Introduction
History and Background of the New York State Network
Historical Perspective
Poison control services have existed in New York State since 1953, when the first poison control centers were established as a result of the collaborative efforts of the American Academy of Pediatrics, the New York Academy of Medicine and local medical societies.
Over the next two decades, additional regional programs provided poison services. The scope of these programs varied depending on the needs of the community and the available funding. To determine the level of poison control services available, the Department of Health in 1979 conducted a survey of all poison control services in the State. Results illustrated that only 50% of New York State's population received any level of poison control services and there was a lack of service uniformity in those areas.
State Involvement
In 1981, the Commissioner of Health established an advisory council on poison prevention and control. The purpose of the council was to advise the Department of Health on the further development of statewide standards for poison control services. The collaborative efforts of the council and the department resulted in the development in 1984 of the comprehensive Administrative Guidelines for the Operation of Poison Control Centers. Those guidelines were subsequently used in the development of State regulations.
The Poison Control Network Act was signed on May 12, 1986 and provided for the establishment of regional poison control centers to form a statewide network to reduce poisonings, educate the public about hazardous exposures and assure statewide emergency coverage by poison control facilities. Poison control centers must disseminate expert information to professionals and the public. Centers must also participate in collection of uniform data and conduct research to enhance the science of toxicology. It was recognized that regional poison control centers can reduce hospital costs by handling nontoxic and mildly toxic poisoning emergencies through telephone consultation.
Together the centers formed the Association of Poison Control Centers of New York State, for the purpose of collaborating on issues of concern to all of the centers and interacting with the New York State Department of Health.
Previous Consolidations
Extensive consolidation of poison control services has taken place since its inception in 1955. During 1956 - 1981, there were 17 - 21 poison control centers in New York State. Many of these existed as a part of emergency room services and many handled calls during day time hours only. There were no regulations or guidelines for these services.
With the enactment of the New York State Poison Control Network Act in 1986, eight poison centers were designated, one for each of the state's health service areas. In 1990, Ellis Hospital Poison Control in Schenectady transferred their services to the Hudson Valley Regional Poison Center and the Southern Tier Poison Center in Binghamton was absorbed by Central New York Regional Poison Control Center.
For the past decade, the six remaining poison centers have effectively carried out the delivery of services to the 18 million people of New York State. During 2001, the Hudson Valley Regional Poison Center converted to a public education center only. As such, the Network is now comprised of five (5) emergency call receiving centers and one public education center. The counties serviced by the Hudson Valley Regional Poison Center were reassigned to the Central New York Regional Poison Control Center, with the exception of Westchester County, which was assigned to the Long Island Regional Poison and Drug Information Center. The newly named Hudson Valley Poison Education Center, continues to provide public education services under the supervision of both the Central New York Regional Poison Control Center and the Long Island Regional Poison and Drug Information Center. The five (5) remaining full service centers are certified by the American Association of Poison Control Centers.
Structure of the Network Location of Centers
The current network consists of five (5) poison control centers and one poison educational center, strategically located throughout the state as noted on the map below. Management information specific to the individual centers is included in Appendix One
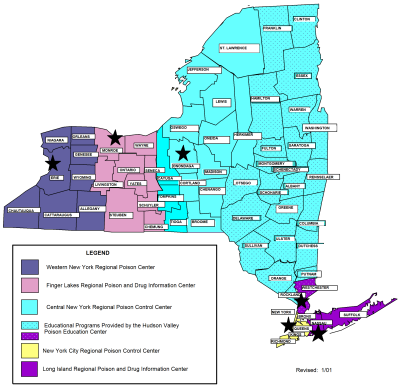
Services Provided By Poison Control Centers
Each of the five (5) regional poison control centers is staffed by a Board Certified Medical Director, a Clinical Board Certified Managing Director, a team of Specialists in Poison Information, Health Educators, and support staff. For the Education Center, there is a Health Educator and support staff. In New York State, the poison control centers perform the following services:
Telephone Communications
Centers publicize their emergency telephone numbers and services to the general public and to health care professionals. The American Association of Poison Control Centers has initiated a new national toll free number (1-800-222-1222) that allows anyone access to their local poison control center. This is similar to the 911 or 411 process. The national toll free number was activated in New York State in June 2001. This new toll free number was tested during the events of September 11, 2001. With the loss of Tower II and the Verizon buildings, the majority of local phone service to the New York City and Long Island poison centers decreased and calls were intermittent. Fortunately, the toll free calls were easily re-routed to other Network poison centers allowing for no loss of calls. All of the Network centers have maintained their local pre-existing numbers in addition to the toll free number. The Network has also developed a backup system where, in case of telephone failure, local calls can be automatically re-routed, as well.
Distribution and advertising of the new phone number is ongoing and usage is being documented. This system allows the Centers to share educational and awareness materials. As always, each Center's emergency telephone numbers are listed on the inside front section of all local telephone directories and is provided to all telephone operators. Centers also have telecommunications that allow contact with hearing impaired persons. Commercial translation services are used by centers with a large number of foreign language speaking populations.
Specialists in Poison Information (registered nurses, pharmacists, physician assistants, and/or physicians) are trained in toxicology, certified by examination, and answer incoming calls to the poison control center. Services include the provision of:
- expert telephone consultation for emergency poison exposures and inquiries 24 hours per day, seven days per week to health care professionals and the public;
- assessment of the risk of toxicity associated with poisoning emergencies;
- home treatment information to the public and clinical consultation to health care professionals;
- ability to recognize potential epidemics, biological and/or chemical terrorist events.
The following case illustrates the cooperation amongst health care professionals, the patient and the poison specialist:
Case:
In early September, the poison center received a call from a doctor in a local emergency department from a family member of a patient who was vacationing in Thailand. Apparently, she was stung by a sea urchin and was in considerable pain. The certified poison information specialist (CSPI), who received the call, made a three-way connection between the patient in Thailand and the physician in the emergency department so an accurate assessment of her injuries could be made. After a few minutes, the poison specialist made the recommendation of hot water soaks, removal of the spines, and a pain reliever for the discomfort.
Crisis Intervention
Poison control centers have immediate access to on-line and print toxicology resources, which display the most current information on more than 500,000 products, drugs, plants, and environmental toxins. The centers are supported 24 hours per day, every day, by medical and clinical toxicologists, and have access to expert consultants in specialties such as plants, mushrooms, snakes, insects and environmental and industrial toxins.
Crisis intervention services:
- contribute to reducing health care costs by triaging home calls to prevent unnecessary emergency department visits;
- provide drug information for the public and health care professionals;
- serve as a source of information on life saving antidotes and vaccines;
- serve as resource for chronic lead poisoning and other environmental toxins;
- serve as a resource for substance abuse information and management;
- provide reporting, surveillance and act as an early warning network for the following: pesticide exposures, food poisoning episodes, substance abuse, herbal products and alternative medicine, biological and chemical warfare terrorist attacks, and exposures associated with malicious acts;
- cooperate in reporting all clusters of similar exposures and hazards to government agencies including the FDA, CPSC, OSHA, EPA, CDC, Department of Environmental Conservation, and local and state health departments.
Education and Research
- provide professional education to medical students, physicians, pharmacists, nurses, and other health care professionals;
- identify new toxic risks;
- conduct research to better prevent poisoning and enhance the management of poisoned persons;
- participate in nationwide sharing of data regarding poisonings;
- promote poisoning prevention among the general public;
- have an analytical toxicology laboratory available.
Most emergency calls to the centers are managed by poison specialists over the phone, avoiding expensive visits to a health care facility. Center staff follow-up on the patient's status by calling them at home at regular intervals to ensure the patient's welfare. If staff assess that further evaluation or treatment by a physician is necessary, they refer the caller to the nearest health care facility capable of providing appropriate care; call that facility to inform the staff of the referral; if necessary, arrange for emergency transportation of the patient. Patient status is monitored by the specialists until the patient is released from the treatment facility. The poison control centers provide expert consultation to health professionals in emergency departments and other health care settings 24 hours per day, seven days per week. Centers conduct product surveillance for use as early warning systems.
The medical and managing directors play important roles in the centers by providing expert toxicology in-service training, hands-on intervention with patients at host facilities, and consultations for health professionals from their own hospitals and from other health care facilities. This vital service provides medical students and residents with hands-on experience in management of poisoned patients, thus helping prepare physicians and future toxicologists.
In addition, medical and managing directors meet with members of the community they serve including EMS providers, 911
communication centers, city, county and regional emergency management agencies, health care provider users and advocacy groups.
Health educators at each of the centers conduct extensive community outreach and education regarding the services provided by the centers and the prevention of poisoning. The health educators are responsible for promoting the center's emergency telephone numbers throughout their region. Educators will continue to promote and distribute educational materials with the national 800# on a statewide basis. In addition, the health educators facilitate poison prevention/awareness events and deliver education programs that target teachers, children, parents and care givers.
Professional Organization Involvement
Each poison center in New York State belongs to, and is certified by, the American Association of Poison Control Centers (AAPCC). Members of the centers take an active, and in some instances, leadership role in the operations of the association including membership on board of directors, certification committee, public education committee, quality assurance committee, abstract review committee, scientific affairs subcommittee, nominating committee, personnel proficiency, long range planning, specialist in poison information committee, and manager's committee. Members of the New York State Network participate fully in the educational and information sharing components of the AAPCC through attendance at the annual and mid-year meetings.
In addition, The Association of Poison Control Centers of New York State, a network made up of the members of the five regional poison control centers and one public education center, collaborate to set policy, share case information, exchange ideas in administration, public education, professional education, data collection and conduct research.