Uterine Fibroids
This summary discusses:
- Fibroids
- Uterine Fibroids
- Uterus - Womb
- What causes fibroids?
- Can fibroids turn into cancer?
- Who usually develops fibroids?
- Symptoms
- How do you know you have a fibroid?
- Diagnostic Procedures
- Fibroids and Pregnancy
- Treatments
- Development of New Treatments
Fibroids
Uterine Fibroids are common non-cancerous (benign) tumors of the uterus and are the most frequent reason for recommending a hysterectomy. They grow from the muscular wall of the uterus and are made up of muscle and fibrous tissue. Many women over 35 have fibroids, but usually have no symptoms.
In some women, however, fibroids (myomas) may cause heavy bleeding, pelvic discomfort and pain and occasionally exert pressure on other organs. These symptoms may require treatment. Treatment may take the form of medication to control pain and bleeding, hormone therapy to shrink the tumor, surgery to remove the tumor or occasionally a hysterectomy. There are promising new experimental drugs that may temporarily shrink the tumors. These drugs may have serious side effects and are generally very costly. There is a type of abdominal surgery (myomectomy) that removes the myoma without removing the uterus (see Alternatives for additional information). These treatments may be sufficient or they may offer temporary relief and enable a woman to postpone having a hysterectomy, especially if she still wishes to bear children. In most severe cases a hysterectomy may be recommended.
Some women choose to do nothing since fibroids will often shrink in size as a woman goes through menopause.
What is a fibroid?
A fibroid is a non-cancerous growth (tumor) made up of mostly fibrous tissue, like muscle. Fibroids grow in or around the uterus (womb). They are the most common type of growth in a woman's pelvic area (the pelvis is the bony structure at the bottom of the spine).
Uterine Fibroids
According to the U.S. National Institutes of Health (NIH), 20-25% of women of reproductive age have fibroids. By the age of 50, up to 80% of black women and up to 70% of white women have fibroids. Uterine fibroids are most common in women who are in their 40s and early 50s, although some women may develop fibroids at a younger age. At least 25% of women have uterine fibroids which can cause problems. Many women with fibroids never have a problem and never know they have a fibroid.
Uterus - Womb
The uterus (womb) is a pear-shaped organ located in the lower part of a woman's body. It is made up of the muscle wall, endometrium (lining) and the cervix (opening). In women who are not pregnant, the lining is shed monthly as part of the menstrual cycle (period). In women who are pregnant, the uterus is where a fetus will grow and develop.
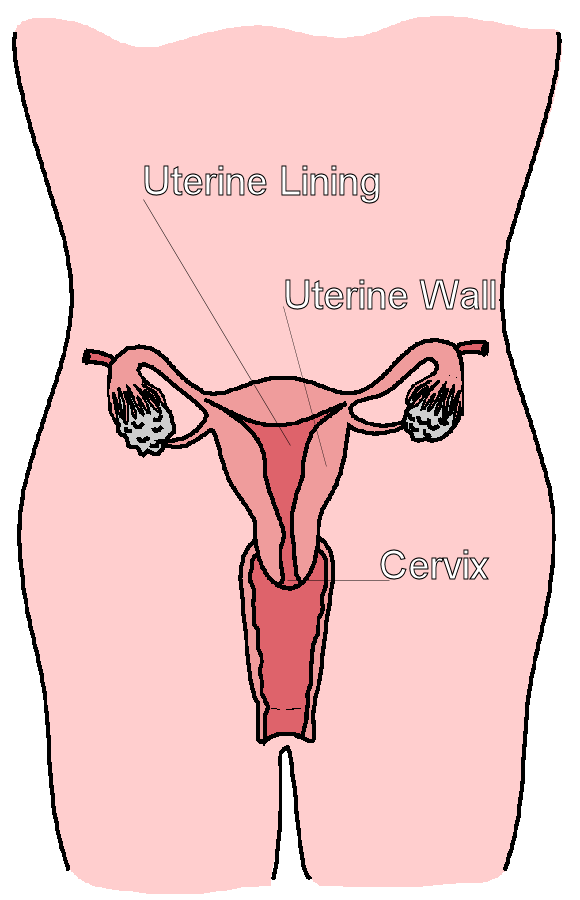
Figure 1. Female Reproductive System
Are there different types of fibroids?
A fibroid can be very small, the size of a seed, or large, the size of a grapefruit. The medical term for a fibroid is a leiomyoma or myoma. A woman may have one fibroid or many. A fibroid may be inside the uterus (submucosal), outside the uterus (subserosal), or in the wall of the uterus (intramural). Most fibroids grow in the wall of the uterus. Fibroids can also grow out from the uterus on stalks called peduncles.
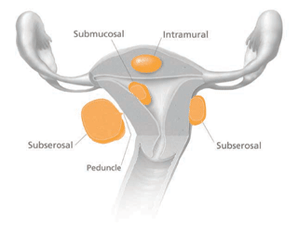
Figure 2. Illustration of Uterine Fibroids from the US Health and Human Women's Health Web site
What causes fibroids?
Fibroids begin when cells overgrow in the wall of the uterus. However, the cause of uterine fibroids is not known. Researchers have many ideas of what may cause fibroids, but none of these are seen as definite causes of fibroid tumors. Some of these ideas include:
- Fibroids may be genetic (runs in families).
- Female hormones, estrogen and progesterone, cause fibroids to grow.
Fibroids grow rapidly during pregnancy, when hormone levels are high and shrink when anti-hormone medicine is used. Fibroids also stop growing or shrink once a woman reaches menopause.
Can fibroids turn into cancer?
Fibroids are usually benign (not cancerous). Having fibroids does not increase a woman's risk of developing cancer. In less than 1 in 1,000 cases a cancerous fibroid will occur. A cancerous fibroid is called leiomyosarcoma.
Who usually develops fibroids?
Age, race, lifestyle and genetics may play a part in the development of fibroids. Here are the few known risk factors:
- Having a family member with fibroids increases the risk. If a woman's mother had fibroids, her risk of having fibroids is about 3 times higher than average.
- African-Americans are 2-3 times more likely to present with symptomatic (problems such as pain or bleeding) uterine fibroids and will often develop fibroids at a younger age than the rest of the population of women with uterine fibroids.
- Asian women have a lower incidence of symptomatic uterine fibroids.
- Obesity is associated with uterine fibroids. The risk of obese women developing fibroids is 2-3 times greater than women of average weight.
- Eating beef, red meat (other than beef), and ham has been linked with having uterine fibroids, while eating green vegetables seems to protect women from developing fibroids.
What are the symptoms of fibroids?
For most women fibroids do not cause symptoms. At least 25% of women who have uterine fibroids do have symptoms which may include:
- Heavy bleeding or painful periods
- Bleeding between periods
- Cramping
- Bloating of the lower belly (abdomen or pelvic area)
- Feeling of fullness in the pelvic area
- Pain during sex
- Low back pain
- Frequent urination
Fibroids can also cause infertility (being unable to get pregnant), miscarriages, or premature labor (labor before 37 weeks of pregnancy).
How do you know you have a fibroid?
You may not know if you have fibroids if they are not causing any problems. A health care provider may find a fibroid on a routine exam, or you may see your health care provider if you are having symptoms. The health care provider may:
- Do a physical exam of your uterus (pelvic exam) to check the size of your uterus (womb), and may feel the fibroid as a lump on your uterus during the pelvic exam.
- Send you for a procedure to get a "picture" of your uterus.
- Do blood tests to check your blood count for anemia (low iron in your blood due to heavy periods or bleeding between periods) or for other problems.
The pelvic exam and the tests help your health care provider find out if you have fibroids, where they are and how large they are.
What kind of procedures may be done to find out if you have fibroids?
Your health care provider can do an imaging examination to produce a picture to confirm that you have fibroids. These might include:
- Ultrasound (US) - uses sound waves to produce a picture to see if you have fibroids. An ultrasound probe can be placed on the abdomen or it can be placed inside the vagina during the ultrasound.
- Magnetic Resonance Imaging (MRI) - magnets and radio waves are used to produce the picture.
- X-rays - uses a form of radiation to produce the picture.
- Cat Scan (CT) - takes many X-ray pictures of the body from different angles for a more complete picture.
- Hysterosalpingogram (HSG) <- an x-ray done by
- Sonohysterogram - an ultrasound test that uses saline and ultrasound to look at the uterus and pelvic area.
You might also need additional procedures to know for sure if you have fibroids. There are two types of procedures to do this:
- Diagnostic Laparoscopy or Gynecologic Laparoscopy - surgery in which the doctor makes a cut into the abdomen and inserts a thin lighted tube with a small camera attached. This allows the doctor to see inside the abdomen to look at the uterus, ovaries and pelvic area.
- Hysteroscopy - The doctor passes a long, thin tube with a light through the vagina and cervix into the uterus. The hysteroscope has a light and camera attached to it so your doctor can see the inside of the uterus on a video screen.
Will I have trouble getting pregnant if I have fibroids?
In some cases, fibroids are severe enough to prevent a woman from becoming pregnant (infertility). If a woman is pregnant, fibroids can cause problems (complications) during pregnancy, labor and delivery. Since fibroids are controlled by hormone levels they grow rapidly during pregnancy. Hormone levels are high during pregnancy.
What kinds of problems will fibroids cause in pregnancy?
The most common complications caused by fibroids during pregnancy are:
- Labor does not progress - this can happen if the uterus (womb) does not contract as it should and the baby does not move out through the birth canal to be born.
- Baby is breech - the baby is coming out bottom first. The usual position of a baby is for the head to come out first, but breech babies are in the bottom or feet-first position.
- Placenta abruption - the placenta pulls away from the uterus (womb) before delivery.
- Preterm delivery - the baby is born before 37 weeks of pregnancy.
- Cesarean section (C-section) - a cut (incision) is made in the mother's abdomen (belly) and uterus (womb) and the baby is lifted out.
What are the treatments for fibroids?
If a woman is having heavy bleeding which could cause a low blood count, or is experiencing severe cramping, painful periods, infertility or bladder or bowel problems, she will need treatment.
Before deciding on a treatment, it is important to talk with your health care provider to get more information. Ask your health care provider:
- How many fibroids do I have and will they grow bigger?
- Where are they located and will they cause problems?
- Do I need treatment if I am not having any problems?
- What are my choices for treatment?
- Can I try other options such as medications or hormone therapy before I try surgery?
- What are the treatment options other than hysterectomy?
- What are the risks and benefits of these treatment options?
If you need more information before deciding on a treatment, you can ask your health care provider to refer you to another doctor for a second opinion to be sure you are making the best decision.
There are many options for treatment of uterine fibroids including:
Medications
For occasional mild to moderate pain or discomfort, an over-the-counter medication such as ibuprofen or acetaminophen can be taken. Over the counter nonsteroidal anti-inflammatory drugs (NSAID), such as ibuprofen, if used during early pregnancy, may cause miscarriage.
For symptoms of heavy bleeding, which can cause anemia, taking an iron supplement and an iron-rich diet can help to prevent anemia or treat anemia. More serious symptoms may require stronger drugs available by prescription from your health care provider.
Hormone Therapy
Birth control pills (oral contraceptives) can be used to treat the bleeding symptoms of fibroids. Low-dose birth control pills or progesterone-like injections (such as Depo-Provera) do not make fibroids grow and can help control heavy bleeding. An intrauterine device (IUD) which contains a small amount of progesterone-like medication (such as Mirena IUD) can also control fibroid symptoms and provide birth control.
Gonadotropin-releasing hormone agonists (GnRHa)
Some fibroids are treated with GnRHa, a hormone that reduces the amount of estrogen to shrink the fibroids and control symptoms. Sometimes GnRHa is used before surgery to make fibroids easier to remove. Most women can take GnRHa without any problems, but using GnRHa causes menopause-like side effects such as:
- Hot flashes
- Depression or mood swings
- Decreased sexual interest
- Insomnia (not being able to sleep)
- Headaches
- Bone thinning
- Joint pain
The side effects go away when the GnRHa is stopped, and once you stop taking the drugs the fibroids often grow back quickly. Most women don't get a period when taking GnRHa. This can relieve the symptoms of heavy bleeding and improve the low blood count (anemia) which can happen with heavy bleeding. Since GnRHa can cause bone thinning, it is generally used for six months or less.
Surgery
There are three surgical treatments for fibroids:
- Myomectomy - cutting fibroids from the uterus,
- Endometrial Ablation - removing or destroying the lining of the uterus, or
- Hysterectomy - removing the entire uterus (womb).
The surgical method used depends on the size, location, and number of fibroids.
Myomectomy
Myomectomy is removing fibroids without taking out the uterus, which makes pregnancy possible for some women. A woman who has had a myomectomy can have problems with the placenta or can make a cesarean delivery more likely if she becomes pregnant. Fibroids may also develop again, even after a myomectomy.
Myomectomy can be done by:
- Laparoscopy - making one or more small cuts in the abdomen and inserting a lighted viewing instrument to remove the fibroids through the small cuts,
- Hysteroscopy - using a lighted viewing instrument going through the vagina and into the uterus to remove the fibroids, or
- Laparotomy - major surgery done by making a larger cut into the abdomen and the uterus.
The type of operation done for the myomectomy depends on the size and location of the fibroids.
Endometrial Ablation
Endometrial Ablation is when the lining of the uterus is removed or destroyed by using laser, wire loops, freezing or other methods to control very heavy bleeding. This procedure is usually considered minor surgery and can be done on an outpatient basis. A woman having this procedure will be unable to have children. Complications can occur, but are not common.
Hysterectomy
A hysterectomy an operation to remove the uterus (womb). The only absolute cure for uterine fibroids is a hysterectomy. This procedure results in permanent infertility; a woman will be unable to have children. A hysterectomy is major surgery. All of the possible risks of surgery listed above are the same for hysterectomy.
Embolization
Uterine Fibroid Embolization (UFE) or Uterine Artery Embolization (UAE) - a nonsurgical procedure that blocks blood flow to fibroids in the uterus. Embolization is done with local anesthesia, and there are no incisions or cuts in the skin. A thin flexible tube is threaded into the blood vessels that supply blood to the fibroid; a solution is then injected into the blood vessels. This blocks the blood supply to the fibroid, causing it to shrink. Fibroids treated with embolization shrink by half or more. Normal uterine tissue usually remains unharmed, because it is supplied by other arteries.
Pregnancy is possible after embolization, but the risks to pregnancy after embolization are not fully known. Embolization is a procedure for women who do not want to have children in the future.
Women who are considered the best candidates for embolization are women who:
- Have fibroids that are causing heavy bleeding
- Have fibroids that are causing pain or pressing on the bladder or rectum
- Don't want to have a hysterectomy
- Don't want to have children in the future
Complications of embolization are not common, but can occur. They are:
- Infection - the most serious, potentially life-threatening complication of embolization. See your doctor immediately if you have a high fever and feel ill or notice pus in your vaginal discharge. In rare cases, emergency hysterectomy is needed to treat an infected uterus.
- Loss of menstrual periods
- Premature menopause
- Scar tissue formation
It is important to note though that all women are different and treatment may vary. Only your health care provider can provide you with the best options to treat uterine fibroids.
Are new treatments for uterine fibroids being developed?
There are several new ways of destroying fibroid tissue or removing fibroids. These methods are not yet standard treatments so your health care provider may not offer them and your health insurance may not pay for them.
If your doctor offers one of these procedures, ask:
- How many of the procedures he or she has done,
- How successful they have been,
- What kinds of problems can result, and
- Whether your insurance covers the procedure.
Myolysis
Myolysis is the destruction of muscle tissue. Myolysis is generally recommended for smaller fibroids. It is not recommended for women who hope to have children. These treatments can cause serious pregnancy complications, such as uterine scarring and infection; these can be dangerous to both mother and fetus.
- Laser (myolysis) - usually done by laparoscopy. A laser is used to remove the fibroid or clot the blood supply to the fibroid, causing the fibroid to shrink and eventually die.
- Cold (cryomyolysis) - usually done by laparoscopy. Liquid nitrogen is used to freeze the fibroid.
- Electric current - Myoma coagulation (myolysis) - usually done by laparoscopy. An electrical needle is passed directly into the fibroid delivering high-temperature energy to destroy both the fibroid and the blood vessels feeding it.
- High-frequency focused ultrasound - Using a high-intensity ultrasound beam, the Magnetic Resonance Imaging (MRI) scanner helps the doctor locate the fibroid, and the ultrasound sends out very hot sound waves to destroy it.
New Medications
New anti-hormonal drugs and other medications are being studied for treatment of fibroids, but none are yet available or Federal Drug Administration (FDA)-approved for us in the US.
It is important you talk with your health care provider to fully understand your options for uterine fibroids that are causing you problems. If your health care provider is recommending a hysterectomy, be sure to ask why other options are not right for you. Remember, you can ask for a second opinion to be sure the treatment option is right for you.