Ear Infections in Children
- The complete brochure Ear Infections in Children is also available in Portable Document Format (PDF, 878KB)
An ear infection is one of the most frequent reasons parents take a child to see a doctor. This brochure will help you understand this disease and the treatment methods that may be suggested by your child's doctor or health caregiver.
What is acute otitis media?
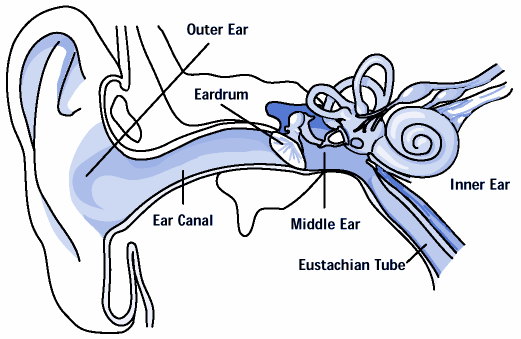
Acute otitis media is the medical term for the common ear infection. Otitis refers to an ear infection and media means middle. So, acute otitis media is an infection of the middle ear, which is located behind the eardrum.
There is a tube, called the Eustachian tube, that connects the middle ear to the nose. This tube helps drain extra fluid from the middle ear. When a child has a cold, swelling in the nose may impede drainage. Germs (either viruses or bacteria) can enter the middle ear and cause an infection. The infection results in increased fluid in the ear and can cause pain, fever and irritability.
When should a parent suspect an ear infection?
A parent should suspect an ear infection when a child becomes ill with fever, is irritable, and usually complains of pain in the ear. Many children who develop ear infections will first have colds. However, ear pain can be caused by other problems, such as a sore throat, without an ear infection.
How is an ear infection diagnosed?
An ear infection should not be diagnosed over the telephone. A doctor or other health caregiver should examine the child. Usually, the child should be seen within 24 hours. However, an emergency room visit is not necessary unless ordered by your health caregiver. While waiting for the office visit, you can give the child a non-aspirin pain reliever, such as ACETAMINOPHEN or IBUPROFEN, to control the pain.
During the examination, your child's health caregiver will take a brief history and carefully examine the ear, checking the appearance and movement of the eardrum.
How is an ear infection treated?
Research suggests that many children with ear infections will get better without antibiotics, and with no ill effects. This is called the "observation option" or "watchful waiting." This option reduces the use of unnecessary antibiotics and limits the child's exposure to the side effects of antibiotics. It also reduces the chance that "super bacteria" — bacteria that cannot be killed by antibiotics — will develop.
Your child's health caregiver may offer this option for your child depending on his or her age and symptoms. If your health caregiver does not discuss it, you may want to ask if this is an option for your child.
It is important that you discuss the plan with your health caregiver if the observation option will be used. If, on the other hand, antibiotics are needed, you should trust him or her to select the proper medication and course of treatment. A parent should not insist on a particular antibiotic.
If an antibiotic is prescribed, it will likely be amoxicillin, unless the child is allergic to penicillin. Depending on the situation, the provider may decide that the child should take the antibiotic for five days instead of 10 days.
Of course, differences in children, and the severity of the illness, may change these choices.
Remember, a single dose of an antibiotic will not make the ear infection feel better! In fact, the antibiotic will not relieve the symptoms. Ear pain from an infection should be treated with a non-aspirin pain reliever.
Even if your child appears better, make sure that your child takes all the antibiotics prescribed by your health caregiver.
Is follow-up care necessary?
If the child is better in 48 hours with either treatment option, the health caregiver may choose not to see the child again for two to four weeks. If, however, the symptoms are not resolved in 48 hours, the child should be re-examined.
Can ear infections be prevented?
Ear infections are very common in children. But there are things parents can do to reduce the number of ear infections their children may have.
Ear infections are not contagious or spread from one person to another, but the colds that result in ear infections are. Colds are spread when germs are released from the nose or mouth during coughing or sneezing. Anything that can reduce the spread of germs will help reduce ear infections.
Because most ear infections occur in children under the age of three, parents can play an active role in preventing them:
- Have children use disposable tissues when they blow their noses or to cover their mouths when they cough.
- Teach children that tissues should be used only once and then thrown away properly.
- Do not allow children to share toys that they put in their mouths.
- Wash dirty toys in hot, soapy water before allowing other children to play with them.
- Teach children to always wash their hands after sneezing or coughing into them.
- Do not allow sick children to share food or drinks.
- Regularly wash and disinfect all surface areas and common play areas.
- Do not share bathroom cups and other utensils that go in the mouth.
- Breastfeeding appears to lower an infant's risk of ear infections.
- Children under age two should not lie flat when they bottle-feed.
- No one should be allowed to smoke around children. Secondhand smoke increases a child's risk for ear infections. In fact, even smoke from wood stoves can irritate breathing and increase the risk of an ear infection.
- Children in day care centers tend to have more colds and a higher risk of ear infection. Although it would be best to keep an ill child at home, this may not be possible. Parents should work with day care center staff to ensure proper handwashing, tissue use and cleanliness.
If, despite your best efforts, you think that your child has an ear infection, make sure that he or she is examined by a doctor or health caregiver. And, if there is an infection, be sure to follow the recommended treatment approaches. Always contact your child's doctor or health caregiver first!