1115 MRT Waiver Public Forum
November 2017
- Presentation is also available in Portable Document Format (PDF)
1115 MRT Waiver Overview
1115 Demonstration Waiver
- Enacted in 1965, Title XIX (19) of the Social Security Act established regulations for the Medicaid program, which provides funding for medical and health–related services for persons with limited income.
- Section 1115 of the Social Security Act gives the Secretary of Health and Human Services the authority to waiver certain provisions and regulations to allow Medicaid funds to be used in ways that are not otherwise allowed under federal rules.
- 1115 Demonstration Waivers grant flexibility to states for innovative projects that advance the objectives of Title XIX of the Medicaid program by waiving certain compliance requirements of federal Medicaid laws.
General 1115 Demonstration Waiver Overview
- Special Terms and Conditions (STCs) outlines the basis of an agreement between the State and the Centers for Medicare and Medicaid Services (CMS). STCs specify the State´s obligation to CMS during the life of the demonstration, including general and financial reporting requirements and the timetable of State deliverables.
- Quarterly and annual reports are required and an Independent Evaluation is completed at the end of a Demonstration program.
- Budget Neutrality must be demonstrated. Federal Medicaid Expenditures with the Waiver cannot be more than Federal expenditure without the waiver during the course of the Demonstration.
- A Demonstration can be approved for 5 years, and renewed for an additional 3–5 years as requested by the State.
New York State´s 1115 Waiver History
- The NYS Medicaid Redesign Team (MRT) Waiver (formerly the Partnership Plan) has been in operation since 1997. It was initially designed to move Medicaid beneficiaries from a Fee–for–Service (FFS) delivery system to Mandatory Managed Care.
- The Waiver has been extended and amended several times since the initial implementation and provides the authority to offer Mainstream Managed Care, Managed Long Term Care, the Health and Recovery Programs and the Delivery System Reform Incentive Program, in addition to other programs.
1115 MRT Waiver Renewal
- New York´s 1115 MRT Waiver was renewed on December 6, 2016 effective through March 31, 2021.
- New York received approved Special Terms and Conditions from CMS in December 2016 to coincide with the renewal.
- Goals for the waiver are to meet the CMS Triple Aim: improve quality, improve health outcomes and reduce health care costs.
- Additional goals: Pay for Performance, reduce hospital admissions and re–admissions, reduce health care disparities, end FFS and institute a comprehensive, high quality, integrated care management system to lower costs.
1115 MRT Waiver Programs
- Medicaid Managed Care
- Provides comprehensive health care services (including all benefits available through the Medicaid State Plan) to low income uninsured individuals. It provides an opportunity for enrollees to select a Managed Care Organization (MCO) whose focus is on preventive health care.
- Mainstream Medicaid Managed Care (MMMC)
- MMMC plans are paid a capitated (flat) rate to provide for all medical needs of the beneficiary in lieu of a FFS based system.
- Adult Behavioral Health (HARPs)
- This program provides specialty care and treatment for mental illness and substance use disorders (SUD) via MCO´s and HARP´s.
- Home and Community Based Services (HCBS)
- Under the MLTC program, eligible individuals in need of more than 120 days of community–based long term care are enrolled with managed care providers to receive Long Term Services and Supports (LTSS). There is an expectation that the enrollee will remain in a community based setting.
- Managed Long Term Care (MLTC)
- Streamlines the delivery of long–term services to people who are chronically ill or disabled that wish to stay in their homes and communities. Services, such as home care or adult day care, are provided through DOH approved MLTC plans.
- Delivery System Reform Incentive Program (DSRIP)
- The purpose of this program is to provide incentives for Medicaid providers to create and sustain an integrated, high performance health care delivery system that can effectively meet the needs of Medicaid beneficiaries and low income uninsured individuals in their local communities by improving care, improving health & reducing costs.
- Designated State Health Programs (DSHP)
- State–funded health care programs, which serve low–income and uninsured New Yorkers, not otherwise eligible for federal matching funds.
i.e. Early Intervention, Child Lead Poisoning Primary Prevention, Cancer Services Program, etc.
- State–funded health care programs, which serve low–income and uninsured New Yorkers, not otherwise eligible for federal matching funds.
1115 MRT Waiver Pending Amendments
- Children´s System Transformation
- As part of New York´s goal to provide managed care for all, the State has submitted an amendment request to transition six children´s 1915c waivers to the 1115 Demonstration Authority.
- Provide HCBS through Medicaid Managed Care for eligible children.
- Streamline HCBS into new benefit package.
- Provide Health Home care management.
- OPWDD 1915c Transition
- Transfer OPWDD Comprehensive Waiver to the 1115 Demonstration Authority.
- Begin transition of Intellectual and Developmental Disabilities (IDD) population into managed care on a voluntary basis.
- Provide Health Home care management for eligible individuals.
- Offer a single Home and Community Based Services (HCBS) benefit package including Community First Choice Option.
DSRIP Progress Update
How have PPS performed so far?
PPS earned 95% of all available funds through DY2
$2,529,408,899 earned of
$2,640,661,327 available
PPS have distributed over $1.1B in DSRIP funds to PPS partners through DY3, Q2
PPS have engaged over 530,000 partners in DSRIP projects through DY3, Q2
PPS have reduced Potentially Preventable Readmissions by 14.9%
PPS have reduced Potentially Preventable ER Visits by 11.8%
PPR: Current results and performance opportunity
Potentially Preventable Readmission
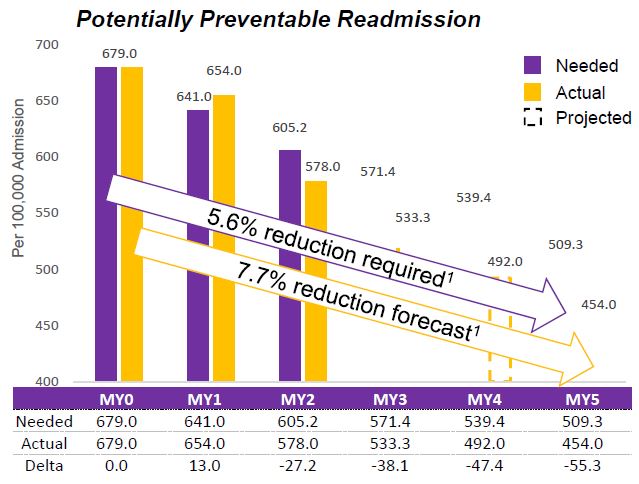
Pursuing the goal of 25% reduction...
If all PPS maintain current reduction rates, the State will achieve a 33.14% reduction over baseline (454.0 per 100,000 members)
| MY2 Rates | PPS |
|---|---|
| −30% to −20% | NYU Lutheran (−29.98%) |
| −19% to −10% | CCB, CPWNY, Refuah, MCC, SIPPS |
| −9 to −5% | NCI, Mount Sinai, One City, Bronx Partners, Nassau Queens, Suffolk CC, NYPQ |
| −4% to 0% | BHA, ACP, CNYCC, NY Presby, FLPPS, WMC, Montefiore, Care Compass, Alliance |
| 1% + | AHI, Leatherstocking, BHNNY |
Potentially Preventable Emergency Room Visits
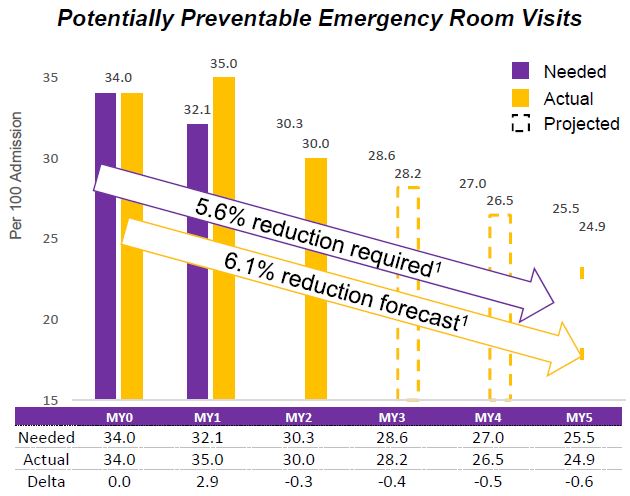
Pursuing the goal of 25% reduction...
If all PPS maintain current reduction rates, the State will achieve a 26.9% reduction over baseline (24.9 per 100 admission)
| MY2 Rates | PPS |
|---|---|
| −20% to −10% | Refuah (−18.52%), CCB, AHI, Suffolk CC |
| −9% to −5% | WMC, SIPPS, Care Compass, NYPQ, CNYCC, Leatherstocking, FLPPS, Nassau Queens, NYU Lutheran, Montefiore, One City, Alliance |
| −4 to −0% | Mount Sinai, ACP, CPWNY, NY Presby, MY0 MY4 MY5 BHNNY, Bronx Partners, NCI |
| 1% + | AHI, Leatherstocking, BHNNY |
Notes:
1. Projection assumes a consistent denominator year over year, and rate estimates are based on CAGR projection driven by MY0 – MY2 non–case mix adjusted results
How have PPS performed so far?
PPS have successfully met all project requirements for 31 projects through DY2
95% of DY2 project requirements successfully implemented
PPS were scheduled to complete an additional 20 projects by DY3, Q2
1115 MRT Waiver Resources
1115 MRT Waiver Website
http://www.health.ny.gov/health_care/medicaid/redesign/medicaid_waiver_1115.htm
Managed Care
https://www.health.ny.gov/health_care/managed_care/index.htm
DSRIP
http://www.health.ny.gov/health_care/medicaid/redesign/dsrip/
OPWDD Webpage
01/19/2017 STCs DOH website
https://www.health.ny.gov/health_care/managed_care/appextension/docs/2017–01–19_renewal_stc.pdf
Follow Us