Strengthening New York's Public Health System for the 21st Century
REPORT OF THE PUBLIC HEALTH INFRASTRUCTURE WORK GROUP TO THE PUBLIC HEALTH COUNCIL
VII. MEASURING PERFORMANCE OF THE NEW YORK PUBLIC HEALTH SYSTEM
A. The National Public Health Performance Standards Program
The National Public Health Performance Standards Program (NPHPSP) began with the mission "... to improve quality and performance, to increase accountability, and to increase the science base for public health."31 Begun in 1998 by the federal Centers for Disease Control and Prevention (CDC), the program was developed in collaboration with many national organizations representing state and local health departments including:
- The National Association of County and City Health Officers (NACCHO),
- The American Public Health Association,
- The Association of State and Territorial Health Officials (ASTHO),
- The National Association of Local Boards of Health and
- The Public Health Foundation
The goal of the NPHPSP is to measure the practice of public health at the state and local levels using certain standards that describe best practices within the context of the ten essential public health services and their delineated subparts. The method of measurement is a self-applied questionnaire with multiple-choice questions that relate to these optimal standards. New York State was enrolled in the initial trials of the NPHPSP. Forty-nine local health departments used Version B of the instrument to assess the performance of their local health department while eight counties used Version C to assess the performance of their local public health system. The overall statewide average score for the local health departments participating in Version B and C was 64.
Figures 4 and 5 below illustrate the local health departments' performance in both Version 5b and Version 5c of the National Public Health Performance Standards Program.
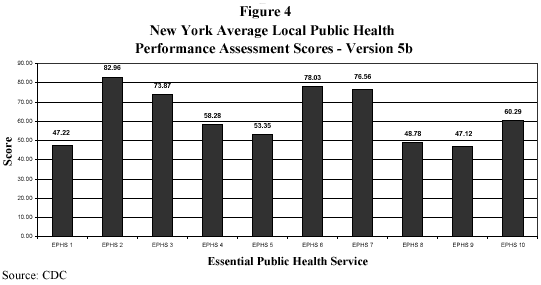
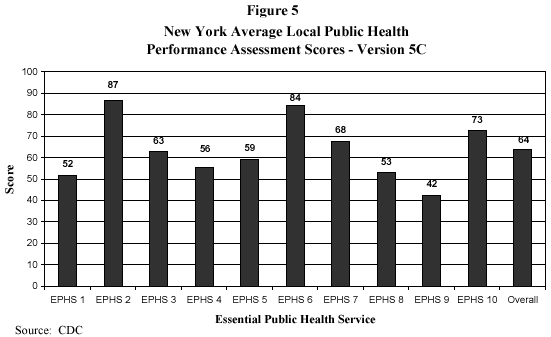
A review of these graphs illustrates that New York State local health departments rated their own performance above the statewide average in five essential services:
- EPHS # 2-Diagnose and Investigate Health Problems/hazards,
- EPHS # 3-Inform, Educate and Empower People about Health Issues,
- EPHS # 6-Enforce Laws and Regulations that Protect Health and Ensure Safety,
- EPHS # 7-Link People to Needed Personal Health Services and Assure the Provision of Health When Otherwise Unavailable,
- EPHS # 10-Conduct Research for New Insights and Innovative Solutions to Health Problems.
Local health departments rated their own performance below the statewide average in five other essential services:
- EPHS # 1-Monitor Health Status to Identify Community Health Problems,
- EPHS # 4-Mobilize Community Partnerships to Identify and Solve Health Problems,
- EPHS # 5-Develop Policies and Plans that Support Individual and Community Health Efforts,
- EPHS # 8-Assure a Competent Public Health and Personal Health Care Workforce,
- EPHS # 9-Evaluate Effectiveness, Accessibility and Quality of Personal /Population-Based Health Services.
B. Public Health Emergency Preparedness
Even before September 11, 2001 and certainly since then, the New York State Department of Health in New York State has focused a considerable degree of attention on bioterrorism (BT) preparedness. The focus on BT has enabled the Department to bolster the state and local public health infrastructure, and has resulted in improved public health preparedness in general. The Centers for Disease Control and Prevention (CDC) grant funds of $27 million for BT have provided additional resources for disease surveillance and control, for communication and communication systems including Internet access and video conferencing, and for training and continuing education of public health system partners. It has also resulted in increased interaction with partners (hospitals, emergency management services and organizations, state wide associations) allowing the public health system to test regional planning approaches to delivery of public health services such as epidemiology services and to provide for an increased understanding of the function and value of public health. The grant funding from the CDC has been effective because it has been used to augment existing state and local investments in public health services and the work force.
31 The Future of the Public's Health in the 21st Century, Institute of Medicine, National Academy Press, 2003.