religion and ethics.
In 1998, after extensive research and interviews with people involved in fertility treatment, the Task Force found that patients have frequently not been adequately informed before giving their consent to undergo these procedures. The Task Force received a grant from the Ford Foundation to create a model process and form for obtaining informed consent, and this guidebook for persons with infertility.
Table of Contents
INTRODUCTION
- What makes infertility treatment special?
DEFINING INFERTILITY
- What is infertility?
- Is infertility a male or female problem?
- If I had a baby once, can I be infertile now?
- What causes infertility?
- Is infertility becoming more common?
- Does age affect fertility?
- Does stress cause infertility?
- Can infertility be prevented?
- Can infertility be cured?
GETTING THE DIAGNOSIS
- What can we do before seeing a doctor?
- When should we seek medical help?
- What will happen first? How is the cause of infertility identified?
- Do we both need to be tested?
- What tests are really necessary?
- Do we need to see a specialist?
- How soon will we have an answer?
- What if all our tests are normal?
ROUTES TO CREATING A FAMILY
- Besides medical treatment, what options do we have?
- Is it true that, if we adopt, we're likely to get pregnant?
- Can we pursue adoption and medical treatment at the same time?
- Will our doctor discuss adoption?
SELECTING A PHYSICIAN OR INFERTILITY PROGRAM
- Do all programs offer the same treatments?
- Will we be treated right away?
- Is word-of-mouth a good way to find a program? How do we select a doctor we can trust?
- What kind of emotional support should I expect?
- Success Rates
- Can a program predict whether I'll become pregnant?
- What do the odds mean?
- Your Right to Treatment
- Can a doctor deny treatment?
- Are we required to take medical and psychological tests unrelated to infertility?
- Can single women or lesbian couples receive infertility treatment?
MAKING DECISIONS ABOUT INFERTILITY TREATMENT
- General Considerations
- What makes this different from other medical decisions?
- Will my religion approve?
- Should we get a second opinion?
- What information should we expect before agreeing to a treatment?
- What if we are offered a brand-new treatment?
- Surgery
- Should I undergo surgery?
- What if my partner or I have been sterilized?
- Fertility Drugs
- Should I use fertility drugs?
- Can the safety of fertility drugs and the likelihood of pregnancy be enhanced?
- Intrauterine Insemination
- Should I use IUI?
- In Vitro Fertilization
- Should I undergo IVF?
- What are the alternatives to IVF?
- Once we agree to undergo IVF, what decisions need to be made?
- What additional treatments or procedures may be recommended?
- How can I find out where I'll have the best chance to have a baby?
- Should I go to the program with the highest CDC success rates?
- Can I rely on the success rates published in advertisements?
- Donor Semen, Eggs, and Embryos
- Who uses donors?
- Where does donor semen come from?
- Where do donor eggs come from?
- Where do donor embryos come from?
- Can infectious diseases be passed through donor semen?
- Can infectious diseases be passed through donor eggs?
- Can donor semen or eggs result in birth defects or inherited diseases?
- What if my egg donor develops medical complications?
- What will we know about the donor?
- Can we meet our donor?
- Can we use the semen or eggs of a relative or friend?
- Should we tell our child we used a donor?
- Should we tell our relatives and friends we're using a donor?
- Is my child likely to meet other children who are blood relatives through the donation?
- Can our donor find out who we are?
- What if my child needs medical information about the donor, or wants to learn his/her identity?
- Will I be the legal mother if my baby was created with a donor egg?
- Will my husband be the legal father if we use donor semen?
- What if a semen donor comes back and wants the baby?
- The Use of Surrogates
- What if I can't carry a pregnancy?
- The Issue of Multiple Births
- Why are so many twins born after infertility treatment?
- Is pregnancy more risky with multiples?
- If twins or triplets are OK with us, what's the problem?
- Can multiple births be prevented?
- Can a multiple gestation be fixed?
- Are some programs more likely to create multiples?
- Freezing Embryos
- If all the embryos aren't transferred, what happens to them?
- Does freezing hurt the embryos?
- How long can I wait to use the embryos?
- If I never use the frozen embryos, what happens to them?
- Who is allowed to make decisions about the embryos?
- What if we get divorced or one of us dies?
PAYING FOR INFERTILITY TREATMENT
- What will treatment cost?
- Will our insurance cover infertility treatment?
- What can we do if an insurance claim is denied?
- Should we pick a program with a money-back guarantee?
- How do the costs of infertility treatment compare with the costs of adoption?
LOOKING AHEAD TO PREGNANCY AND PARENTHOOD
- Will my infertility specialist see me through the pregnancy?
- Are there special concerns for pregnancies achieved through infertility treatment?
- Does infertility treatment endanger the children conceived?
IF TREATMENT FAILS
- When a cycle of infertility treatment doesn't work, should we try again?
- When is it time to find a new doctor or take a different approach?
- When is it time to stop treatment?
RESOURCES
- New York State Offices
- Other Organizations
GLOSSARY
NEW YORK STATE TASK FORCE ON LIFE AND THE LAW Advisory Group on Assisted Reproductive Technologies
Introduction
Return to TopEvery year, thousands of couples seek medical assistance because they want a child and find it difficult to become pregnant or to carry a pregnancy to term. The New York State Task Force on Life and the Law created this guidebook because, in many ways, the treatment of infertility is even more complex than other issues faced by medical consumers.
What makes infertility treatment special?
- There are no clear medical answers. Experts hold differing opinions about all aspects of treatment. There are no firm guidelines regarding when it should be recommended, what diagnostic tests mean, and when treatment should be ended.
- The treatment is expensive. Infertility treatments can cost hundreds to tens of thousands of dollars, depending on the procedures used. Insurance does not generally cover all treatments. In addition, some fertility programs advertise money-back guarantee programs that are unique in medical treatment.
- Complications can harm people who were in good medical condition before treatment began. When a donor provides the eggs, or a pregnancy is carried by a gestational surrogate, treatments with significant risks may be performed on people who will have no direct medical benefit.
- Resulting children must be considered. If it works, treatment results in the conception and birth of children with rights and interests of their own.
- Many patients will not have a successful outcome despite treatment. Others will become pregnant without treatment.
- Laboratories have unique responsibilities. Infertility programs sometimes have long-term custody of embryos.
This guidebook suggests issues for you to consider if you are facing infertility and questions to ask before making important treatment decisions. A doctor has a professional responsibility to offer medical advice, but only you can weigh all the medical and personal information needed to arrive at a decision.
In this guidebook, specific medical procedures will be described in general terms only. It is important that you obtain and understand the details of any treatments. They will not be covered here because of the variety of approaches used, and because this field of medicine is evolving rapidly. Likewise, the success rates of various procedures change over time and differ depending on the patient and the program.
Defining Infertility
Return to TopWhat is infertility?
Infertility is difficulty in conceiving a pregnancy. This general term does not identify the cause of the problem or whether it will be permanent.
Often, physicians and researchers consider a couple to have infertility if they have not conceived, despite regular intercourse without using birth control, for at least a year. Fifteen to 20 percent of couples will not conceive despite a year of trying. However, this does not mean that they will not conceive later on, even without treatment. Some investigators consider two years without conception to be a better indicator of a couple's need for assistance.
More than 90 percent of couples will have achieved a pregnancy within two years.
When an individual has no chance to conceive without treatment (for example, a woman does not ovulate or has two blocked fallopian tubes), it is sometimes called sterility.
Is infertility a male or female problem?
In the past, infertility was commonly considered to be solely a female problem. It is now recognized that a couple's infertility is just as likely to stem from problems in the male partner. After couples with infertility undergo testing, about 40 percent of the cases are found to stem from female factors and another 40 percent from male factors.
In 10 percent of couples, infertility factors are found in both the man and woman. In the remaining 10 percent, the infertility remains unexplained after testing.
Because either or both may be involved, it is important to test both the man and woman before starting treatment. No matter what the cause, most treatments require the active participation of both partners.
If I had a baby once, can I be infertile now?
Yes. Secondary infertility is the name given when the problem arises in a couple who have been able to get pregnant in the past. Sometimes a new factor, such as an infection, has damaged the reproductive organs since the last child was born. Sometimes the aging process makes it more difficult for a couple to conceive, even if they had no problems when they were younger.
Secondary infertility is even more common than infertility in couples who have never achieved a pregnancy.
Generally, the diagnosis and treatment is the same. However, couples with secondary infertility may make different treatment choices as they take into account the needs of their other children. Overall, treatments are somewhat more likely to work in women with secondary infertility than in women who have not previously become pregnant with the same partner.
Couples with secondary infertility may wish to seek emotional support specifically geared to their concerns. These couples often report that they feel caught between two worlds. They feel alienated from those who easily create families of the size they want, while at the same time they are envied by childless people with infertility.
"My first baby was born at 36 - no problem. I got pregnant the first try. But, three years later, I didn't get pregnant." INFERTILITY PATIENT
What causes infertility?
For a couple to conceive and carry a pregnancy, four parts of the reproductive system must be working adequately:
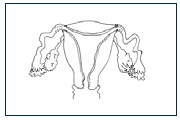 1) A woman's ovaries must be regularly producing and releasing good-quality eggs.
1) A woman's ovaries must be regularly producing and releasing good-quality eggs.
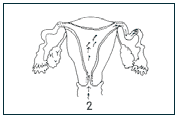 2) Normal sperm must be produced in high enough numbers and delivered during sexual intercourse.
2) Normal sperm must be produced in high enough numbers and delivered during sexual intercourse.
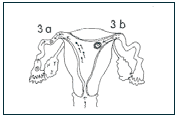 3) The reproductive passageways must be clear enough for: a) sperm to enter the uterus (through the cervix) and swim into the tubes to unite with the egg; b) the egg or early embryo to travel to the uterus (through the fallopian tubes).
3) The reproductive passageways must be clear enough for: a) sperm to enter the uterus (through the cervix) and swim into the tubes to unite with the egg; b) the egg or early embryo to travel to the uterus (through the fallopian tubes).
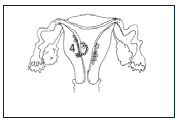 4) The lining of the uterus must be capable of having the embryo implant, and of sustaining the pregnancy.
4) The lining of the uterus must be capable of having the embryo implant, and of sustaining the pregnancy.
Many types of problems - including hormone abnormalities or blockages caused by infection or scar tissue - can affect one or more of these functions.
Is infertility becoming more common?
According to national data, there has not been a major increase in the proportion of couples who are infertile. However, many more women are seeking medical services for the diagnosis and treatment of infertility - particularly those who have not previously had any children.
Does age affect fertility?
In general, women's fertility begins to decline gradually after age 30, with a steep drop between 35 and 45. This means that, on average, it takes longer for an older woman to conceive, and older women are more likely to be diagnosed with infertility. Pregnancies in older women are also more likely to miscarry.
The most predictable age-related change is a gradual reduction in the number and quality of eggs produced as a woman enters her late thirties. As she nears menopause, eggs are not released in more and more of a woman's menstrual cycles, making conception impossible.
"The office said they don't refer to infertility specialists until a year of trying. I said maybe they shouldn't wait that long in someone who is 39, and she agreed." IVF PATIENT
Also, as women age, they are more likely to have had illnesses or medical treatments that can compromise fertility. Some of these affect the reproductive system directly, such as endometriosis, sexually transmitted diseases (STDs), surgery on the reproductive organs, or ectopic pregnancies. Others are general medical problems that can damage fertility, such as hypothyroidism, high blood pressure, diabetes and lupus.
As they age, men may also be exposed to infections, medications, or occupational or environmental chemicals that can impair fertility. However, they do not experience the same dramatic and predictable age-related decline as women.
Because of the increased possibility of fertility problems, women over the age of 35 are often counseled to seek medical advice if they attempt to conceive for six months without success. However, because conception is likely to take longer in older women, some experts suggest that couples give themselves more, rather than less, time to conceive before seeking medical help.
Couples must find a balance between not allowing enough time for conception and delaying too long (making treatment less likely to succeed).
Does stress cause infertility?
However well-intentioned, the statement "just relax and you'll get pregnant" has been very hurtful to couples with infertility. Two decades ago, researchers thought that almost half of infertility in women could be attributed to stress and psychological factors. Nowadays infertility is better understood, and stress is recognized primarily as a result, rather than a cause, of fertility problems. However, there is evidence that stress can have a negative impact on sperm and egg production. Research is ongoing to help understand how stress may influence fertility and the success of treatment.
Can infertility be prevented?
Sometimes. By learning about the known causes of infertility, young men and women can reduce the risk that they will face this challenge when they decide to start a family. Some strategies for prevention:
Take precautions (such as the use of condoms) to avoid sexually transmitted diseases (STDs). STDs, particularly gonorrhea and chlamydia, can infect the reproductive tract and cause blocked fallopian tubes or sperm-carrying ducts.
Seek prompt treatment for potential STDs. STDs cause more harm to fertility if they are untreated or not completely treated.
When selecting a birth control method, learn about its possible impact on future fertility and make that an important factor in your decision.
Make medical decisions with fertility in mind. Inquire about the impact of medications, including herbal supplements, on reproduction in men and women. If you develop a gynecologic condition, such as a uterine fibroid, endometriosis, or abnormal Pap smear, ask which treatments are most likely to preserve your fertility.
Make fertility-enhancing lifestyle choices. In men, excess heat exposure can lower fertility. Cigarette smoking is associated with an abnormal semen count in men. In women, smoking can reduce fertility and raise the risk of miscarriage. Being underweight, losing weight rapidly, or exercising at an extreme level can impair fertility in both men and women. In women, obesity is also associated with lower fertility. For some couples, changing exercise habits or achieving a more healthful body weight leads to conception with no medical treatment.
Allow sufficient time to attempt conception. Many infertility factors do not make it impossible to conceive but lower the chance with each cycle. This lengthens the amount of time conception is likely to take. If you do not try to become pregnant until late in your reproductive years, or if you count on conceiving within a short time period, you are more likely to be unsuccessful and to assume you need medical help - even if you might be capable, given enough time, of conceiving without treatment.
Can infertility be cured?
Some treatments correct factors that cause infertility. If they work, the infertility should be reversed and a couple should be able to achieve one or more pregnancies. In contrast, other therapies are used to establish pregnancy in a treatment cycle without permanently correcting the underlying problem.
In some cases, medication can improve or correct an underlying medical condition that makes it difficult to conceive. Women with endometriosis, cervical infections, polycystic ovarian syndrome, or hormonal imbalances can be treated with medications, thus easing barriers to conception.
When a woman has blocked or damaged fallopian tubes, surgery to repair them is an example of treatment aimed at curing infertility. If it is successful (meaning the tube is both open and able to function normally), she should be able to conceive one or more times without further medical intervention. However, many experts believe that, for most women with blocked tubes, the chance of becoming pregnant is greater using in vitro fertilization(a technique to get around the problem) than surgery.
When considering various treatments, ask whether each approach is supposed to circumvent infertility or cure it. Get information about the chance of success with each approach (in light of your age and diagnosis) and its costs (including learning if your insurance carrier covers it).
Getting the Diagnosis
Return to TopWhat can we do before seeing a doctor?
While you are trying to conceive, enjoy a healthful lifestyle. Take note of the strategies for preventing infertility (above) and consider how - such as smoking - you may be lowering your chances to conceive. Tell your doctor and pharmacist that you are trying to get pregnant. They can tell you whether any prescription or over-the-counter medications, supplements, or herbal remedies you or your partner use could be disturbing your fertility or be dangerous to use during early pregnancy. If so, ask what alternatives are available. Avoid douching or using vaginal lubricants.
Even a couple with no fertility problems have only about a one in four chance of conceiving during a single cycle. Maximize your chances by having sexual intercourse regularly during the fertile part of your cycle. If you have questions about when you are most likely to conceive, ask a health care professional. An ovulation predictor (available without a prescription) may help you determine when you ovulate so you can better time intercourse.
When should we seek medical help?
Most doctors advise you not to be concerned unless you have been trying to conceive - not using birth control and having regular intercourse around the time of ovulation - for at least a year.
Women with certain symptoms or previous medical conditions may wish to seek medical advice earlier. Some symptoms or prior conditions make fertility problems more likely, and others may indicate a medical condition that needs treatment for other reasons. Seek medical advice if:
- You have lots of pain during your menstrual period or during intercourse.
- You have an abnormal menstrual cycle (less than 21 or more than 35 days from the first day of one cycle to the first day of the next).
- You are troubled by acne or excess facial or body hair.
- You have had pelvic inflammatory disease (PID), an infection in the reproductive organs, usually the fallopian tubes.
- You have had surgery on your reproductive organs, such as a cone biopsy of the cervix.
- You have had more than one miscarriage.
- Your partner has an abnormal sperm analysis.
What will happen first?
Ideally, a couple will attend the first medical appointment together. The man and woman will be interviewed about many topics in order to determine possible reasons that conception has not occurred. A man may be asked about his development at puberty; whether he has ever fathered children, if he has had infections or other illnesses, or any injuries or operations involving his genitals; and what medications he has used. He will also be asked about recreational drug use, and any chemicals to which he is exposed in his work or hobbies.
A woman may be asked details about her reproductive history, including her puberty and menstrual cycle; contraceptives used; pregnancies, abortions or miscarriages; pelvic surgeries; gynecologic symptoms; and previous infections. She will also be asked about her general medical history, medication or recreational drug use, and chemical exposures. Both partners should expect to answer frank questions about their sexual histories and attempts to conceive.
"I already had an inkling it might be hard for me to get pregnant, because I had one ovary removed as a teenager." EGG DONATION PATIENT
The initial physical exam is likely to focus on the hormonal system and reproductive organs. Afterward, further testing may be recommended or you may be offered information and advice on attempting to conceive before you undergo further evaluation.
How is the cause of infertility identified?
An infertility work-up will involve tests to determine how well each of the systems involved in conception is working.
- EGG PRODUCTION: To determine if and when you are ovulating (producing and releasing a mature egg during the menstrual cycle), you may be asked to chart your basal body temperature. You will take your temperature before getting out of bed each morning. A slight, sustained rise in temperature is an indirect indication that ovulation has occurred. You may also be asked to use an ovulation predictor kit at home. Your doctor may check various hormone levels on specific days in your menstrual cycle, or monitor your body's response to a dose of fertility medications.
- SPERM PRODUCTION: A semen specimen will be analyzed for the number of sperm, their shape and movement. If the results are abnormal, a man may be examined by a urologist or tested for hormonal abnormalities or infection.
- FALLOPIAN TUBES: To see whether the fallopian tubes are open, an X-ray (called a hysterosalpingogram or HSG) may be taken while dye is injected into the uterus and tubes. Alternatively, a doctor might inject a salt-water solution and view the uterus and tubes using ultrasound (called a sonohysterogram). The tubes can also be observed during a surgical procedure.
- CERVIX: To determine whether sperm are able to swim through the cervix, a sample of cervical mucus is examined after intercourse. If this post-coital test is abnormal, other tests may be ordered to find out why. Doctors disagree about the usefulness of this test, and many couples conceive despite poor results on a post-coital test.
- UTERUS: The shape of the uterus is shown in an HSG. It can also be seen through a telescope-like device (hysteroscope) inserted through the vagina and cervix. An endometrial biopsy samples the uterine lining in the last half of the cycle to see if it is prepared for an embryo to implant. The thickness of the lining can also be measured using ultrasound.
Do we both need to be tested?
Almost always. Both male and female factors can contribute to a couple's infertility. For efficiency, diagnostic testing may focus first on tests that are less invasive (such as a semen analysis) or those that may confirm a suspected problem (such as a test for blocked fallopian tubes if a woman has had a pelvic infection).
What tests are really necessary?
Doctors and infertility programs vary in which diagnostic tests they recommend or require. Some variations reflect differing medical opinions on the value of specific tests. For example, some doctors insist on an endometrial biopsy or post-coital testing while others find them of little use. A test's value also depends on the person being tested and the treatment being considered. For example, if a woman is in her 40s, the first priority may be to test for age-related changes in her ability to produce eggs. Until those results are in, a doctor might consider other tests a waste of time.
- Before undergoing a test, ask enough questions to assure yourself that it will be worth the time and expense involved and will help guide your treatment. Some questions to ask include:
- What will the results tell us about the chance for pregnancy with or without treatment?
- Might the results be different if the test was repeated?
- Is the test ever abnormal in people with normal fertility?
- Are there other ways to get the same information?
- How do the alternatives compare in reliability, risk and cost?
- How will the results affect the next step that we take? (If the doctor's advice will not depend on the results, there may be little reason to have the test.)
In addition, make sure you understand what will be involved in taking the test. Ask:
- What are the risks of the test?
- Do most people find it painful?
- Must it be performed at a certain time in the menstrual cycle?
- What preparation is required?
- How expensive is it?
- Will insurance cover this test? (Your insurance company, not your doctor, is likely to be the best source for this information.)
Do we need to see a specialist?
Doctors from various medical disciplines treat infertility. A gynecologist may or may not have extensive experience in this area.
Experts often suggest seeing a specialist if you:
- Have endometriosis or damaged tubes.
- Are considering pelvic surgery for any reason.
- Have had two or more miscarriages.
- Have irregular menstrual cycles or another reason to believe you do not ovulate regularly.
- Have an abnormal semen analysis.
- Are a woman age 35 years or older.
- Have had a pelvic infection.
- Have not conceived in two years despite normal test results.
If you are already being treated by a non-specialist, request a referral or ask that doctor when it might be advisable to consult a specialist. If your current doctor makes the referral, it may smooth the transfer of care and exchange of information. Some health maintenance organizations (HMOs) do not include reproductive endocrinologists. Members may have difficulty obtaining a referral or having a specialist's services covered.
How soon will we have an answer?
Testing will likely take more than a month. Some tests must be scheduled at a specific point in the menstrual cycle. Others may require charting or repeated testing over a few months.
If you become concerned that your work-up is not proceeding efficiently, particularly if you are a woman over age 35, talk to your doctor about your concerns. Many infertility patients report that they regret having wasted valuable time prior to starting treatment.
What if all our tests are normal?
In 10 to 15 percent of couples, testing finds no reason for their reproductive difficulties. They are given the diagnosis of "unexplained infertility." This does not mean that no reason exists, just that testing has not revealed it.
If you are told you have unexplained infertility, ask whether other tests might clarify the situation. You may want to seek a second opinion.
Medical experts do not agree on the best way to treat unexplained infertility. Despite a few years of unexplained infertility, some couples will conceive with no treatment at all, particularly if they are younger. Other couples are offered standard treatments, such as fertility drugs and intrauterine insemination (IUI), or in vitro fertilization (IVF).
In general, couples with unexplained infertility are at least as likely to succeed with these treatments as are couples with a clear medical rationale for their use. If you are considering treatment for unexplained infertility, ask your practitioner to compare your chances of becoming pregnant with and without treatment.
Routes to Creating a Family
Return to TopBesides medical treatment, what options do we have?
People want children for many reasons. They may wish to create a genetic link with the future, to experience pregnancy and childbirth, to become a parent, to influence the next generation, or to nurture children. When fertility is not an issue, most people fulfill these at the same time by having and raising a child. Once fertility becomes an issue, a couple will need to assess which components are most vital to them and the various routes they can use to fulfill them. Counseling may be helpful to a couple as they discuss their priorities and evaluate their feelings on these issues.
If a couple decides that becoming a parent is their primary goal - more than having a genetic connection with the child they will raise - they may wish to pursue adoption. Adoption allows them to raise children and become legal parents. Within adoption, various alternatives can be pursued. A couple may seek to adopt a healthy infant of their own race; a child from another race and/or country; an older child; a child with special needs; or more than one child from a family.
Some couples decide not to pursue treatment or adoption and find other avenues for nurturing and influencing children. These often include teaching, becoming a mentor, or developing close relationships with nieces, nephews and friends' children. Others determine that if they do not have a child, they will focus their energy and resources on aspects of life other than nurturing children.
Even if they pursue medical treatment, couples may find that some of the aspects of parenting they desired are not available. For example, when sperm or egg donors are involved, one or both parents will not have a genetic link to the child. Or, when a surrogate is involved, pregnancy and delivery are not experienced.
Is it true that, if we adopt, we're likely to get pregnant?
No. For couples who continue trying to achieve pregnancy after adopting, the chances are the same as for couples who have not adopted. This myth has been hurtful to couples facing infertility, both because it is false and because it implies that adoption is not a joyful outcome, but simply a means to another end.
Can we pursue adoption and medical treatment at the same time?
There is no best time to consider adoption. Some couples pursue adoption rather than undergoing any treatment. Others do not want to consider adoption until they have pursued all medical approaches. Still others pursue the two options simultaneously.
In practical terms, it is not easy to actively pursue adoption and medical treatment at the same time. Some adoption agencies will not accept a couple who are still undergoing medical treatment. Both adoption and infertility treatments require time, money, and flexibility on the part of couples. However, couples have described being extremely disappointed if they postponed considering adoption and unsuccessfully tried medical treatments, only to find they had passed many agencies' age limits or no longer had the financial resources to adopt.
"I was on two adoption lists while I was doing the inseminations, and I said whichever happens first is fine." DONATION INSEMINATION PATIENT
Adoptive parents suggest that you begin to educate yourself about adoption while you are informing yourself about medical approaches to infertility. Talk to adoptive parents. Read about adoption and attend educational sessions by reputable groups such as RESOLVE, the national infertility association. Gather unbiased information to dispel any myths or assumptions you may have about adoption or infertility treatment. Some areas to research and compare include:
THE CHANCE OF SUCCESS
Like medical treatment, the chance of success with adoption depends on your personal circumstances (age, health, etc.) and the resources you can invest. Most people can adopt. It is untrue that it is no longer possible to adopt a healthy infant, but other adoption choices may make it possible to adopt sooner or at a lower cost.
LEGAL AND MEDICAL RISKS
Varying degrees of medical information are available on adopted children.
Medical treatment of infertility offers more control over a child's prenatal and early medical care.
However, the treatments are also associated with a higher risk of multiple births, which can result in children with serious medical problems. Legal issues must be addressed in adoptions as well as in many fertility situations involving frozen embryos or the use of donor semen, eggs or embryos.
Expenses
The cost of adoption and infertility are highly variable. The assistance you will receive for medical care will depend on your insurance coverage, employee benefits, and tax planning.
Will our doctor discuss adoption?
Yes. Not all doctors are equally informed about adoption, but your infertility specialist may have useful information. No matter where you get adoption information, you and your doctor should discuss all options to family building before you decide about medical treatment.
This will help you evaluate various options (medication, IVF, donor eggs or semen, gestational surrogacy, no treatment, adoption) and ensure that you and your doctor understand each other's attitudes towards various approaches - although you may certainly change your mind along the way. For example, a doctor who knows how important you consider experiencing a pregnancy, or who understands your religious beliefs about the use of donor eggs and semen, will be better able to help you assess your options. A doctor offering infertility treatment should respect that a medical approach is not right for every couple.
"Adoption should come up as an option, but the physician needs to take the lead from the woman. I thought if I can't have my own child, I just want to die. But I've been surprised to see it's a process, and I have changed." INFERTILITY PATIENT
Selecting a Physician or Infertility Program
Return to TopDo all programs offer the same treatments?
No, and even those capable of providing the same treatments will not offer the same approach for every couple. These questions may help you identify differences that are important to you:
Does the program primarily offer high-tech treatments, such as IVF? If you are just starting your work-up, a more general service might be a better fit.
Are several types of specialists involved? The ease of communication among specialists at larger programs may be an advantage. In particular, this may help couples requiring more than one type of treatment (for example, if there are both male and female factors).
Does the program offer what you need? If you foresee the need for a special service (such as egg donation for an older woman, or intracytoplasmic sperm injection - ICSI - to treat severe male infertility), look for a program with that expertise.
Does the program share your perspective about different treatments? Programs differ in attitudes about certain treatments. Some programs steer all women of a certain age towards the use of donor eggs; others do not. Some programs insist on certain tests and routine treatments that others consider of limited value.
Does the program share your attitudes about risk? Think about whether you are inclined towards taking the most or least aggressive approach. Are you and your doctor compatible in this regard?
Will we be treated right away?
Maybe not. Some programs have waiting lists, particularly for procedures that involve lengthy laboratory time or recruiting a donor. Ask how long you may wait; how treatments are scheduled; if you need more tests before starting; and whether the program shuts down at regular intervals.
Is word-of-mouth a good way to find a program?
You can learn a lot about the treatment experience by talking to friends or support group members.
Current or former patients can describe the emotional ups and downs, physical side effects and impact on daily life. The experience of other couples can also alert you to areas of potential support or frustration you may encounter. Did the schedule run on time? Were your questions answered? Did you get your test results easily? Was the staff helpful in dealing with financial issues?
When you know someone who has gotten pregnant, that may seem like the strongest endorsement to seek the same treatment at the same program. But, someone who did not succeed might hold less favorable views. Be cautious, therefore, in using the experience of others to gauge your chances of success at a specific program. Every couple brings different fertility problems, and your chances may be higher or lower than that of other couples you know.
How do we select a doctor we can trust?
Trust is extremely important as you make complicated decisions that involve your health, your family and large amounts of money.
Unfortunately, the field of infertility treatment has been marred by the well-publicized unethical, and even criminal behavior of a few doctors.
Make sure you know the experience and credentials of the doctor who will be treating you. To find out if a doctor is a board-certified OB-GYN, reproductive endocrinologist, or urologist, contact the American Board of Medical Specialties. This organization can also help you find a specialist in your area.
If a program's embryology lab has been accredited by an agency approved by the Society for Assisted Reproductive Technology (SART), it has been inspected and met SART's standards for handling and storing embryos. The New York State Department of Health is accredited by SART, so you can assume that any program licensed in New York State has met these standards. You can ask if a program's laboratory is accredited, or check the Web site of the Centers for Disease Control and Prevention (CDC). (See Resources) The CDC publishes this information along with annual success rates for ART programs.
In addition, RESOLVE offers referrals to doctors who meet its standards regarding education, training and focus on infertility treatment.
If you are getting information from the Internet, consider the source behind any endorsement of a particular treatment, physician or program.
Chances are good that the doctor or program you select will deserve your trust. As you pursue any type of medical treatment, keep in mind that a trustworthy doctor will not work in an atmosphere of secrecy. You should be able to see the information in your medical file and your doctor should be willing to discuss your treatment with colleagues. You should not be discouraged from seeking a second opinion.
What kind of emotional support should we expect?
Emotional support is vital when you are coping with infertility and its treatment. Infertility is a crisis that many women and men describe as the most upsetting of their lives. Treatment is also stressful and can place a major strain on couples. The medications used sometimes have an impact on a woman's mood and ability to concentrate. As treatment proceeds, patients describe riding a roller coaster of emotion as each test or step in the process seems to point towards eventual success or disappointment.
While most programs acknowledge the need for emotional support, they differ greatly in the services they require or offer. A counselor can help you evaluate your feelings about starting or continuing treatment and offer a valuable non-medical perspective on treatment and its demands. Some programs organize support groups and make counseling available. Others do not. Some programs include various relaxation techniques to ease the stress of treatment.
Your access to emotional support inside and outside a program should be considered as you decide where to be treated. At a minimum, any program offering infertility treatment should:
- Be sensitive to the stresses of treatment.
- Be supportive to the needs of individuals and couples.
- Help you anticipate and deal with predictable crisis points (such as getting pregnancy test results or having a miscarriage).
- Recognize that you need to consider non-medical factors, such as family responsibilities, as you decide whether to start or continue treatment.
- Schedule times to re-evaluate your approach to infertility.
"My biggest and only disappointment was that there was no counselor or support group." IVF PATIENT
"They had counseling if you wanted to avail yourself of it, but I didn't. I had a little support group of friends." IVF PATIENT
At some point, you may want to seek counseling from someone independent of a treatment program but knowledgeable about infertility treatments and issues. Particularly if you are considering treatment involving a donor or a surrogate, you and your partner can benefit from counseling as you sort through the many non-medical issues involved. Counseling or joining a support group may also help you, as an individual or a couple, receive support and develop strategies to cope with the stress of infertility and its treatment.
SUCCESS RATES
Can a program predict whether I'll become pregnant?
Every couple is unique, and there are serious limitations in any program's ability to predict how you will respond to treatment. You will likely be given an estimate of the chances you will achieve a successful pregnancy (either with or without treatment). It should be based on your diagnosis or test results, as well as the previous experience of that program or others in using the techniques. Be extremely cautious if someone offers you a guarantee or unrealistically high estimate of your chances.
When a prediction is made, ask what it is based on. The most directly applicable information would be your program's previous experience in treating similar couples. Often, however, predictions are made based on information from sources outside the program:
- National averages (your program may have higher-or lower-than-average success).
- A study published by a single center (which might have a very different level of experience).
- Data submitted by a manufacturer before a drug was approved by the Food and Drug Administration (and you may or may not be similar to the people they studied).
- Ask enough questions to feel comfortable that you are making a decision based, as closely as possible, on a program's experience treating people like you.
What do the odds mean?
Chances are, the success you're looking for is taking home a healthy, full-term baby. But, you can't assume that your definition is the same as the program's. To understand any odds they give you, you need to be clear on how they are defining two terms:
What do they count as a success?
Is it an open fallopian tube, a positive pregnancy test, a pregnancy that lasts at least into the second trimester, delivery of at least one living baby, or something else? If success is not defined as a live baby, ask enough questions to see how the odds they give relate to this goal.
How many pregnancies miscarry after the first trimester? How many of the pregnancies end prematurely? What is the chance of a stillbirth? In general, there are more statistics available about IVF than other infertility treatments.
What do they count as an attempt?
Is it one cycle of treatment or a series? Six months of trying to conceive after surgery or 12? Do they count treatment cycles that must be canceled in the middle (for example, due to a poor response to fertility drugs)?
YOUR RIGHT TO TREATMENT
Can a doctor deny treatment?
Yes. Doctors have a great deal of discretion in deciding whom to accept as a patient. A doctor must use professional judgment to determine whether a particular treatment is reasonable in your case. If not, a doctor might not accept you as a patient, or might refuse to continue with a course of treatment. Doctors are encouraged to have clear screening policies.
That way prospective patients can learn, in advance, what criteria or test results might be used to accept or reject them.
Factors that are often applied in infertility treatment are the:
- Age of the woman.
- Likelihood that treatment will succeed (both to avoid futile treatment and to avoid putting patients through high-tech treatments if they are likely to conceive without them).
- Presence of medical conditions that pose a risk to a pregnant woman or any resulting offspring.
- Welfare of any children who might be born as a result of treatment.
If doctors choose not to accept you for treatment, they should tell you why and inform you if there are other programs that might consider circumstances differently.
A doctor can not deny you treatment on the basis of your race, color, creed or national origin.
"All of them think they're being moral and ethical by saying your chances aren't good. I know my chances aren't great, but it did happen at age 43 and it might happen again." IVF PATIENT
Are we required to take medical and psychological tests unrelated to infertility?
Yes. As part of screening, you may be asked to undergo medical or psychological testing. For example, you may be required to be screened for infections that can be transmitted during pregnancy or through tissue transplants, such as hepatitis or human immunodeficiency virus (HIV) infection. Before a woman over a certain age is accepted, she may be required to undergo extra medical tests to determine whether her heart can withstand the physical demands of pregnancy. Doctors may require psychological testing in order to gauge a patient's stability and ability to make the decisions needed to safely undergo complex treatment.
Can single women or lesbian couples receive infertility treatments?
Usually. According to a recent national report, most programs in the country, including all programs in New York State, treat single women.
"Nobody blinked an eye at my being unmarried. I was treated gently, kindly, and appropriately... I'm glad I didn't have to go to a bar and get pregnant and worry about getting AIDS - to know there was a safe, sanitary way to have a child." DONOR INSEMINATION PATIENT
These women may wish to use donor insemination or may need additional treatments. Many programs also assist lesbian couples, although this was not asked as part of the national report.
New York State law permits, but does not require, fertility programs to accept single women or lesbian couples as patients. You can ask a program about its policy or check its report on the CDC Web site (see Resources). In addition to exploring treatment options, find out if you need to take special steps to ensure your parental rights. A growing number of states, including New York, allow a lesbian to adopt her partner's biological children without taking away the rights of the biological mother.
Making Decisions about Infertility Treatment
Return to TopGENERAL CONSIDERATIONS
What makes this different from other medical decisions?
In many ways, deciding about infertility treatment is similar to deciding about other types of elective health care. Your past experience as an informed medical consumer will serve you well. However, others who have been through the process - whether successful or not - urge you to keep in mind the many ways that infertility treatment can be different:
- Decisions about treatment must often be made without clear medical evidence of the benefits and risks.
- Treatment involves the intimate participation of both partners.
- Your decisions should take into account the best interests of children who may be created.
- Religious cultural and emotional factors can play an important role in decisionmaking.
- The costs may be high and are difficult to predict with accuracy.
- Treatment can damage your health or the health of a donor working on your behalf.
- An unique family arrangement is being created, and you are entering uncharted legal and psychological territory.
"I waited six months after getting the insemination information to make sure it was the right decision for me." DONOR INSEMINATION PATIENT
Will my religion approve?
You may wish to consult a religious advisor as you consider treatment. Organized religions have diverse views about the use of medical techniques to create a family. In addition, theologians and active members within each religion also vary in how they see these issues. When religions analyze a treatment, they commonly consider one or more of the following issues:
- Its impact on the bond of marriage.
- The importance that particular religion places on procreation.
- Whether a resulting child will be recognized within the religion.
- How embryos are created, stored and used.
- Whether it is acceptable to use third parties (such as semen and egg donors, or surrogates) in the creation of children.
- Concerns about accidental matings between relatives through the use of donor semen and eggs.
- The methods used to collect semen.
- Whom the religion will recognize as the parents.
Should we get a second opinion?
In infertility treatment, there are honest differences of opinion and philosophy among doctors. Many infertility experts encourage their patients to seek a second medical opinion before making major decisions. A second opinion may be helpful prior to medical intervention, when considering a new approach, or when re-evaluating whether to continue care. To get the most from a second opinion, have your records and test results sent to the doctor prior to your appointment. Be wary if a doctor discourages you from seeking a second opinion or resists sending your records.
What information should we expect before agreeing to a treatment?
A doctor is required to obtain your informed consent before treating you.
Before giving your consent to any treatment, you should have the following types of information (some of these apply only to IVF and its variants):
- A description of the treatment.
- A reasonable estimate of your chances of becoming pregnant and delivering a live baby. This should include how successful the treatments are, on average, for patients across the country and those treated at your program. The information should be compared with your chance of becoming pregnant without any treatment or with a less aggressive approach.
- How well-established the treatment is in the field.
- How much experience the program and its doctors have with the treatment.
- The risks of the treatment, including the risks of all medications and procedures.
- The chance of a multiple pregnancy and its risks for the mother and the pregnancy. This should include the fact that you may be asked to consider multi-fetal pregnancy reduction, explaining the process and its complications (see "Can multiple gestion be fixed?). It should also include ways to minimize the chance of multiple pregnancy.
- Problems that may occur during pregnancy and how they may affect you and the baby(ies).
- An estimate of the fees for treatment, plus predictable charges not covered in standard fees.
- Your options regarding the use of any eggs or embryos not used during your treatment.
- Other treatments offered at this program or others and the non-medical alternatives, including adoption and no treatment at all.
"The reproductive endocrinologist gave me the most down-to-earth prognostic information, saying my chances were less than 5 percent. In many ways, that was what we needed to hear." PATIENT UNSUCCESSFUL WITH STANDARD IVF AND SUCCESSFUL WITH DONOR EGGS
While your doctor should describe your various options, he or she will likely offer an opinion on which medical course of action is preferable. It is a doctor's professional responsibility to offer medical advice, but only you can make the decision that best addresses your medical and non-medical concerns.
"Nobody told me until after my second cycle that IVF is designed for basic infertility problems, not for old eggs. If someone had analyzed the chance this process would help with my problem, and said I needed donor eggs, I might not have done it." DONOR INSEMINATION PATIENT
What if we're offered a brand-new treatment?
Infertility treatment is rapidly evolving. As doctors learn of promising new procedures or ways to alter older ones, they are often eager to introduce the innovations to their patients. Sometimes a technique is offered before doctors have much experience in performing it, and even before the procedure's value is known.
If there is not evidence from research studies that a procedure is safe and effective, a program should offer it only as part of a research project. An ethics committee should have reviewed the project to ensure that participants are informed and protected as much as possible. The doctor should give you detailed informed consent documents so that you understand what the treatment involves, its experimental nature, and the possible risks and benefits.
Many treatments require a great deal of technical skill. If published research has documented the value of a new procedure in the hands of some practitioners, that doesn't necessarily mean that others will obtain the same results. When a program first introduces a new procedure, it is recommended that it be offered as part of a well-controlled research study until the program's doctors have a track record in using it.
If you are offered a new treatment, be sure you have answers to these questions:
- What is the evidence that it is safe and effective?
- At this point, would most doctors consider the procedure experimental?
- How long has the program been performing the technique?
- What have the results been?
- Will I be charged for the procedure?
- Could it make my chances worse instead of better?
- Will doing this technique lead to other changes in my treatment or prenatal care?
- Participation in research is entirely voluntary. If you decide against it, the program should provide a standard (non-experimental) treatment.
SURGERY
Until the development of IVF, surgery was the only treatment for blocked or damaged fallopian tubes. Surgery may also be recommended to remove scar tissue, fibroids or endometriosis from a woman's reproductive organs. In men, surgery may be suggested to open blocked passages in the reproductive tract or to treat varicose veins in the scrotum.
The goal of most reproductive surgery is to make it possible to conceive without IVF. Since the advent of IVF, reproductive surgery is recommended less frequently because it is less likely to lead to a successful pregnancy. A program that offers a variety of treatment approaches may be in an ideal position to help you evaluate whether to pursue surgery, other types of treatment, or no treatment at all.
Reproductive surgery has many variations, including endoscopic surgery, laser surgery and microsurgery. Each approach has strong advocates and detractors among infertility specialists.
Endoscopic surgery involves inserting a telescope-like laparoscope through a small incision in the abdomen or a hysteroscope through the cervix. This makes it possible to avoid major abdominal surgery and speed recovery. Laser surgery substitutes a laser for a traditional scalpel, but has not proven to be significantly better. Microsurgery uses several techniques (viewing the area under magnification, stitching with delicate sutures) to minimize damage to healthy tissues.
Should I undergo surgery?
Some questions you may want to ask about reproductive surgery and its variations are:
- Why are you recommending this approach?
- What will the recuperation be like? How long will it take?
- How soon can we start trying to conceive?
- What are the chances of conception after surgery? If a success rate is given, find out what period of time it covers. Typically, a postsurgery success rate is based on pregnancies achieved within a year or two of the procedure.
In contrast, most IVF success rates are presented on a per-cycle basis. Make certain that the success rate you are given refers to full-term pregnancies and is not just a measure of surgical success (such as an open tube).
- Does anything about my condition make it more or less likely that surgery will succeed? For example, a tube blocked in several places is far less likely to be opened effectively.
- If the surgery doesn't work, what would be my next option? What are the advantages and disadvantages of proceeding directly with that option instead of doing surgery?
- Are other types of surgery used for this problem?
- Are any non-surgical treatments used for this problem?
- How do the results compare?
Insist on an appropriate infertility work-up for both partners before proceeding with surgery. You don't want to undergo surgery only to discover that an unrelated problem (for example, male factor infertility or failure to ovulate) will make it difficult to conceive without another type of treatment that could have been used in the first place.
What if my partner or I have been sterilized?
Sometimes a tubal ligation or vasectomy can be surgically reversed. The chance of success depends on what type of procedure you had, how long ago, and other factors related to fertility in both of you (such as age). In some cases, a doctor might recommend using IVF rather than a surgical reversal to help you have a baby.
Fertility drugs
Each month, the ovaries normally mature one egg, releasing it in the middle of the menstrual cycle at ovulation. The general term "fertility drugs" usually refers to medications that influence this process. Fertility drugs can be used to spur ovulation in a woman who ovulates only irregularly or not at all. In addition, the drugs are often prescribed in order to cause several eggs to mature in a single cycle. This may be done to improve the odds of conception during intercourse or in conjunction with other treatments (such as intrauterine insemination or IVF).
Should I use fertility drugs?
Make certain that you understand the possible advantages and disadvantages.
It can be helpful to discuss these questions with your doctor:
Why are you suggesting fertility drugs in my case? Sometimes they are prescribed to women who do not ovulate regularly. However, they are frequently prescribed to women who do ovulate normally (especially those with unexplained infertility) in the hope that the drugs will increase the chance of conception.
How will the drug affect my chance of getting pregnant? While helping with ovulation, some fertility drugs have side effects that can actually make it more difficult to conceive and establish a pregnancy.
How will I take the medications? Some are taken orally. Others must be given by injection (in some cases, just under your skin; in others, into the muscle).
How am I likely to feel while using the medications? Some women find that these powerful hormones alter their moods, ability to concentrate and physical well-being. These influences, coupled with the time demands of monitoring your body's response to the drugs, can have a major impact on your daily routine and relationships. Although every woman's response is unique, it can be helpful to speak with others who have used the medications.
What are the risks? Fertility drugs sometimes result in serious medical complications. In the short term, the most serious is ovarian hyperstimulation syndrome, in which the ovaries become swollen and painful and there can be a dangerous buildup of fluid, at times requiring hospitalization.
"In all my hormone only cycles, I would hyperstimulate, sometimes worse than others. I would have to be on bedrest and a couple of times in the hospital so they could watch the fluid around my lungs." INFERTILITY PATIENT
If I get pregnant, what impact will the drugs have? Pregnancies achieved using certain fertility drugs are somewhat more likely to miscarry. In addition, most fertility drugs are associated with an increased risk of multiple pregnancy. Before beginning treatment, educate yourself about the risks of multiple pregnancy and the choices that you may be asked to make during pregnancy (see risks). Discuss these concerns with your doctor before taking the medications.
Are there any long-term risks to my health? A few studies have suggested that using fertility drugs, particularly for an extended period of time (in one study, for more than 11 cycles), may increase a woman's lifetime risk of developing ovarian cancer. Although data from recent studies are more reassuring, recognize that there are still unanswered questions about the long-term risk of using fertility drugs.
"You have to sign a big long consent concerning the retrieval, but there is a lack of any discussion about the use of the drugs. Pumping yourself with hormones has a tremendous impact on your body and emotions." UNSUCCESSFUL IVF PATIENT
Can the safety of fertility drugs and the likelihood of pregnancy be enhanced?
Yes, if you and your doctors work together to use the drugs properly. First, be sure that you are being monitored properly. Injectable fertility drugs should be used only if you are under the care of a doctor who has the experience and equipment to track your response using blood tests and ultrasound. Follow any instructions you are given. If too many follicles seem to be developing, you may be asked to stop using the medicine and refrain from attempting a non-IVF pregnancy in that cycle.
Second, make sure your care is re-evaluated at appropriate time intervals. Fertility drugs are not designed for use on an ongoing basis. No fertility drugs should be used cycle after cycle without the doctor evaluating how you are responding and whether a different dose, medication or procedure might work better.
Intrauterine Insemination
In intrauterine insemination (IUI), a health professional places specially prepared semen into a woman's uterus near the time she is ovulating. IUI can be used to bypass a problem preventing sperm from reaching an egg - for example, if the sperm do not get through the cervix into the uterus. In other cases, there is no known barrier to the passage of sperm, but IUI is suggested in an attempt to increase the odds of conception. IUI is often used in combination with fertility drugs.
Depending on the situation, IUI may be performed with semen collected from the male partner or frozen semen from a donor.
Should I use IUI?
Before undergoing IUI, make sure you clearly understand its benefits and risks. Ask your doctor the following questions:
Why are you recommending IUI in our case?
While there may be a specific diagnosis, the combination of fertility drugs and IUI is often suggested to couples with no known problem. Couples are sometimes advised to try a few cycles of this less expensive treatment before undergoing IVF.
How and when will the semen be collected?
If the male partner's semen is used, it is usually collected by masturbation shortly before the procedure. If you have concerns about this method of collection or your partner's availability, discuss these with the doctor. It may be advisable to freeze a specimen ahead of time, and alternative methods for semen collection may be available.
How successful is the procedure in couples similar to us?
How does it compare to our chances if we just time our intercourse well at home?
Success rates for IUI may be given for a single cycle or may be based on performing the procedure over several months. Make sure you know which statistic is being used. In general, IUI is not a recommended treatment for poor semen quality, and it will not overcome an age-related decline in a woman's ability to produce eggs.
Do you recommend the use of fertility drugs in conjunction with insemination?
If so, thoroughly consider their advantages, risks and costs before making your decision.
What are the alternatives to IUI?
Depending on your condition, your options might involve less medical intervention (advice on timing intercourse at home), more intensive treatment (IVF), or the use of donor semen. Learn the advantages and disadvantages of each option before making a decision.
In Vitro Fertilization
In vitro fertilization, or IVF, is a method of treatment in which the man's sperm and the woman's eggs are combined outside of the body. In general, IVF involves five steps:
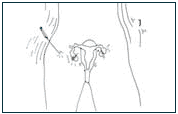 1) A combination of medications is used to stimulate the woman's ovaries to mature many eggs in one cycle, a process called controlled ovarian hyperstimulation.
1) A combination of medications is used to stimulate the woman's ovaries to mature many eggs in one cycle, a process called controlled ovarian hyperstimulation.
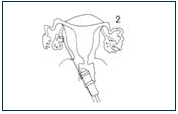 2) The mature eggs are removed from the woman's ovaries - usually through a slim needle inserted through the wall of the vagina.
2) The mature eggs are removed from the woman's ovaries - usually through a slim needle inserted through the wall of the vagina.
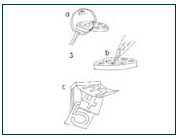 3) The eggs are examined and placed into a culture dish in the lab. At the proper time, they are mixed with specially prepared sperm. Later, if fertilization occurs, the resulting embryos are grown in the lab for a few days.
3) The eggs are examined and placed into a culture dish in the lab. At the proper time, they are mixed with specially prepared sperm. Later, if fertilization occurs, the resulting embryos are grown in the lab for a few days.
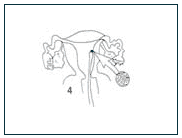 4) One or more embryos are transferred back into the woman's uterus, where an embryo may implant and result in an ongoing pregnancy.
4) One or more embryos are transferred back into the woman's uterus, where an embryo may implant and result in an ongoing pregnancy.
 5) A pregnancy test is given. If conception does not occur, all steps of the cycle should be evaluated by the treatment team and discussed with the patient in a follow-up meeting.
5) A pregnancy test is given. If conception does not occur, all steps of the cycle should be evaluated by the treatment team and discussed with the patient in a follow-up meeting.
Should I undergo IVF?
For most couples, whether or not to undergo IVF is a major decision that requires them to assess many medical, emotional and financial factors. Before deciding, you may want to speak with others who have gone through the process (successfully and not), an infertility counselor, and/or a support group. These are a few of the questions to discuss with your doctor:
- Why are you recommending IVF for me?
- What are my alternatives to using IVF?
- What are the risks of each step in the process?
- What is it like for most women as they go through each step? (This will help you predict what the impact may be on your time, physical well-being and emotions).
- What is my chance to become pregnant and deliver a baby as a result of this treatment?
- How does that compare to my chances with other treatments or no treatment at all?
"The waiting rooms are filled with people whose total life is going through these programs. It was hard to juggle working and IVF, but I'm glad I didn't just sit there for a month." IVF PATIENT
What are the alternatives to IVF?
Depending on your fertility problems, you may decide to use lower-tech treatments or no treatment at all.
In addition, two IVF alternatives are available at some programs, although their use has declined greatly. In gamete intrafallopian transfer (GIFT), the first two steps are the same as IVF. But, instead of fertilizing the eggs in the laboratory, a mixture of sperm and eggs is placed into one or both of the woman's fallopian tubes. In GIFT, fertilization and the embryos' travel to the uterus occur in the natural environment of the fallopian tubes. GIFT usually involves a surgical procedure and requires that at least one of a woman's tubes be open and healthy. Because general anesthesia is usually required, GIFT is considered riskier and usually costs more than IVF.
Another procedure, zygote intrafallopian transfer (ZIFT), combines elements of IVF and GIFT. The first three steps are similar to IVF. However, instead of transferring the embryos into the uterus, they are placed into one or both of the woman's fallopian tubes.
The general term assisted reproductive technologies (ART) is used for all treatments that involve removing a woman's eggs and combining them with sperm outside the body, including IVF, GIFT and ZIFT.
Once we agree to undergo IVF, what decisions need to be made?
IVF is not a uniform treatment. To carry out a treatment cycle, several decisions must be made, including:
- What dose of fertility drugs to use
- When to retrieve the eggs
- How long to culture the embryos before inserting them into the uterus
- How many embryos to transfer to the uterus in a cycle
- Whether to freeze embryos for later cycles
Make certain that you understand the impact these choices could have on your chance of pregnancy and on treatment decisions you may be asked to make later on.
What additional treatments or procedures may be recommended?
Depending on your condition or your response to previous treatments, variations on IVF may be suggested. Each adds cost and certain risks. Success depends greatly on the expertise of the lab personnel who will be manipulating the eggs, sperm and embryos. Be sure you know your program's level of experience, as well as the pros and cons of using any of these procedures in your case:
Intracytoplasmic sperm injection (ICSI) is used to increase the chance of fertilization. Instead of mixing sperm and eggs and waiting for fertilization to occur, a single sperm is injected directly into each egg.
Assisted hatching is used to increase the chance that an embryo will implant in the uterus. A small opening is created to make it easier for the developing embryo to emerge from the protective shell that surrounds it.
Blastocyst transfer is used to maximize the chance of pregnancy while minimizing the risk of a multiple pregnancy. Instead of transferring embryos after two or three days in the lab, they are grown to the many-celled blastocyst stage and transferred on day five. By this point, surviving embryos have a higher chance of establishing a pregnancy, so fewer need to be transferred.
How can I find out where I'll have the best chance to have a baby?
Consumers considering IVF now have a new tool to help them learn where they may have the best chance to have a baby. Each year, the federal Centers for Disease Control and Prevention (CDC) publish the outcomes of IVF and related procedures. These include both national averages and clinic-by-clinic results. The national averages can provide a general ballpark idea of how well IVF works in people your age or with your diagnosis. If the chance of success seems unacceptably low, you may want to pursue other methods of building your family. If the chances seem reasonable, you can check the individual results for any clinic you are considering.
"Going into treatment, I hadn't realized the huge amount of variation in success rates. It's pretty phenomenal. Although IVF patients, on the whole, tend to be better educated, many are unaware of success rates and select a program based on convenience, location, and who their initial doctor referred them to." SUCCESSFUL IVF PATIENT
You can obtain this important resource through the Web sites of RESOLVE or the CDC (see Resources). Any program that you contact should be willing to give you a summary of their results from the latest report, along with their individual assessment of your case. The CDC also publishes a list of programs that have not submitted their results. Keep in mind that the availability of published success rates for IVF does not mean that it would necessarily be the most successful or most appropriate treatment for you.
Should I go to the program with the highest CDC success rates?
Not necessarily. It helps to understand a clinic's success rate before you sign up for treatment. However, it may not be the only - or even the most important - way to determine which IVF program is right for you.
As you evaluate the CDC's statistics, keep these factors in mind:
- Small differences can occur strictly by chance and are not meaningful when comparing programs or tracking how a program's success has changed from year to year.
- Published rates are not current. The results of IVF cycles performed in a given year can't be collected and analyzed until all the resulting pregnancies are completed. This means a time lag of about two years by the time results are published. Keep in mind that doctors and lab personnel could have changed since the latest published data. Make sure you have the information you need about the experience and track record of the current staff.
- The best rates may not apply to you. Look at the national rates for those in your age group. Even within categories, there can be major differences in outcome. For example, since the chance of pregnancy declines steadily after women are in their mid-30s, if you are 40 years old, the pooled results for women 38-40 will likely overestimate your chance of success.
If you need a specialized procedure, such as ICSI, check on the program's experience with that procedure.
- Note the number of embryos transferred and the rate of multiple births. For some programs, more than half the deliveries involve two or more infants. Also, check the percentage of pregnancies that involve twins or other multiples. For some programs, more than one-fourth of IVF pregnancies in younger women involve three or more fetuses. Some programs attempt to increase their published success rates by transferring many embryos in each cycle. This means that more of their patients will have to decide between carrying a high-risk multiple pregnancy and undergoing fetal reduction.
"Success rates weren't that important. I just asked around what the best place was." SUCCESSFUL IVF PATIENT
- Programs differ in their willingness to accept the tough cases. A program that takes more difficult cases may provide equal or better treatment than a program that posts a high success rate but only accepts those most likely to conceive. Likewise, if a program advises no treatment or lower-tech options to couples with milder problems, it may serve patients better than a program that obtains a high success rate by using IVF on couples who might conceive without it.
- Ask about complications. The success rates don't tell you how many women needed hospitalization or how many infants were born prematurely or died shortly after birth.
- Ask how many cycles your doctor would recommend you consider.
- Ask what percentage of cycles are canceled and why. Programs differ greatly in how many treatment cycles are canceled (an average of 14 percent, but ranging from less than 1 percent to more than 40 percent), often because of a poor response to fertility drugs.
- Pay attention to a program's success using frozen embryos. Many IVF cycles are conducted with the intention of freezing excess embryos to use in a later cycle, if needed. How well those cycles work may have a large impact on whether you become pregnant
"We checked around and found the chances were slightly higher at one program. We knew and liked the doctor at the other program in town, so it was a very difficult decision. But we picked the one with better numbers." WOMAN PREGNANT AFTER TWO IVF CYCLES
Can I rely on the success rates published in advertisements?
It can be tricky to decipher the reality behind some ads. If a success rate is given, look for how they define success and how they define an attempt (see "Success Rates"). To avoid misleading people, both the Society for Assisted Reproductive Technology (SART) and the Federal Trade Commission (FTC) recommend that programs report data on live births.
If a program is comparing its results to those of another program, they should use the same definitions. SART requires its members to support any advertising claims they make with reliable data. It no longer permits programs to make comparisons with other programs in their ads.
Remember, there may be important reasons other than quality for the rates at programs to differ, such as the patients they select to treat. The results being advertised may not have been achieved on patients similar to you. And, don't give much weight to ads touting statistics collected over only a few months. Any program can have a brief run of pregnancies that inflates the short-term success over their usual rate.
Not all advertising is clearly labeled. If a program hands out videos or books, or offers informational seminars, its aim may not be just to educate but to attract new clients. The information presented will reflect that program's point of view about who should seek care and the most valuable tests and treatments. This information may or may not correspond with scientific evidence and the opinions of experts in the field. Consider the source of these materials as you evaluate their content.
If you feel that advertising for a fertility program has been deceptive or misleading, report it to your state or local office of consumer affairs, or to the FTC (see Resources).
DONOR SEMEN, EGGS AND EMBRYOS
Who uses donors?
Couples use donor semen to create a pregnancy in cases of male factor infertility or to avoid transmitting a genetic disease. It may also be used by women who wish to become pregnant without involving a male partner. When there is severe male factor infertility, couples are most commonly offered a choice between using donor semen and using IVF with ICSI. IVF with ICSI can be extremely costly. Using donor semen is far less invasive and less expensive, but means that the man will not be the genetic father of the baby.
Donor eggs may be used in IVF when a woman wants to avoid transmitting a genetic disease or no longer produces usable eggs, often because she is approaching or has entered menopause.
In recent years, it has become apparent that, after the age of 35, women's pregnancy rates using standard IVF begin to fall. In IVF using donor eggs, the pregnancy rate corresponds to the donor's age. With supplementary hormone treatment, many women in their 50s (and some who are older) have given birth through this process. When donor eggs are used, the recipient is the birth mother, but not the genetic mother, of any resulting children.
"In the back of my mind I think about doing a donor egg cycle, but it's a big step to take." UNSUCCESSFUL IV PATIENT
About half the nation's fertility programs now offer the relatively new option of having a donor embryo transferred into a woman's uterus - after she receives medications to prepare her uterus to receive it. Although the woman would be the birth mother, any resulting children would not be genetically related to her or her male partner. Donor embryos might be used when there is both male and female infertility, by couples who wish to avoid transmitting a genetic disease, or as a possibly less costly alternative to a complete IVF cycle.
Where does donor semen come from?
Frozen donor semen is generally purchased from a semen bank. Some infertility programs have their own semen banks. Other semen banks are independent and may sell semen specimens to doctors all over the country. Each semen bank selects its pool of donors. It is important for you to understand how they recruit and screen the donors, and what information they make available to recipients. Any semen bank providing specimens for use in New York State must be licensed by the state and adhere to its guidelines.
Where do donor eggs come from?
Unlike donor semen, which can be frozen, typically donor eggs are collected and used immediately. Most egg donors are young adult women who are recruited and screened by fertility programs. Donors undergo the required medical procedures (taking fertility drugs, monitoring, and egg retrieval) at the same program as the recipient.
In addition, some independent companies or agents recruit and arrange for the screening of potential egg donors, but do not provide medical services.
It is important for you to be comfortable with how your egg donor has been selected and screened, and how she will be treated by the program.
Most programs allow the use of known donors, if they fit the program's eligibility standards. If you have a friend or relative who could serve as your egg donor, ask the program about this option.
Any program providing donor eggs for use in New York State must be licensed by the state and adhere to its guidelines.
Where do donor embryos come from?
Donor embryos have usually come from couples who created and froze extra embryos during their own treatment but no longer wish to use them. Any program providing donor embryos for use in New York State must be licensed by the state and adhere to its guidelines. These require embryo donors to be screened as thoroughly as semen or egg donors.
Can infectious diseases be passed through donor semen?
Yes. Like other human tissues, semen can harbor bacteria and viruses that can cause illness in the recipient. For this reason, it is essential that semen donors be regularly tested for a variety of infections.
A man may not test positive for antibodies to HIV (the virus that causes AIDS) until several months after he is exposed. For that reason, donor semen should be frozen for at least 180 days and not released for donation until the donor tests negative a second time.
Make sure you are satisfied with the precautions taken by your semen bank to prevent the transmission of infectious diseases.
Can infectious diseases be passed through donor eggs?
Although no cases have been reported, it is theoretically possible that an infection could be passed through a donor egg. Most programs test egg donors for the same infections as semen donors.
With donor eggs, freezing is not practical at this time. This causes special concern with regard to HIV testing, since a woman may not test positive for antibodies to the virus until several months after she is exposed.
Eggs cannot be stored until a donor passes a second HIV test. This means that a recipient must rely on an egg donor's current HIV test results or have the embryos frozen to use after the donor is retested. Most recipients of donor eggs accept the small possibility that a donor might have been recently exposed to HIV and could transmit the virus through the donor egg. Some programs take the additional precaution of requiring HIV testing for the sexual partner(s), if any, of prospective egg donors.
Can donor semen or eggs result in birth defects or inherited diseases?
Yes. If a donor has a genetic disease, or is healthy but carries a gene associated with a genetic disease, it can be transmitted during semen or egg donation.
Some semen banks and egg donation programs take thorough genetic histories and perform many genetic tests on all donors. Others test only for common genetic diseases or those required by state regulations. Many genetic abnormalities cannot be detected through existing tests. Before starting treatment, make certain you are satisfied with the extent of planned donor screening and testing.
Tell your doctor about any genetic diseases that are present in your family or are more common in your ethnic group. This might include sickle cell disease in those of African heritage or Tay-Sachs disease in French Canadians or people of Ashkenazi Jewish heritage.
If you are uncertain about your family history or the likelihood that you carry an inherited disease, you may wish to seek genetic counseling before proceeding. For assistance in finding a genetic counselor, contact your doctor or the National Society of Genetic Counselors (see Resources).
What if my egg donor develops medical complications?
Egg donors undergo the first two steps in the IVF process (the use of fertility drugs and retrieval of eggs). Donors occasionally develop complications from fertility drugs or the procedure to remove the eggs. Rarely, these are serious enough to require hospitalization. Before you agree to undergo treatment using donor eggs, review the information and consent forms your donor has received to make certain you find her treatment acceptable.
Clarify who has the financial responsibility if your donor develops complications. At most programs, the recipient must agree to pay all expenses.
What will we know about the donor?
Semen banks and egg donor programs vary in how much information they make available to recipients. Some supply only a few details to use in matching (race or ethnic background, height and weight, blood type, etc.). Others provide - sometimes for a fee - far more biographical information and test results. Although these details may help you to feel that you know your donor better, experts caution that there is little evidence such characteristics are inherited.
"They say it's anonymous. But the profile told a lot more than I would have expected, including the place of birth, the year, the nationality, and that he has a sister. I'm not complaining, but I think I could find this person." WOMAN ATTEMPTING DONOR INSEMINATION
At a minimum, be certain you have enough medical information to choose an appropriate donor. For example, if you carry a recessive genetic disease (such as cystic fibrosis, sickle cell anemia or Tay-Sachs), then you need to be certain your donor has been tested and found not to be a carrier.
Can we meet our donor?
It depends on the program. A few semen banks and egg donation programs specialize in helping donors and recipients who want to know each others' identities and arrange for some level of contact.
Can we use the semen or eggs of a relative or friend?
Sometimes. In New York State, a known donor is subject to the same State Health Department regulations as an anonymous donor. A known donor's semen must be collected, prepared, frozen and stored for six months by a licensed semen bank until he re-passes tests for HIV and other infectious diseases. Because of the risk of genetic disease, a woman can not be inseminated with the semen of a close blood relative.
At some programs, a woman may bring in a friend or relative to serve as an egg donor. This woman must undergo the same screening as other egg donors, and the program will want to take precautions to ensure that she understands the medical risks and other issues.
Because of the risk of genetic disease, the donor can not be a close blood relative of the intended father. In order to ensure that a woman does not feel pressured to donate because of her emotional or financial ties to the recipient, some programs place restrictions on the relationships they allow. For example, some programs do not permit an employee or young adult daughter of a woman to become her egg donor.
In addition to the medical issues raised by using a known donor, you must consider the many legal and psychological issues that can emerge at a later date. For example, will you tell your child that his uncle is actually his biological father, or that her older sister is genetically her mother? What would you do if a friend/donor suddenly wanted to be recognized as your child's parent?
Should we tell our child we used a donor?
It is up to you. Historically, families were not encouraged to tell children that donor semen was used in their conception. Today, however, many parents and health professionals advise giving children this information.
They cite evidence that secrecy within families can be harmful, and stress that children may someday need medical information about the donor.
With more families using donor semen, eggs and embryos, there is an increasing amount of support for informing children of their genetic origins. At this point, however, there is a lack of follow-up information on children to help in making this decision. A counselor can help you decide what to tell your child. Counselors at some infertility programs offer support to parents as they ponder whether, when and how to best explain these issues. In addition, organizations such as RESOLVE offer member contact systems for those who are considering or have built families through donor conception (see Resources).
"Somebody at day care said, 'Where's [Neil's] daddy?' I said, 'I don't know.' They said, 'What does he look like?' I said, 'Brown hair and blue eyes.' That's pretty much all I know." SINGLE WOMAN WHO HAD A CHILD THROUGH DONOR INSEMINATION
Should we tell our relatives and friends we're using a donor?
It is entirely your decision. However, many who have used donors strongly advise you to tell others only if you plan to inform your child.
"We've said at this point we won't tell him unless there is a clear reason to do so, and it has to be agreed upon by all involved. My parents do not know. I haven't gone out of my way to find other infertile couples for support, and that comes largely from the decision to keep the egg donation private. It's somewhat alienating." WOMAN WHO GAVE BIRTH TO A CHILD CONCEIVED WITH A DONOR EGG
Is my child likely to meet other children who are blood relatives through the donation?
Probably not. Any other child conceived using semen or eggs from the same donor is a genetic half-sibling of your son or daughter. If you received a donor embryo, your child is genetically the full brother or sister of others conceived from embryos created with the same semen and eggs. Your child is also the full sibling of any other children of the couple who donated the embryos.
The possibility that your child will meet his or her genetic siblings depends on how many children have been born using the same donor.
Under New York State regulations, licensed semen banks and egg or embryo donation programs are required to consider this possibility. They must set reasonable limits on the number of pregnancies allowed using each donor. However, there are no absolute rules in this regard and the risk can only be reduced, not eliminated. If you are considering using donated eggs, semen or embryos, ask if the program places a limit on how many times the same donor is used, and whether eggs (or embryos) are ever shared by more than one recipient.
In many religions and societies, sexual relations between close blood relatives is a serious taboo. In addition, when close relatives reproduce, they are at increased risk of delivering a child with a genetic disorder. This is one reason some couples choose not to use donors. It is also one rationale for informing a child that a donor was used in his or her conception.
That way, if the child is considering becoming involved with someone else conceived using a donor, he or she can check medical records or seek medical testing to ensure that they are not related.
Can our donor find out who we are?
If you are using a commercial semen bank, the donor should not have access to your identity. In fact, he is unlikely to know whether anyone got pregnant using his semen. Programs differ in how much they tell egg donors about the outcome of their donations. Ask about this before you select a semen bank or egg donation program.
What if my child needs medical information about the donor, or just wants to learn his/her identity?
If the semen bank or donor egg program you use follows the guidelines of the American Society for Reproductive Medicine, it will keep a record of the donor's genetic information and other non-identifying information. If needed, you or your child can obtain this information, but not to find out who the donor was (unless the donor gives permission).
At some semen banks and egg donation programs, you have the option to select a donor who has stated a willingness to be contacted (often after a child has reached adulthood). For some couples, whether or not this permission has been granted is an important factor in selecting a donor.
"They did say he's a very popular donor. I thought, I'll have to move out of the area - what if his kids meet each other?" DONOR INSEMINATION PATIENT
Will I be the legal mother if my baby was created with a donor egg?
As the woman who gives birth, it is highly unlikely that anyone would ever challenge your status as the legal mother of the baby. However, the issue has been raised in a few custody disputes between a birth mother and her husband or partner. In these cases, the father argued that he should have greater rights because he has a genetic link to the child that the mother does not. If a question arises, it would be decided in accordance with state law. Laws in several states make it clear that the birth mother, and not the egg donor, is the legal mother.
Under New York State law, a birth mother - whether or not she is also the genetic mother - is the legal mother unless she later gives up her parental rights. However, the use of donor eggs by unmarried women is not specifically mentioned in the New York laws.
Will my husband be the legal father if we use donor semen?
By law in most states, your husband will be considered the baby's legal father, with all the rights and responsibilities that brings. To ensure this, ask about the law in your state and make certain that you have followed its requirements. In some states, such as New York, the husband must give written consent for the insemination and it must be performed under the direction of a licensed doctor.
"We are not at liberty to know whether our eggs worked out or not. I imagine everything worked out beautifully, because they asked me to do it again. It would be comforting to have the information, but it could get out of hand. I don't need to know anything about the recipient." EGG DONOR
What if a semen donor comes back and wants the baby?
The chance that an anonymous semen donor will learn who you are and seek to become your baby's legal father is extremely small. If an anonymous semen donor ever sought custody of a child resulting from the donation, his rights would depend on state law. You need to understand the law in your state and any provisions you must follow to preserve your rights. Some states make it clear that men forfeit all their parental rights and responsibilities for resulting children when they become semen donors. In New York State, there is no provision for a semen donor to give up his rights when the semen is used to inseminate an unmarried woman.
THE USE OF SURROGATES
What if I can't carry a pregnancy?
If it is impossible or unsafe for the woman to carry a pregnancy, some couples enlist the help of another woman to fulfill this function. This "surrogate mother" becomes pregnant with the explicit intention of giving the child to the couple after birth.
Often, she is paid for her services and all expenses.
There are two types of surrogacy. In one type, a woman becomes pregnant through artificial insemination. The surrogate is both the genetic mother and the birth mother of the child. In gestational surrogacy, an embryo created by the intended parents through IVF is transferred to the surrogate's uterus. The gestational surrogate is the birth mother but not the genetic mother of the child.
In New York and some other states, it is illegal to enter into a surrogate parenting contract that requires a woman to give up an infant and her maternal rights in exchange for money. If an arrangement with a surrogate does not involve payment (other than for the surrogate's medical expenses), ART practitioners are allowed to provide the necessary medical services. However, they cannot protect you if things do not go as planned after the birth. If a surrogate changes her mind and refuses to give up the child, she maintains the same rights as any other birth mother. The result could be a dispute between you and the surrogate over custody of the child.
If you are considering the use of a surrogate, be aware that you are entering an area of significant legal and financial risk in New York State. Other states have different laws pertaining to gestational surrogacy and the rights of the genetic parents and birth mother. Seek knowledgeable legal advice before proceeding.
THE ISSUE OF MULTIPLE BIRTHS
Why are so many twins born after infertility treatment?
Certain drugs and procedures greatly increase the chances of multiple births.
For example, clomiphene citrate results in an 8-10 percent twin rate in those who conceive. This drug usually is not associated with births involving three or more fetuses. Injectable fertility drugs (such as human menopausal gonadotropins or folliclestimulating hormone) may result in many eggs maturing within a single menstrual cycle. About 15 percent of pregnancies induced by these hormones result in twins. Five percent involve three or more infants. The risk depends on the dose, the patient's diagnosis and her response to the hormones.
In an IVF cycle, more than one embryo is usually transferred into the uterus to increase the likelihood that at least one will implant. However, whenever more than one embryo is transferred, there is the possibility of a multiple birth. According to recent CDC statistics, transferring two or three embryos increases the chance of pregnancy - as well as the chance of twins or triplets. Pregnancy rates decline when four or more embryos are transferred, but the chances of multiple births stay high.
"Some of the information I was naive about - like the multiple birth risks. After they found out it was triplets, they mentioned fetal reduction but didn't have a lot of information. The obstetrician gave us more information about the risks, saying we could lose them all, and that kind of scared us." MOTHER OF PREMATURE TRIPLETS WHO DIED SHORTLY AFTER BIRTH
Is pregnancy more risky with multiples?
Yes. The more fetuses, the higher the risk of complications to both mother and babies. A woman pregnant with multiples is more likely to miscarry, to develop high blood pressure, diabetes, or anemia, and to have her uterus rupture or her placenta detach prior to delivery. She is more likely to go into early labor, which requires medical treatment (with its own side effects) and often means hospitalization and prolonged bedrest.
Despite treatment, delivery usually occurs four weeks early for twins, eight weeks early for triplets, and ten weeks early for quadruplets. After delivering multiples, a woman is at increased risk of serious bleeding.
If twins or triplets are OK with us, what's the problem?
Only you know whether you are prepared to raise two or more children - which means caring for two or more infants - at once. But it is important to realize that children from multiple births have a much higher chance of prematurity and low birthweight. Premature babies may suffer from several long-term medical problems that require extraordinary care or may even result in early death. Low-birthweight and premature babies are more likely to need prolonged hospitalizations after birth and to develop cerebral palsy, mental retardation, blindness and deafness than normal-weight infants.
As one example, consider the chance that a baby will die before it is one month old. According to national statistics (not all involving IVF), compared with a single baby, early death is four times as likely in twins, 10 in triplets, 13 in quadruplets, and 30 in quintuplets. More than half of all twins and nearly all newborns from pregnancies involving three or more babies are low-birthweight, with some born dangerously tiny and premature.
When results are reported after IVF or GIFT, a live birth means at least one infant showed signs of life after delivery. It does not tell you whether any or all of the infants survived or went home from the hospital in good shape.
Can multiple births be prevented?
Since the early 1980s, there has been an astonishing rise in multiple births. About two-thirds of the increase is thought to be the direct result of fertility therapies, including the use of fertility drugs and IVF.
Many of these multiple births can be prevented. Several countries in Western Europe, and also Australia and New Zealand have federal laws or regulations that limit the number of embryos that may be transferred during a cycle. For example, in the United Kingdom, doctors may transfer no more than three embryos in a cycle, and they are encouraged to transfer only one or two. In the United States, these decisions are left to the individual doctor and patient. However, prominent medical organizations, such as the American Society for Reproductive Medicine (ASRM) and the American College of Obstetricians and Gynecologists (ACOG), have called on doctors to make the prevention of multiple births a high priority as they plan fertility therapy (see Resources). In the interest of preventing the maternal and infant complications stemming from multiple births, a responsible doctor will:
- start with the lowest dose likely to develop enough eggs for an individual patient, including frozen IVF cycles.
- use injectable fertility drugs only if they can provide careful ultrasound and blood hormone monitoring can be provided.
- not give drugs to induce ovulation if hormone levels are too high or if ultrasound shows that too many follicles are maturing; and will counsel patients not to have unprotected intercourse during that cycle.
These restrictions are especially important if the cycle involves IUI or drugs alone (rather than IVF) or in an IVF cycle in which freezing is not planned.
- limit the number of embryos transferred in a single IVF cycle and eggs transferred in GIFT.
"The issue was discussed and discussed up front. They said they limit transfers to four embryos and said that three might be more appropriate for me. I decided three would be maximum." DONOR EGG RECIPIENT
Although decisions about how many embryos to transfer must depend on the individual patient and program, the ASRM advises that, usually, no more than two good quality embryos should be transferred in women under 35 (who have extras to freeze) and no more than three in women under 35 without frozen embryos. For older women, the ASRM suggests that no more than four embryos be transferred to women between 35-40, and no more than five in women older than 40 or those who have already undergone many failed IVF cycles. In a donor egg cycle, the age of the donor is used to determine the number of embryos to transfer.
In a GIFT cycle, the chance of a multiple birth rises along with the number of eggs transferred back to a woman's fallopian tubes. However, since all eggs may not fertilize, ASRM guidelines permit one more egg than embryo to be transferred in each age category.
You share responsibility in reaching decisions and following medical advice aimed at reducing the chance of a high-order multiple pregnancy. Your doctor may recommend that a specific number of embryos or eggs be transferred, based on your diagnosis or past reproductive history. You have the right to ask your doctor to transfer fewer in order to lower the risk of a multiple pregnancy. If your doctor is not willing, seek treatment elsewhere. If you wish to have more eggs or embryos transferred than is recommended, your doctors are not required to comply. Doctors are not obligated to help create a situation that is likely to cause harm to a patient or any resulting children.
Can a multiple gestation be fixed?
If a woman becomes pregnant with many fetuses, she can be offered fetal reduction (also called multi-fetal pregnancy reduction). In this amniocentesis-type procedure, a lethal chemical is injected into one or more fetuses, leaving an agreed-upon number. The goal is to decrease the chance of miscarriage or premature delivery.
Fetal reduction lowers, but does not eliminate, the risks involved in multiple gestation. The procedure itself sometimes results in miscarriage. Many couples find it emotionally trying; some believe it is ethically unacceptable.
Before taking fertility drugs or pursuing IVF or GIFT, ask your doctor about the fetal reduction procedure. If you decide that fetal reduction is something you will not consider or wish to avoid, your doctor should know that and agree to provide treatment that will limit the chance of a multiple pregnancy.
Are some programs more likely to create multiples?
Yes. Despite recent calls for programs to reduce the number of multiple gestations they create, about 37 percent of the pregnancies and live births resulting from IVF and GIFT involve multiples, and about 8 percent of the pregnancies (and 5 percent of the births) involve three or more fetuses. Statistics reported to the CDC show a wide range in the average number of embryos that programs transfer in a cycle (in women under 35, from one to five). At times, high delivery rates are achieved by placing higher numbers of embryos, which result in high multiple rates.
As you look at outcome statistics, check a program's rates of multiple pregnancies, multiple deliveries and the average number of embryos transferred. Ask how often their patients undergo fetal reduction. Ask what they do to reduce the chance of multiples and what they are likely to recommend in your case.
"I remember once they said, 'We have five fertilized eggs and we're putting them all in.' I literally got off the table and made them discuss it." IVF PATIENT
FREEZING EMBRYOS
If all the embryos aren't transferred, what happens to them?
Before you begin an IVF cycle, you and your physician should agree on what will happen to any extra eggs or embryos. In most cases, excess embryos are frozen for possible use in a future cycle. However, other options are open to couples who do not wish to freeze embryos. Depending on the program, excess embryos can be discarded, donated for research or donated to another couple. Couples who object to all of these options can limit the number of eggs that are mixed with sperm. That way no extras can be created. However, no one can know with certainty how many eggs will fertilize or what the quality of the resulting embryos will be. Therefore, this option could significantly limit your chances of delivering a child.
In New York State, programs that freeze embryos must be licensed and adhere to state regulations on safety and recordkeeping. A program should not offer IVF unless they have the ability to freeze and store embryos.
Does freezing hurt the embryos?
Not all embryos survive freezing and thawing. The proportion of embryos that will be usable after freezing can be difficult to predict. Program and patient factors (such as age and diagnosis) can affect embryo quality. Embryo quality differs from cycle to cycle. Embryos created during the same cycle may also vary widely in quality. If those appearing to be of better quality are transferred in the initial cycle, those that are frozen may be less likely to result in pregnancy. This is not a result of freezing per se, but reflects the initial selection.
How long can I wait to use the embryos?
Some programs will keep frozen embryos indefinitely if you continue to pay the storage fees. Others limit the time embryos may be stored. At that point you may need to transfer the embryos to another facility or select a different option for their use or disposal.
According to the available evidence, how long embryos are stored does not seem to affect their quality.
If I never use the frozen embryos, what will happen to them?
Depending on the program, you may be offered any or all of the following options:
- You can allow the program to donate them to another couple. In New York State, because of the risk of transmitting infection through the embryo, you may donate your embryos only if you undergo the same testing as semen or egg donors.
- You can allow the embryos to be thawed and discarded.
- You can donate the embryos for use in medical research.
Couples can have strong preferences or religious and ethical concerns about any or all of these choices. Make sure that you are comfortable with the choices offered and be sure to express your wishes, in writing, before embryos are frozen.
Who is allowed to make decisions about the embryos?
Although a fertility program may have custody of your embryos, in most circumstances program staff can not make decisions about their use without your consent. When embryos are created by a couple (whether or not donated eggs or semen were used), the couple usually retains joint decision-making authority over the embryos.
Before freezing any embryos, make note of what you are required to do while your embryos are stored. You must keep the program informed of your intention to continue storage or to have the program carry out your instructions for disposing of the extras. If you decide to change your instructions, inform the program in writing.
"It's weird to go through all the scenarios. After everything you've been through, it's hard to think about what could happen to the embryos." IVF PATIENT
What if we get divorced or one of us dies?
Serious questions and disagreements could arise if you divorce or if one or both of you die or become incapacitated. It is important for you to think about these possibilities before you begin treatment. To the extent possible, you should indicate - in writing - what you would want to happen to the embryos in case of death or divorce.
In some states, these documents may be legally binding unless both of you agree to change them.
When disagreements arise, courts have taken various approaches in deciding who, if anyone, has the right to use the embryos over the other's objection or what should happen in unforeseen circumstances. This is likely to be an area of ongoing legal uncertainty.
Paying for Infertility Treatment
Return to TopWhat will treatment cost?
Infertility treatment can be extremely expensive. Depending on the type of treatments and how long they last, your out-ofpocket costs will vary.
In order to minimize the unexpected costs, be sure to include these expenses (which may not be included in prices quoted on a per-cycle basis) in your estimates:
- Diagnostic tests
- Medication
- Monitoring
- Donor fees and medical bills
- Prenatal care costs
- Missed time from work and impact on career
- Lodging and transportation for treatment away from home.
The costs to treat medical complications - should they occur in you or a donor treated on your behalf - may be substantial, but they cannot readily be predicted in advance.
Will our insurance cover infertility treatment?
Many health insurance plans do not cover diagnosing and treating infertility. Among those that do, policies differ in what is covered and the limits and restrictions involved. It is your right to see the contract detailing exactly what is covered under your plan. Examine sections of the contract that list exclusions, procedures not covered, or limits of coverage. You may also write to your insurer requesting a predetermination of benefits. In your letter, give your diagnosis and the specific treatments (and their fees) that have been recommended. (Break down the treatments into components such as medications, laboratory tests, etc.)
While your insurance coverage may influence your choice of treatment, do not let it stop you from being fully informed about your medical options. Ask your doctor: "If my insurance covered all treatments, or if money were not an issue, would you make the same recommendation?"
"They estimated what the medication would cost, but the estimate was very, very low. It was almost $2000 more." SUCCESSFUL IVF PATIENT
Programs differ in the amount of help they provide in dealing with insurance companies. Some will submit claims directly. Others will not get involved. Some set their fees on a per-cycle basis. Others will provide itemized billing to aid those without full coverage in seeking partial reimbursement. In several states, the law requires that insurance companies offer a certain amount of coverage for infertility treatment. However, even if you live in one of these states, do not assume that your bills will be paid.
Some states require insurers to offer policies that provide coverage for infertility treatment, but also permit them to issue policies without such coverage. Your employer may or may not have chosen to include infertility coverage in your plan.
Some state mandates include unlimited cycles of IVF, while others limit the amount and type of treatment insurers must cover. In addition, if your employer or union is funding its own insurance plan, it is regulated by federal law (ERISA, the Employee Retirement Income Security Act), and state laws do not apply. Your employer can tell you whether you have an ERISA plan.
In New York State, insurance carriers are required to cover the diagnosis and treatment of correctable medical conditions. They cannot exclude coverage just because the medical condition results in infertility. However, insurance carriers are not required to cover certain procedures, including IVF. Insurance carriers must cover infertility drugs, as long as they are approved by the FDA for the diagnosis and treatment of infertility.
"We scrimped and saved all of our pennies. Until the pregnancy test, we had to pay for everything up front." SUCCESSFUL IVF PATIENT
What can we do if an insurance claim is denied?
You don't need to accept an initial denial as final. Ask the insurance company to supply you, in writing, the reason your claim is being denied. If you or your physician can supply information to address the reason, submit it and ask for a review of the claim. Depending on your insurer, you may get useful assistance from your employee benefits office, the billing office at your hospital or physician's office, or the customer service representatives at your insurer's toll-free number.
If you have a general question about insurance coverage, or believe that your insurer has denied a claim improperly or failed to act in accordance with your contract, contact your state's insurance commissioner's office (see Resources, for New York State contact information).
"Everything was covered prior to IVF. That's how come I had all the surgery, even though my doctors recommended IVF first. Insurance coverage would have saved three operations, and so much heartache and hardship could have been avoided." SUCCESSFUL IVF PATIENT
Should we pick a program with a money-back guarantee?
For many couples, cost is a major obstacle to undergoing treatments such as IVF and GIFT. In addition, most programs require full payment prior to beginning each cycle.
In recent years, some infertility programs have instituted creative pricing plans that attempt to make the cost of becoming pregnant more predictable. Some programs allow couples to pay a flat fee that covers all the costs of one full IVF cycle, plus additional cycles (if needed) to transfer frozen embryos that were created in the first attempt.
The most controversial pricing plans offer partial refunds to couples who do not succeed. Each plan differs somewhat in its details, but several elements are usually present:
- The cost for a money-back cycle is far higher than the cost for a cycle without a refund option. In general, this means that couples who succeed in becoming pregnant are subsidizing the refunds of those who do not.
- Couples must meet rigorous medical and age requirements to enter a refund program. By accepting those couples most likely to become pregnant easily, a program can minimize the number of refunds it must pay.
- Not all costs are refundable. In the contracts for refund plans, many charges (often those for tests to determine whether you qualify or for medications used during treatment) are not subject to the refund provisions. These may add several thousand dollars to your out-ofpocket costs.
- Programs typically define success as establishing a pregnancy of a certain length, often 12 weeks. If a miscarriage occurs after that point, you may not be eligible for a refund or for further treatment.
- A program may require that you let them make certain medical decisions, such as how many embryos to transfer. If you do not consent, you may lose your refund eligibility.
Money-back payment plans have led to heated debate among health professionals, ethicists and consumer advocates. The major argument in favor of the plans is that they allow couples without insurance coverage to spend a fairly predictable amount for treatment. If it is successful, they will be well on their way to becoming parents. If it is not, they will have the refund to use for further treatment or to pursue adoption or other means of family-building.
"It's important to research your insurance right at the beginning. We didn't have a clue what would be covered." IVF PATIENT
Some of the arguments against these plans are based on concerns about how refunds might affect the doctor-patient relationship. The American Medical Association, for example, objects on the grounds that it is unethical to link payment for medical treatment to a specific outcome. Other arguments focus on the potential for consumers to sustain medical or financial harm. Some organizations, including RESOLVE, are concerned that these plans create incentives for doctors to try to increase the odds of pregnancy by taking greater medical risks. There are particular concerns about any plan that requires couples to consent, in advance, to all treatments that may be recommended during the cycles it covers. In reality, your experience during the first cycle (such as a miscarried multiple pregnancy or the side effects of fertility drugs) may make you rethink the dose of medications and the procedures you wish to have used in the second cycle.
As you decide whether a refund program is right for you, proceed with caution and make certain you understand the medical and financial details. Some questions to ask include:
- How will my medical treatment be different if I participate? (For example, will I be required to undergo more tests than I would as a regular IVF patient?)
- What would my chance of pregnancy be if I had less aggressive treatment (such as using fertility drugs without IVF or GIFT)?
- What happens if I withdraw from treatment before I have finished all cycles covered by the plan?
- What happens if I miscarry?
- Can I limit the number of eggs/embryos transferred, or does the program decide?
How do the costs of infertility treatment compare with the costs of adoption?
The expenses involved in adopting a child are as varied as those for medical treatment. There may be no fees for adopting a child who is currently in foster care. As with infertility treatment, if you adopt a child in a different city or country, you need to factor in expenses for travel and time away from work as well as the adoption fees. After the adoption, children may be found to have medical or emotional problems that require special treatment.
Financial assistance is sometimes available for couples who adopt. These may include sliding-scale agency fees, government subsidies for adopting a child in foster care or to help pay the medical bills of adopted children with special needs, adoption benefits from employers and federal tax credits for adoption costs.
Looking Ahead to Pregnancy and Parenthood
Return to TopWill my infertility specialist see me through the pregnancy?
Some infertility specialists are practicing obstetricians. However, many specialists find it difficult to do both things well because deliveries are unpredictable, while infertility procedures often require precise timing. Some couples feel that they get more attentive infertility treatment if their doctor is not also practicing obstetrics. Others seek continuity of care.
Ask about your prenatal care options. If you can't get prenatal care at the same program, ask when and how you will be transferred, whether there will be ongoing contact, and whether you need a doctor specializing in high-risk pregnancies. You may wish to consult with an obstetrician before starting infertility treatment.
"I chose an obstetrician who did high-risk pregnancies, because I felt more comfortable with that." SUCCESSFUL IVF PATIENT
Are there special concerns for pregnancies achieved through infertility treatment?
Many pregnancies achieved through infertility treatment are designated as high risk for miscarriage or pregnancy complications. This may result from a woman's age, pre-existing medical problems that may have contributed to the infertility, or the treatments themselves. For example, in 1999, an average of 15 percent of IVF and GIFT pregnancies miscarried in women younger than 35. In women age 40, about 29 percent of IVF and GIFT pregnancies miscarried, as did 43 percent of those in women age 42. Ask your doctor how likely it is that you will miscarry or develop other serious complications.
An infertility specialist or obstetrician may be able to predict what special care you are likely to need. In general, pregnancies resulting from infertility treatment involve more medication, more prenatal tests, and are more likely to end in a cesarean delivery. Before any treatment, ask how it may affect your pregnancy and the prenatal care that will be recommended.
Pregnancies involving multiple births require special care and involve a higher risk of certain complications (see Risks).
Does infertility treatment endanger the children conceived?
In general, birth defects are thought to be no more common in infants born following infertility treatment than among those conceived without it. However, a greater number of the pregnancies end prematurely (primarily due to multiple gestation), which can have permanent consequences for a child, including breathing difficulties, blindness and brain damage. With new (but widely used) procedures such as ICSI, there has not been enough time to know whether any problem will become apparent as the children grow older. Recent data from a few population-based studies point to a possible trend towards a higher rate of birth defects and low birthweight in infants resulting from assisted reproduction, even when multiple gestations were not included. However, experts caution that this might reflect a risk resulting from the underlying infertility rather than the treatments used to establish pregnancy.
"There was an amniocentesis, sixteen weeks of progesterone shots, and extra check-ups - every two to three weeks." SUCCESSFUL IVF PATIENT
Psychological studies of children born after fertility treatment have identified no problems related to their conception. Some experts remain concerned that parents who invest large amounts of effort and money in conceiving their children may hold unrealistic expectations about their behavior and accomplishments.
If Treatment Fails
Return to TopWhen a cycle of infertility treatment doesn't work, should we try again?
Those who have undergone infertility treatment often describe feeling as if the next step were inevitable. If one regimen doesn't work, they feel they should proceed, as soon as possible, to the next attempt or a new level of therapy. But fertility experts and former patients stress the importance of planning treatment breaks to re-evaluate your options and prognosis. Ask your doctors to be realistic about your likelihood of success and to tell you what, if any, aspects of your treatment might be changed to maximize your chances.
Weigh that in the context of how the process is affecting your life. If your circumstances or priorities have shifted, you always have the option to forgo further treatment.
When is it time to find a new doctor or take a different approach?
One regret of many fertility patients is that they repeatedly received the same unsuccessful treatment - spending time and money that might better have been used for a different approach.
If any of the following circumstances apply to you, it may be time to get another medical opinion:
- You have used the identical treatment for months without re-evaluation.
- Your time and money for treatment is running out, and you want to make the most of it.
- Your doctor does not seem to have a clear treatment plan or wants to continue the same treatment indefinitely.
- Your doctor seems uninformed about your medical history and test or treatment results.
- Your doctor is reluctant to re-evaluate previous cycles and adjust your treatment plan.
- You feel you have not been monitored properly during previous treatments.
"After the first time, you think maybe your odds will be better the second or third time. Now I'm convinced that I shouldn't have done it the third time." UNSUCCESSFUL IVF PATIENT
When is it time to stop treatment?
Medically, there is rarely a clear endpoint to infertility treatment. There is usually a possibility, however small, that a different treatment or another cycle of the same treatment will succeed. Even menopause, which used to be an undisputed endpoint for treating women, is not a barrier to using donor eggs.
Stopping treatment, therefore, is rarely a medical decision alone. Rather, it is made by individuals or couples for a variety of medical and non-medical reasons. For each couple, the right stopping point may be different. Some couples reach a point at which further treatment would unacceptably compromise their health, finances or marriage. Some set a limit in advance on the number of cycles or the amount of time they will try. Some find the next treatment under consideration to be unacceptable for religious or personal reasons.
"For three years, I was doing the same thing over and over. If they would have said earlier to do IVF, I would have been better off and saved money." IVF PATIENT
At some point, couples can decide that becoming parents is more important to them than achieving a pregnancy, leading them to shift their towards adoption.
Those providing your infertility care should be willing to assist you in making decisions about ongoing treatment by:
- Providing their best estimate of the chances that treatment will succeed or that you will become pregnant without treatment;
- Openly discussing the option of stopping treatment (either permanently or as a break while you reassess your options);
- Encouraging you to seek a second medical opinion and/or psychological counseling at various points in your treatment; and,
- Respecting your priorities and values, including the option of placing an arbitrary limit on treatment.
Many couples find that an ongoing relationship with an independent counselor who is familiar with infertility issues can help them decide when it is time to stop treatment. A counselor can also provide support as they adjust to ending treatment without having achieved a live birth.
"I knew before the third try that I was going to stop afterward, and I knew it probably wouldn't work. I was depressed coming off it, but you know what? I'm fine... For the people who have trouble stopping, programs may need to have help built in." FORMER IVF PATIENT
Resources
Return to TopNEW YORK STATE OFFICES
New York State Attorney General's Office
HEALTH CARE BUREAU
Information and Complaint Hotline 800-771-7755 (select option 3)
If you have a question about insurance coverage, or believe that a claim has been improperly denied or an insurance company has failed to act in accordance with your contract, you can report it to this office.
New York State Department of Health
BLOOD AND TISSUE RESOURCES PROGRAM
Wadsworth Center
Empire State Plaza P. O.
Box 509 Albany NY 12201-0509
518-485-5341
www.health.ny.gov. email: btraxess@health.state.ny.us
This office can tell you whether a donor semen, egg donation, or donor embryo program is licensed by the New York State Department of Health.
New York State Department of Health
ENVIRONMENTAL HEALTH HELPLINE 800-458-1158
If your doctor has concerns about the reproductive impact of specific substances you are exposed to at work or in your community, this office can discuss the available scientific information with you or your doctor.
New York State Department of Health
OFFICE OF PROFESSIONAL MEDICAL CONDUCT
433 River Street,
Suite 303 Troy NY 12180
800-663-6114
http://www.health.ny.gov/professionals/doctors/conduct/
If you feel that you have received incompetent, negligent, or fraudulent care from a doctor in New York State, you may file a report with this office. You may also find out whether the Office of Professional Medical Conduct has ever taken action against a particular doctor.
New York State Division of Human Rights
One Fordham Plaza
Bronx NY 10458
718-741-8400
www.nysdhr.com
If you believe that a doctor has improperly discriminated against you (based on race, creed, color or national origin), you may make a report to this state office.
New York State Insurance Department
CONSUMER SERVICES BUREAU
Agency Bldg. 1-ESP
Albany NY 12257
800-342-3736
http://www.dfs.ny.gov
If you have a question about insurance coverage, or believe that a claim has been improperly denied or an insurance company has failed to act in accordance with your contract, you can report it to this office.
OTHER ORGANIZATIONS
American Board of Medical Specialties
1007 Church Street, Suite 404
Evanston IL 60201-5913
866-ASK-ABMS (866-275-2267)
www.abms.org
This organization can tell you whether a doctor is board-certified in a given specialty, or help you find a specialist in your area.
American College of Obstetricians and Gynecologists
409 12th Street,
SW P. O. Box 96920
Washington DC 20090-6920
202-484-3321
www.acog.org
This professional organization represents the nation's obstetricians and gynecologists. It supplies a physician directory and educational materials on subjects related to women's health.
American Infertility Association
666 Fifth Avenue,
Suite 278
New York NY 10103
888-917-3777
www.americaninfertility.org
This support and advocacy organization provides educational and support group meetings in the New York metropolitan area.
American Society for Reproductive Medicine Society for Assisted Reproductive Technology
1209 Montgomery Highway
Birmingham AL 35216-2809
205-978-5000
www.asrm.org
This professional organization for reproductive specialists offers a nationwide physician locator service and numerous educational materials on reproductive health and infertility treatments.
Centers for Disease Control and Prevention
Division of Reproductive Health
4770 Buford Hwy. NE,
Mail Stop K20
Atlanta GA 30341-3717
800-311-3435
www.cdc.gov/nccdphp/drh
This government agency publishes the national success rates for assisted reproductive technologies.
Federal Trade Commission
CDC-240
Washington DC 20580
877-FTC-HELP (877-382-4357)
www.ftc.gov
If you feel that an advertisement for infertility treatment is misleading or deceptive, report it to this office.
National Adoption Information Clearinghouse
330 C Street,
SW Washington DC 20447
888-251-0075
www.calib.com/naic
This service, provided by the U. S. Department of Health and Human Services, provides information on various options for adoption.
National Society of Genetic Counselors
233 Canterbury Drive
Wallingford PA 19086-6617
610-872-7608
www.nsgc.org
This organization can help you locate a genetic counselor in your area.
RESOLVE
1310 Broadway
Somerville MA 02144
617-623-0744
www.resolve.org
This national infertility association provides physician referrals, a national helpline, a variety of educational materials and support resources throughout the country.
Glossary
Return to TopAmerican Society for Reproductive Medicine (ASRM) - A professional society whose affiliate organization, the Society for Assisted Reproductive Technology (SART), reports annual fertility clinic data to the federal Centers for Disease Control and Prevention (CDC).
ART (assisted reproductive technology) - All treatments or procedures that involve surgically removing eggs from a woman's ovaries and combining the eggs with sperm to help a woman become pregnant. (Note: This definition is based on the 1992 law that requires the CDC to report on ART success rates. The term ART is sometimes used to describe a wider variety of treatments, including intrauterine insemination and the use of fertility drugs.)
ART cycle - A process in which 1) an ART procedure is carried out, 2) a woman has undergone ovarian stimulation or monitoring with the intent of having an ART procedure, or 3) frozen embryos have been thawed with the intent of transferring them to a woman. A cycle begins when a woman begins taking fertility drugs or having her ovaries monitored for follicle production.
Canceled cycle - An ART cycle in which ovarian stimulation was carried out but which was stopped before eggs were retrieved.
Centers for Disease Control and Prevention (CDC) - A government agency within the U. S. Department of Health and Human Services responsible for publishing annual fertility clinic success rates.
Donor egg cycle - An embryo formed from the egg of one woman (the donor) and then transferred to another woman who is unable to conceive with her own eggs (the recipient). The donor relinquishes all parental rights to any resulting offspring.
Ectopic pregnancy - A pregnancy in which the fertilized egg implants in a location outside of the uterus - usually in the fallopian tube, the ovary or the abdominal cavity. An ectopic pregnancy is a dangerous condition that requires prompt treatment.
Egg - The female reproductive cell, also called an oocyte.
Egg retrieval (also called oocyte retrieval) - A procedure to collect the eggs contained in the ovarian follicles.
Egg transfer (also called oocyte transfer) - The transfer of retrieved eggs into a woman's fallopian tubes through laparoscopy (see definition). This procedure is used only in GIFT (see definition).
Embryo - An egg that has been fertilized by a sperm and undergone one or more divisions.
Embryo transfer - Placement of embryos into a woman's uterus through the cervix after in vitro fertilization. In zygote intrafallopian transfer (ZIFT) (see definition), the embryos are placed in a woman's fallopian tube.
Endometriosis - A medical condition involving the presence of tissue similar to the uterine lining in locations outside of the uterus, such as the ovaries, fallopian tubes or abdominal cavity.
Fertilization - The penetration of the egg by the sperm and the resulting combination of genetic material that develops into an embryo.
Follicle - A structure in the ovaries that contains a developing (unfertilized) egg.
Fresh eggs, sperm or embryos - Eggs, sperm or embryos that have not been frozen. Note, however, that fresh embryos may have been conceived using either fresh or frozen sperm.
Gamete - A reproductive cell, either a sperm or egg.
GIFT (gamete intrafallopian transfer) - An ART procedure that involves removing eggs from the woman's ovaries, combining them with sperm, and using a laparoscope to place the sperm and unfertilized eggs into the woman's fallopian tube through small incisions in her abdomen.
Gestation - The period of time from conception to birth.
Gestational sac - A fluid-filled structure that develops within the uterus early in pregnancy. In a normal pregnancy, a gestational sac contains a developing fetus.
Gestational surrogate (also called a gestational carrier) - A woman who carries an embryo that was formed from the egg of another woman. The gestational carrier usually has a contractual obligation to return the infant to its intended parents. (In New York and some other states, it is illegal to enter into a surrogate parenting contract that calls for a woman to give up an infant and her maternal rights in exchange for money.)
ICSI (intracytoplasmic sperm injection) - A procedure in which a single sperm is injected directly into an egg; this procedure is most commonly used to overcome male infertility problems.
IUI (intrauterine insemination) - A medical procedure that involves placing sperm into a woman's uterus to facilitate fertilization. IUI is not considered an ART procedure, because it does not involve the manipulation of eggs.
IVF (in vitro fertilization) - An ART procedure that involves removing eggs from a woman's ovaries and fertilizing them outside her body. The resulting embryos are then transferred into the woman's uterus through the cervix.
Laparoscopy - A surgical procedure in which a fiber-optic instrument (a laparoscope) is inserted through a small incision in the abdomen to view the inside of the pelvis.
Live birth - The delivery of one or more babies with any signs of life.
Male factor - Any cause of infertility due to insufficient sperm quantity or other deficiencies that make it difficult for a sperm to fertilize an egg under normal conditions.
Miscarriage (also called spontaneous abortion) - A pregnancy ending in the spontaneous loss of the embryo or fetus before 20 weeks of gestation.
Multi-fetal pregnancy reduction - A procedure used to decrease the number of fetuses a woman carries and improve the chances that the remaining fetuses will develop into healthy infants.
Multiple birth - A pregnancy that results in the birth of more than one infant.
Multiple gestation - A pregnancy with multiple fetuses.
Oocyte - The female reproductive cell, also called an egg.
Ovarian monitoring - The use of ultrasound and/or blood or urine tests to monitor follicle development and hormone production.
Ovarian stimulation - The use of drugs to stimulate the ovaries to develop follicles and eggs.
Pregnancy (clinical) - Pregnancy documented by the presence of a gestational sac on ultrasound. For ART data-collection purposes, pregnancy is defined as a clinical pregnancy rather than a chemical pregnancy (i. e., a positive pregnancy test).
RESOLVE - A national, nonprofit consumer organization offering education, advocacy, and support to those experiencing infertility. Services include a national Helpline, quarterly newsletter, extensive literature list, member-to-member contact systems and local support groups through a network of over 50 chapters nationwide.
Stillbirth - The delivery of an infant delivered without signs of life after 20 or more weeks of gestation.
Sperm - The male reproductive cell.
Stimulated cycle - An ART cycle in which a woman receives oral or injected fertility drugs to stimulate her ovaries to produce more follicles.
Tubal factor - Structural or functional damage to one or both fallopian tubes that reduces fertility.
Ultrasound - A technique used in ART for viewing the follicles in the ovaries, and the gestational sac or fetus in the uterus.
Unexplained cause of infertility - Infertility for which no cause has been determined despite a comprehensive evaluation.
Uterine factor - A disorder in the uterus (e. g., fibroid tumors) that reduces fertility.
ZIFT (zygote intrafallopian transfer) - An ART procedure in which eggs are collected from a woman's ovaries and fertilized outside her body. A laparoscope is then used to place the resulting zygote (fertilized egg) into the woman's fallopian tube through a small incision in her abdomen.
Source: CDC, National Center for Chronic Disease Prevention and Health Promotion, Division of Reproductive Health
NEW YORK STATE TASK FORCE ON LIFE AND THE LAW
ADVISORY GROUP ON ASSISTED REPRODUCTIVE TECHNOLOGIES
Rev. Msgr. John A. Alesandro, J.C.D., J.D.
Episcopal Vicar
Western Vicariate Diocese of Rockville Centre
Rabbi J. David Bleich, Ph.D.
Professor of Talmud,
Yeshiva University Professor of Jewish Law and Ethics
Benjamin Cardozo School of Law
Owen K. Davis, M.D., F.A.C.O.G
Associate Professor, Obstetrics and Gynecology
Associate Director, In Vitro Fertilization Program
Center for Reproductive Medicine and Infertility
Weill Medical College of Cornell University
Chair of Practice and Membership Committees Society for Assisted Reproductive Technology
Nancy N. Dubler, LL.B.
Director, Division of Bioethics
Department of Epidemiology and Social Medicine
Montefiore Medical Center/ Albert Einstein College of Medicine
Alan Fleischman, M.D.
Senior Vice President
The New York Academy of Medicine
Cassandra E. Henderson, M.D.
Medical Director,
MIC-Women's Health Services New York, NY
Associate Professor of Obstetrics and Gynecology
Albert Einstein College of Medicine
Margaret R. Hollister, J.D.
Director of HelpLine and Educational Services
National RESOLVE
Gordon B. Kuttner, M.D., FACOG, FACS
Assistant Professor & Director Division of Reproductive Endocrinology, Surgery & Fertility
Department of Obstetric and Gynecology
University of Miami School of Medicine
Member, Work Group on Assisted Reproductive Technologies,
American College of Obstetricians and Gynecologists
Vivian Lewis, M.D.
Director, Reproductive Endocrinology Unit
Associate Professor, Obstetrics-Gynecology
University of Rochester Medical Center
Rochester, NY
Ruth Macklin, Ph.D.
Head, Division of Philosophy and History of Medicine
Department of Epidemiology and Social Medicine
Albert Einstein College of Medicine
Kathryn Meyer, J.D.
Chair of the Advisory Group
Senior Vice President and General Counsel
Continuum Health Partners, Inc.
Senior Vice President for Legal Affairs and General Counsel
Beth Israel Medical Center New York, NY
Mark V. Sauer, M.D.
Chief, Division of Reproductive Endocrinology
Department of Obstetrics and Gynecology
New York Presbyterian Hospital
Professor of Obstetrics and Gynecology
Columbia University New York, NY
Bonnie Steinbock, Ph.D.
Professor of Philosophy Chair,
Department of Philosophy University at Albany,
State University of New York
Judith Steinberg Turiel, Ed.D.
Author, Beyond Second Opinions
(Berkeley: University of California Press, 1998)
Berkeley, CA
Staff
Dwayne C. Turner, Ph.D., J.D., M.P.H.
Executive Director
New York State Task Force on Life and the Law
John Renehan, J.D.
Counsel
New York State Task Force on Life and the Law
Dana H. C. Lee, J.D.
Former Project Attorney
New York State Task Force on Life and the Law
Carl H. Coleman, J.D.
Associate Professor of Law
Seton Hall University School of Law
Former Executive Director
New York State Task Force on Life and the Law
Susan E. Ince, M.S.
Consultant
Judy Doesschate, J.D.
Division of Legal Affairs
New York State Department of Health
Jeanne V. Linden, M.D., M.P.H.
Director, Blood and Tissue Resources Program
New York State Department of Health