DOH Medicaid Update January 2007 Vol. 22, No. 1
Office of Medicaid Management
DOH Medicaid Update
January 2007 Vol. 22, No. 1
State of New York
Department of Health
Medicaid Update
is a monthly publication of the
New York State Department of Health,
Office of Medicaid Management
Table of Contents
Annual Ambulette Survey for 2007 - Form
Attention: Transportation Ordering Providers
Issuance of 1099 Forms
Medicare Part D Drug Plan Problems Formal Complaint Process
Medicare Part D Drug Plan Complaint Process Tip Sheets
Preferred Drug Program Update
Mandatory Generic Drug Program Update
NYS Medicaid Smoking Cessation Policy
NYS Medicaid Recipient Stop Smoking Coverage Fact Sheet
Medicaid Reimbursement for Immunizations in Article 28 Hospital-Based Freestanding Clinic Settings
Comprehensive Medicaid Case Management Providers: Payment Guidelines
Attention Physicians and Clinics: Service Authorization Exception Code 7- Special Handling
UB92 Form to be Replaced by UB04 Form
ePACES Enrollment
Attention Private Duty Nursing Providers: Billing Reminders
Medicaid Recipients with Medicare Managed Care (HMO/MCO) Coverage
Seminar and Schedule Registration
Most Integrated Setting Coordinating Council Authorizes Initial Report
Announcement from Medicaid Inspector General Kimberly A. O'Connor
First in Nation: Oral Health Care During Pregnancy and Early Childhood Practice Guidelines Issued
Sickle Cell Disease in New York's Medicaid Population: An Underutilization of Drug Therapy (Hydroxyurea)
Juvenile Arthritis
Weathering the Storm: Important Advice to Individuals Receiving Dialysis Treatment
Older Adult Falls Can Be Prevented
Provider Services
ATTENTION
AMBULETTE PROVIDERS
Annual Ambulette Survey for 2007
Return to Table of Contents
Providers of Ambulette services are required to submit vehicle information on an annual basis in accordance with Title 18 NYCRR (New York Code, Rules and Regulations) 502.6(b):
Each provider of ambulette services must, during the month of January of each year, disclose to the department in writing, information concerning those vehicles currently owned or leased by the provider.
The information to be disclosed must include at a minimum the name and address of the provider, each vehicle's license number and Department of Transportation identification number and a statement regarding whether the vehicle is owned or leased.
A provider of ambulette services that fails to disclose this information may have its participation in the medical assistance program terminated.
Failure to comply may result in the termination of enrollment as a Medicaid provider.
The form on the following page must be returned by February 15, 2007 to:
Investigations & Enforcement
Attn: 2007 Ambulette Survey
150 Broadway, 4th Floor
Albany, NY 12204-2719
Certified/Return Receipt mail is suggested. A copy of the form and proof of mailing should be retained for your records. In the event of non-receipt of the form by the Office of the Medicaid Inspector General, this proof will be used to validate compliance.
Annual Ambulette Survey for 2007
Return to Table of Contents
Date:_______________________
Provider Name:________________________________________________________________
Provider Address:______________________________________________________________
____________________________________________________________________________
____________________________________________________________________________
Provider Phone #:__________________________________________
eMedNY Provider #:_____________________________________________________
Name of Person Completing This Form:_____________________________________________
Title of Person Completing This Form: _____________________________________________
Signature of Person Completing This Form:__________________________________________
DAYS OPEN AND HOURS OF OPERATION
S ______ M _______ T _______ W _______ TH ______ F _______ S _______
| Check One | |||||
| DMV Plate Number | Vehicle Identification Number (VIN#) | Passenger Capacity | Owned | Leased | Leased from |
NYS DOT OPERATING CERTIFICATE #_________________________________________

Transportation Ordering Providers
Return to Table of Contents
To order transportation of Medicaid clients, you must make your request by following the procedures established by the local department of social services (DSS) of the county which retains fiscal responsibility of the client.
DSS information can be found in the Information for All Providers - Inquiry Manual online at:
http://www.emedny.org/ProviderManuals/AllProviders/index.html
Questions? Please contact the Medicaid Transportation program at:
(518) 474-9219
or email
MedTrans@health.state.ny.us
ATTENTION
PHYSICIANS AND CLINICS
Issuance of IRS Form 1099
Return to Table of Contents
Computer Sciences Corporation, eMedNY contractor for the Department of Health, issues IRS (Internal Revenue Service) Form 1099 to providers at the beginning of each year for the previous year's Medicaid payments.
The IRS 1099 amount is not based on the date of the checks;
rather,
it is based on the date the checks were released to providers.
Due to the two-week check lag between the date of the check and the date the check is issued, the IRS 1099 amount will not correspond to the sum of all checks issued for your provider identification number during the calendar year. The IRS 1099 amount is based on check release date.
The IRS 1099 that will be issued for the year 2006 will include the following:
- Check dated 12/19/05 (Cycle 1478) released on 01/04/2006 through,
- Check dated 12/11/06 (Cycle 1529) released 12/27/06.
Additionally, in order for group practice providers to direct Medicaid payments to a group identification number and corresponding IRS 1099, providers are reminded that they must submit the group identification number in the appropriate field on the claim (paper or electronic). Claims that do not have the group identification number entered will cause payment to go to the individual provider and his/her IRS 1099.
IRS 1099s for the year 2006 will be mailed no later than January 31, 2007.
The above information is provided to assist providers with reconciling the IRS 1099 amount.
Any questions should be directed to the eMedNY Call Center at:
(800) 343-9000.
Medicare Part D Drug Plan Problems
Formal Complaint Process
Return to Table of Contents

Problems obtaining drug coverage from a Medicare Part D plan?
- Work with the plan first.
- If you are not satisfied with the plan's response, contact 1-800-MEDICARE.
Prescribers, pharmacists and recipients who are experiencing difficulties obtaining medically necessary drug coverage from Medicare Part D plans are encouraged to work with the plans toward resolution.
However, if you believe a Part D plan has not provided a satisfactory response, to register a formal complaint, you should contact Medicare at:
1-800-MEDICARE
This is an opportunity to give input on the oversight and evaluation of the Part D plans - the information provided is used by the federal government to monitor plans' compliance with their contractual obligations to provide beneficiaries with the drug benefits to which they are legally entitled.
A tip sheet describing the complaint process is available at the following website. Please copy and hand out.
http://www.cms.hhs.gov/partnerships/downloads/PartnerTipSheetPartDComplaints081706.pdf

Medicare
covers prescription smoking cessation products for beneficiaries who have Medicare Prescription Drug Program coverage.
Medicaid
covers over-the-counter smoking cessation agents.
Preferred Drug Program
Return to Table of Contents

What is the procedure for newly FDA approved prescription drugs subject to the Preferred Drug Program (PDP)?
In June 2006, the Medicaid Pharmacy and Therapeutics (P&T) Committee unanimously recommended that drugs newly approved by the Food and Drug Administration (FDA), in categories subject to the PDP, be added to the Preferred Drug List (PDL) as non-preferred until the P&T Committee completes their annual review of the specific therapeutic drug class. That recommendation was subsequently approved by the Commissioner of Health.
Therefore, prescription drugs newly approved by the FDA, in classes already on the PDL, will be added to the PDL as "non-preferred" until they are reviewed by the P&T Committee.
Providers should be aware that the addition of newly approved drugs to the PDL may occur without notification.
The Office of Medicaid Management will continue to notify providers directly to announce the addition of new drug classes to the PDL.
The most current PDL can be found at:
http://www.nyhealth.gov or http://newyork.fhsc.com
Or you can call the clinical call center for a faxed copy at:
1-877-309-9493
Prescriber Reminder!
If you write a prescription for a proton-pump inhibitor (PPI), remember that Nexium, Prevacid capsules, and Prilosec OTC are preferred products and do not require prior authorization.
Note: When prescribing a non-preferred PPI or a non-preferred Second Generation Antihistamine, prior authorization is obtained through the staffed prior authorization clinical call center at the telephone number above.
Questions? Please call 1-877-309-9493.
MANDATORY GENERIC DRUG PROGRAM UPDATE
Changes Effective February 1, 2007
Return to Table of Contents
The following list of drugs has had generic equivalents available for six months or longer, and requires prior authorization from the Mandatory Generic Program, effective February 1, 2007.
Remaining refills of current prescriptions written prior to this date, but filled on or after February 1, 2007, will not require prior authorization.
When a current prescription expires, a prior authorization will be required for the patient to continue to receive the brand-name drug.
PRESCRIPTIONS FOR GENERIC EQUIVALENTS OF THESE DRUGS DO NOT REQUIRE PRIOR AUTHORIZATION.
BRAND NAME DRUGS REQUIRING PRIOR AUTHORIZATION
EFFECTIVE FEBRUARY 1, 2007
| ADOXA 50, 100 MG TABLET | LOCOID 0.1% OINTMENT |
| AMARYL 1 MG, 2MG, 4MG TABLET | LOESTRIN FE 1.5/30, 1/20 TABLET |
| AMIKIN 250 MG/ML VIAL | LOPROX 0.77% CREAM |
| ANAFRANIL 25 MG, 50MG, 75MG CAPSULE | MEDROL 8 MG TABLET |
| ANCEF 500MG, 1 GM, 10 GM VIAL | METAGLIP 2.5/250 MG, 2.5/500MG, 5/500MG TAB |
| AUGMENTIN 250-125 TABLET | METROLOTION TOPICAL 0.75% |
| BENADRYL 50 MG/ML SYRINGE, VIAL | MOBIC 7.5MG, 15 MG TABLET |
| BENTYL 10 MG/5 ML SYRUP | NEOSPORIN G.U.IRR 40 MG/ML |
| CAFCIT 20 MG/ML ORAL SOLN, VIAL | NEURONTIN 600 MG, 800 MG TABLET |
| CARNITOR 1 GM/5 ML VIAL | NORINYL 1+50-28 TABLET |
| CEFZIL 125 MG/5 ML, 250MG/5 ML SUSP | NOVANTRONE 2 MG/ML VIAL |
| CEFZIL 250 MG, 500 MG TABLET | PARLODEL 5 MG CAPSULE |
| CLAFORAN 500 MG, 1 GM, 2 GM VIAL | PENTAM 300 VIAL |
| CLEOCIN 2% VAGINAL CREAM | PHRENILIN W/CAFF/CODEINE CP |
| CLEOCIN PHOS 150 MG/ML VIAL | RETROVIR 10 MG/ML SYRUP |
| CLOMID 50 MG TABLET | RETROVIR 100 MG CAPSULE |
| CONDYLOX 0.5% TOPICAL SOL | ROBINUL 0.2 MG/ML VIAL |
| COPEGUS 200 MG TABLET | ROCEPHIN 250MG, 500MG, 1GM, 2GM, 10 GM |
| CUTIVATE 0.005% OINTMENT | SALAGEN 5 MG TABLET |
| CYTOXAN 25 MG TABLET | SANDOSTATIN 0.2 MG/ML, 1MG/ML VIAL |
| CYTOXAN 500 MG, 1 GM, 2 GM VIAL | SEDAPAP TABLET |
| DARVOCET A500 TABLET | SOLU-CORTEF 500 MG ACT-O-VL |
| DDAVP 0.01% NASAL SPRAY | SOLU-MEDROL 125 MG VIAL |
| DDAVP 0.1 MG, 0.2 MG TABLET | TEMOVATE 0.05% CREAM, OINTMENT |
| DECLOMYCIN 150 MG, 300 MG TABLET | TEMOVATE E 0.05% CREAM |
| DEPO-PROVERA 150 MG/ML SYRN, VIAL | TERAZOL 3 80 MG SUPPOSITORY |
| DIDRONEL 200 MG, 400MG TABLET | TERAZOL 7 CREAM |
| DILAUDID-HP 10 MG/ML VIAL | TESSALON PERLE 100 MG CAP |
| DOSTINEX 0.5 MG TABLET | TRIDESILON 0.05% CREAM, OINTMENT |
| DURICEF 250 MG/5 ML, 500 MG/5ML SUSP | TRI-NORINYL 28 TABLET |
| DYNACIN 75 MG TABLET | ULTRAVATE 0.05% CREAM, OINTMENT |
| EFUDEX 2%, 5% SOLUTION | UNASYN 1.5 GM, 3GM VIAL |
| ELOCON 0.1% CREAM, LOTION | UROCIT-K 5 MEQ,10 MEQ TABLET SA |
| ESTRADERM 0.05 MG, 0.1 MG PATCH | XANAX XR 0.5 MG, 1MG, 2MG, 3MG TABLET |
| FLEXERIL 5 MG TABLET | ZANTAC 25 MG/ML VIAL |
| FOSCAVIR 24 MG/ML INFUS BTT | ZINACEF 750MG, 1.5 GM VIAL |
| GABARONE 400 MG TABLET | ZITHROMAX 100 MG/5 ML , 200MG/5ML SUSP |
| GLUCOTROL XL 2.5 MG TAB SA | ZITHROMAX 250 MG, 500MG, 600MG TABLET |
| INTAL NEBULIZER SOLUTION | ZOLOFT 25MG, 50MG, 100 MG TABLET |
| KANTREX 1 GM/3 ML VIAL | ZOLOFT 20 MG/ML ORAL CONC |
| KEFLEX 250 MG, 500 MG CAPSULE | ZONEGRAN 50 MG, 100 MG CAPSULE |
| KLONOPIN WAFERS 0.125 MG, 0.25MG, 0.5MG, 1MG, 2MG |
For billing questions, call (800) 343-9000.
For clinical concerns or Mandatory Generic Drug Program questions, call (877) 309-9493
For Medicaid pharmacy policy and operations questions, call (518) 486-3209
NYS MEDICAID
SMOKING CESSATION POLICY
Return to Table of Contents

- Smoking cessation therapy consists of prescription and non-prescription agents. Covered agents include nasal sprays, inhalers, Zyban (bupropion), Chantix (varenicline), over-the-counter nicotine patches and gum.
- Two courses of smoking cessation therapy per recipient, per year are allowed. A course of therapy is defined as no more than a 90-day supply (an original order and two refills, even if less than a 30 day supply is dispensed in any fill).
- If a course of smoking cessation therapy is interrupted, it will be considered one complete course of therapy. Any subsequent prescriptions would then be considered the second course of therapy.
- Some smoking cessation therapies may be used together. Professional judgment should be exercised when dispensing multiple smoking cessation products.
- Duplicative use of any one agent is not allowed (i.e., same drug and same dosage form and same strength).
- For all smoking cessation products, the recipient must have an order. A prescription is the terminology for an order of a prescription product. A fiscal order refers to an order, which looks just like a prescription-written on a prescription blank, for an over-the-counter product.
- NYS Medicaid reimburses for over-the counter nicotine patches. Prescription nicotine patches are no longer reimbursed.
RESOURCES
NYS SMOKERS' QUITLINE (866) NY-QUITS (866-697-8487)
American Cancer Society 1-800-227-2345
American Lung Association 1-800-585-4872
Centers for Disease Control and Prevention 1-800-CDC-4636 (1-800-232-4636)
National Cancer Institute 1-800-4-CANCER (1-800-422-6237)
For more information on the New York State Medicaid Smoking Cessation policy, please call
the Bureau of Pharmacy Policy and Operations at:
(518) 486-3209.
NYS MEDICAID RECIPIENT
STOP SMOKING COVERAGE FACT SHEET
Return to Table of Contents
POLICY

- Stop smoking products to help you quit smoking can be obtained with a prescription. Medicaid will pay for inhalers, nasal sprays, Zyban (bupropion), Chantix (varenicline), over-the-counter nicotine patches and gum.
- Your health care provider must write a prescription for you to receive either a prescription or over-the-counter stop smoking product.
- You are allowed a course of stop smoking therapy twice a year. A course of therapy is defined as no more than a 90-day supply (an original order and two refills, even if less than a 30 day supply is dispensed in any fill).
- Some smoking cessation therapies may be used together. For example, Zyban, taken by mouth, and nicotine patches, which are applied to the skin, may be used at the same time. Ask your physician and pharmacist what is appropriate for you.
RESOURCES
There are many cost free programs and resources available to help you quit and stay tobacco free. Some are listed below.
NYS SMOKERS' QUITLINE (Toll-free) 1-866-697-8487
| RESOURCES Local cessation support program information can be obtained from: New York State Smokers' Quitline Toll-free: 1-866-697-8487 American Cancer Society Toll-free: 1-800-227-2345 American Lung Association Toll-free: 1-800-586-4872 |
| BROCHURES AND OTHER INFORMATION Centers for Disease Control and Prevention Toll-free: 1-800-232-4636 National Cancer Institute Toll-free: 1-800-4-CANCER (1-800-422-6237) |
In the December 2006 Medicaid Update, the article on Reimbursement for Immunizations did not contain correct policy.
The article below is updated and contains corrected policy. Providers need to be aware of the changes in billing, as stated in the table.
Medicaid Reimbursement for Immunizations in
Article 28 Hospital-Based and Freestanding Clinic Settings
Return to Table of Contents
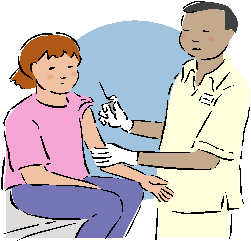
Change of Medicaid Payment Policy
An article printed in the September 2001 Medicaid Update provided billing guidance for influenza immunizations provided in the clinic setting.
This article reflects a change in policy.
Please refer to the chart below when billing for immunizations provided in an Article 28 facility.
Definitions Required For Chart Use
- A registered clinic patient is one whose primary source of medical care is received from the Article 28 facility.
- When services are provided to a registered clinic patient, the facility bills Medicaid their all-inclusive threshold clinic rate. It is expected that all necessary services should be provided on that date, including necessary immunizations and/or injections. Occasionally, this is not possible. A registered clinic patient service does not qualify for reimbursement as an ordered ambulatory service; however, in some scenarios presented below, you will note specific exceptions where we allow fee-for-service billing.
- An ordered ambulatory patient is one who has been referred to the clinic for a specific service. The referring practitioner is not affiliated with the Article 28 facility which is providing the ordered ambulatory service. Such services may include a singular occasion of service or a series of tests or treatments.
- Claims for ordered ambulatory services are paid on a fee-for-service basis and not at the all-inclusive threshold clinic rate. The billing provider must have the Ordered Ambulatory Category of Service (0163 for freestanding Diagnostic and Treatment Centers; 0282 for hospital-based outpatient clinics).
- A qualifying threshold visit is one where the registered clinic patient has an encounter with a physician, physician assistant, nurse practitioner or licensed midwife for services that include comprehensive primary care. A qualifying visit is reimbursed at the all-inclusive clinic threshold rate.
| Patient Status | Visit/Services | Billing Guidance |
|---|---|---|
| Registered Clinic Patient (Any age) | Patient is receiving primary care services. | This is a qualifying threshold visit and is reimbursed at the clinic rate. |
| Registered Clinic Patient (Any age) | Patient is receiving primary care services and an immunization. | This is a qualifying threshold visit and is reimbursed at the clinic rate. |
| Registered Clinic Patient (Under 19 years of age) | Patient visits for immunization only. Vaccine is provided to the clinic by the Vaccines For Children (VFC) program. |
This is not a qualifying threshold visit. However, the clinic may bill the Healthcare Common Procedure Coding System (HCPCS) procedure code that represents the immunization provided, appended with the modifier 'SL' and will be paid as an Ordered Ambulatory service. Reimbursement will be for the immunization administration in the amount of $17.85. (From a regulatory perspective, this is not really an Ordered Ambulatory service. We are using the Ordered Ambulatory billing construct to allow VFC reimbursement.) |
| Registered Clinic Patient (19 years of age or older) | Patient visits for immunization only. The vaccine is not provided by the VFC program. | Immunizations should routinely be given as part of a qualifying threshold visit. Seasonal immunizations (e.g., influenza vaccine) may not be available at the time of a patient visit. It should be provided when available without billing for an additional threshold visit. A separate threshold visit may be billed only when immunization is medically contraindicated at the time of the encounter with the health provider, since it is expected that the patient's health status will be reassessed prior to immunization. When a patient must return to complete a series of vaccinations, a separate threshold visit for each encounter may be billed when provided by a recognized practitioner. |
| In a Products of Ambulatory Care (PAC) Clinic (Any patient, any age) | Patient is receiving an immunization only. The service is provided by a physician, physician assistant, nurse practitioner, or licensed midwife. | This is grouped and paid as a PAC reimbursement. |
| Ordered Ambulatory Patient (Under 19 years of age) | Patient visits for immunization only. Vaccine was provided by the VFC program. | This is NOT a qualifying threshold visit. However, the clinic may bill the HCPCS procedure code, appended with the modifier 'SL' and will be paid as an Ordered Ambulatory service. Reimbursement will be for the immunization administration in the amount of $17.85. |
| Ordered Ambulatory Patient(19 years of age or older) | Patient visits for immunization only. Vaccine is not provided by the VFC program. | This is NOT a qualifying threshold visit. However, the clinic may bill the HCPCS procedure code that represents the immunization provided at their actual acquisition cost for the vaccine +$2.00 for administration. |
Important Reminders
- For a clinic threshold visit to be billed to Medicaid, the patient must be seen by a recognized practitioner (e.g., physician, dentist, physician assistant, nurse practitioner, licensed midwife, physical/speech/occupational therapist, or psychologist).
- When a Medicaid beneficiary under the age of 19 years is immunized and the vaccine is provided by the VFC program, the SL modifier should be used.
Questions regarding this policy may be directed to the Bureau of Policy Development and Agency Relations at:
518-473-2160
Questions regarding the VFC Program should be directed to:
1-800-543-7468
or to the Immunization Program at:
518-474-4578
Clinics that do not have the Ordered Ambulatory Category of Service (0163 or 0282) should contact the Division of Medical Review and Provider Enrollment at:
518-474-8161
COMPREHENSIVE MEDICAID CASE MANAGEMENT PROVIDERS
Payment Guidelines
Return to Table of Contents

We are reaffirming the following payment guidelines to ensure the timely payment of Medicaid claims submitted by Comprehensive Medicaid Case Management providers.
- The client must be Medicaid eligible at the time the provider delivers services. It is the responsibility of the provider to verify Medicaid eligibility at each visit via the Medicaid Eligibility Verification System (MEVS) before providing services to the Medicaid client. Medicaid eligibility may be verified via the MEVS Card Swipe procedure, by using the Audio Response Unit at 1-800-997-1111 or via ePACES (web-based program).
- The client must be enrolled with an Exception Code 35 in the Welfare Management System (WMS) Restriction/Exception Subsystem (R/E) by the local department of social services (LDSS) responsible for the client's Medicaid benefits. The OMRDD Revenue Support Field Operations enters R/E Code 35 for OMRDD's Medicaid Service Coordination (MSC) program.
If you bill monthly, the enrollment "From Date" recorded on the enrollment request should be the first date service was provided in the month. If you are disenrolling and are a monthly biller, the disenrollment "Thru Date" must be the first of the month following the last date you provided services to the recipient. If the client is not Medicaid eligible on the date of service, the LDSS will be unable to enroll the client with the R/E Code 35, and thus, the claim will be rejected.
Enrollment in the WMS R/E Subsystem accomplishes the following:
- It identifies the client as an appropriate member of the target population;
- It confirms that the client has freely chosen to participate in the program;
- It links the client to the provider number of the specific Case Management Program providing service; and
- It establishes a specified "From and Thru Date". Claims for Case Management services provided outside the enrollment time frames will not be paid.
- The client must be enrolled in the Case Management program providing services. Registration in that program in the WMS R/E Subsystem will only continue as long as the client is willing to accept
services from that provider. If the client decides to change providers, the LDSS must be notified so that the registration will be changed to reflect the new provider's Identification Number effective as of the date the new provider rendered Case Management services.
A Medicaid eligible client is referred to a Case Management provider either by the LDSS, another agency, or through self-referral. The client may choose to accept professional services from the referred provider, to seek service from another provider, or to reject case management services completely. - If the client has been determined to be Medicaid eligible, is enrolled in the WMS R/E Subsystem, and is enrolled with the Case Management Program providing services, the initial Medicaid claim submission should be no sooner than one day after the provider received verification of successful enrollment in Case Management by the LDSS. In OMRDD's MSC program, the date of service for MSC claims is the first day of the month following provision of services.
- The client must be enrolled in the Case Management program providing services. Registration in that program in the WMS R/E Subsystem will only continue as long as the client is willing to accept
services from that provider. If the client decides to change providers, the LDSS must be notified so that the registration will be changed to reflect the new provider's Identification Number effective as of the date the new provider rendered Case Management services.
To assist Case Management Providers with enrollment, disenrollment, and changes to the Case Management information in the WMS R/E Subsystem, the Office of Medicaid Management (OMM), in conjunction with LDSS, is offering forms, plus instruction sheets for enrollment and disenrollment of recipients into Comprehensive Case Management. These forms are modeled on forms used in New York City, and are being offered for use by OMM and the LDSS to providers serving the rest of the State.
To obtain forms and instructions to fill them out, please contact your LDSS Case Management contact person or go to our website at:
http://www.emedny.org/ProviderManuals/CMCM/index.html
Return completed forms to your usual contact person in the LDSS responsible for the Medicaid coverage of the client to whom you are providing Case Management services. Please enclose a self- addressed, stamped envelope, so that verification of the processed enrollments, disenrollments, and/or changes can be returned to you promptly.
If the enrollment or disenrollment forms have not been returned to the provider within 30 days of the date they were sent to the LDSS, the provider should contact the LDSS to determine the status of the enrollment/disenrollment/change.
It is the provider's responsibility to keep track of the form requests sent to and returned from the LDSS.
Providers may not submit a claim until successful enrollment verification has been sent to them by the LDSS.
The LDSS responsible for the client's Medicaid eligibility is also responsible for notifying providers within ten calendar days of the denial of a registration, or termination of an existing registration.
The LDSS IS NOT responsible for notifying providers when a client loses Medicaid eligibility.
Providers are encouraged to notify the LDSS within ten calendar days of any changes which would affect the client's need or eligibility for Case Management services. Providers should also notify the LDSS on a timely basis when they are no longer providing Case Management services to the client.
PROGRAM SPECIFIC VARIATIONS - OMRDD Clients
The Office of Mental Retardation and Developmental Disabilities administers its Medicaid Service Coordination (MSC) program through the 13 regional Developmental Disabilities Services Offices (DDSOs).
All MSC enrollments and terminations must be approved by the DDSOs. Persons authorized by the DDSO to receive services are notified of the enrollment and persons removed from the program are notified of the termination by OMRDD.
OMRDD Revenue Support Field Operations staff are responsible for processing the R/E Code 35 transactions for MSC into the WMS R/E Subsystem.
CLAIM EDITING - The following information refers to claim editing performed by Computer Sciences Corporation during claims processing.
Edit 01338 - "Recip not on the Rest Recip File" (The Recipient is not on the Restriction/Exception Recipient File) - This means that the recipient is not enrolled with a R/E Code 35 in the WMS R/E Subsystem.
Solution: Send the enrollment form to the LDSS and track the return of the form from LDSS indicating that successful enrollment to your provider identification number has occurred. When you receive verification of enrollment from the LDSS, re-submit the claim at least one day after the LDSS transaction input date shown on the form. OMRDD MSC vendors should contact their local Revenue Support Field Offices for assistance when this edit is encountered. RSFO contact information is available on the OMRDD website.
Edit 01339 - "Recip not Authorized for CMCM on SVC DT" (Recipient not authorized for Case Management Services on the Service Date). This means that the client is correctly enrolled with a R/E 35 to your provider identification number. However, the enrollment period on file does not include all or part of the dates of service for which payment is requested.
Solution: Check the enrollment form returned from the LDSS. Is the R/E 35 begin date you requested successfully entered? Are you billing for dates of service prior to the requested enrollment "From" date?
If the enrollment form returned by the LDSS indicated successful entry of R/E 35, check to see if the enrollment "From" date you requested was the correct date for which you provided service. Be aware that if you are a monthly biller, the "FROM" date should be the first date service was provided in the month. If you sent an incorrect "From" date of service for enrollment, re-send an enrollment form with the corrected "From" date. Note that this is a correction to your original "From" date request.
If the enrollment form returned by the LDSS has a reason stating that a current restriction already exists, follow the instructions given in the solution to Edit 01340 below.
If the enrollment form returned from the LDSS has a reason stating that the "Individual Has No MA Coverage For The Enrollment Request", it means that the client was not enrolled with a WMS R/E 35 for the "From" date of service you requested because the client was not Medicaid eligible on that date. This indicates that you did not verify the client's eligibility through MEVS. Contact the LDSS to enroll the client with WMS R/E 35 with the "From" date equal to the client's first date of Medicaid eligibility. Resubmit the claim at least one day after the LDSS has enrolled the client with WMS R/E 35.
EDIT 01340 - "Claim Prov. Not Equal Rest Recip File Prov" (Claim Provider is not equal to the Restriction/Exception Recipient File Provider). This means that the client is enrolled with a R/E Code 35 but is enrolled to a different provider.
Solution: The enrollment form returned by the LDSS would have a reason stating that the current restriction already exists and the name of the "other" provider listed on the returned enrollment form. You, the new provider, should then contact the "other" provider asking that the "other" provider send a disenrollment form to the LDSS. This would allow the" other" provider to disenroll the client from their care, and for you to begin service with an appropriate "From" date by sending your enrollment form to the LDSS. The change form could also be used. Resubmit the claim at least one day after the LDSS has enrolled the client with you as the provider.
WMS systems questions can be directed to the WMS Upstate Eligibility Systems at:
(518) 473-4040
Policy questions can be directed to the Bureau of Policy Development and Agency Relations at:
(518) 473-2160.
Billing questions can be directed to the eMedNY Call Center at:
(800) 343-9000.
ATTENTION
PHYSICIANS AND CLINICS
Service Authorization Exception Code 7
Special Handling
Return to Table of Contents
Use of the Service Authorization (SA) Exception code 7 - Special Handling affects more than Utilization Threshold (UT) Service Authorization edits:
- This code is necessary, in certain instances, to assign a UT exempt specialty to the claim during processing.
- The assignment of the exempt specialty code to the claim may also affect pricing of the claim and certain managed care related edits.
For a list of physician specialties exempt from UT, physicians may refer to Appendix A of the Physician's Provider Manual at:
http://www.emedny.org/ProviderManuals/Physician/index.html
In addition, a list of UT exempt specialty codes may be found in the 837 Professional Supplemental CG or the 837I Institutional Supplemental CG under eMedNY Companion Guides and Sample Files under NYHIPAADESK at:
http://www.emedny.org/HIPAA/index.html
Providers submitting claims for a specialty exempt from Utilization Threshold service authorization must enter the SA exception code 7 on their claims.
- On the eMedNY 150001 -claim form, the SA Exception Code is entered in field 25D.
- On the 837P and 837I, the SA Exception Code is entered in Loop 2300 Data Element REF01=Qualifier 4N and REF02=SA Exception Code.
In instances when the provider has multiple UT exempt specialties on their provider file, use of SA Exception Code 7 does not guarantee assignment of the desired specialty code to the claim. The SA Exception Code 7 causes the system to assign the first SA exempt code it finds on the providers master file.
Questions regarding SA Exception Codes? Please contact the eMedNY Call Center at:
(800) 343-9000

UB92 Form to be Replaced by UB04 Form
Return to Table of Contents
Rate-based providers who use the paper claim form UB92 should be aware that this form will be replaced by the UB04 form during the second quarter of 2007.
Upon acceptance of the UB04 form by the NYS Medicaid program, there will be a transition period of approximately three months where NYS Medicaid will accept both the UB92 and the UB04 claim forms.
Specific dates will be announced before these changes occur.
The following is a list of Form Locators (FL) from the new UB04 form and the changes that will impact how the UB04 is completed for submission to the program.
| UB04 FORM LOCATOR NUMBER | UB04 FORM LOCATOR NAME | DESCRIPTION OF CHANGE |
|---|---|---|
| 3a | PATIENT CONTROL NUMBER | FL 3 on UB92 |
| 7, 8, 9, 10 | COV'D, N-CD, C-IN, L-RD | Removed - information moved to Value Code Section FLs 39-41. |
| 8b | PATIENT NAME | FL 12 on UB92 |
| 10 | BIRTHDATE | FL 14 on UB92 |
| 11 | SEX | FL 15 on UB92 |
| 14 | ADMISSION TYPE | FL 18 on UB92 |
| 17 | STAT | Fl 22 on UB92 |
| 18 - 28 | CONDITION CODES | FLs 24 - 30 on UB92 |
| 31 - 34 | OCCURRENCE CODES | Ls 32 - 36 on UB92 |
| 39 - 41 | VALUE CODES | Covered Days, Non-covered Days and Co-insurance days will be reported here using the following codes. Value Code 80=Covered Days, Value Code 81=Non-Covered Days and Value Code 82=Co-insurance Days. |
| 51 | HEALTH PLAN ID | Will not be used by NYS Medicaid, see FL 57 below. |
| 56 | NPI | New FL for billing provider's National Provider ID to be used upon NPI implementation by NYS Medicaid. |
| 57 | OTHER PRV ID | FL 51 on UB92. Used to report the billing provider's Medicaid ID. |
| 64 | DOCUMENT CONTROL NUMBER | FL 37 on UB92. Used to report a TCN for replacing or voiding a previously paid claim. |
| 78 | OTHER | FL 83 on UB92. Used to report ordering provider NPI and Medicaid ID or License Number/Profession Code information. |
Specific instructions related to these changes will be provided along with updates to your Provider Manuals and will be posted to the website at: http://www.emedny.org, prior to the second quarter of 2007.
Please note that there is no space provided on the UB04 form for a submitter's signature. Providers submitting these paper forms must have an active certification on file with at least one Electronic Transmitter Identification Number (ETIN). Providers submitting electronic claims should already have a certification on file. Providers only submitting paper UB04 forms can locate certification instructions on the eMedNY website under "Provider Enrollment Forms", then select "Electronic Transmitter Identification Number (TSN/Provider)".
UB04 claim forms are not provided by NYS Medicaid but may be obtained from your national supplier.
Please adjust your supply of UB92 forms so you are prepared to begin using the UB04 claim form.
Questions? Please contact the eMedNY Call Center at:
1-800-343-9000.
ePACES Enrollment
Return to Table of Contents

Providers Must Have Their Own Electronic Transmitter Identification Number (ETIN) to Enroll in the electronic Provider Assisted Claim Entry System, ePACES.
Providers wishing to enroll in ePACES must not enroll in ePACES with an ETIN that belongs to a service bureau or a group practice to which the provider has disassociated himself/herself. You can tell if an ETIN belongs to a service bureau because the ETIN begins with the number 0 (Zero). If this is the only ETIN a provider has, he/she must apply for a separate provider ETIN by contacting the eMedNY Call Center at the number below to get the ETIN application and the associated Certification Statement or by visiting http://www.emedny.org/info/ProviderEnrollment/index.html.
ePACES is a web-based application available to enrolled Medicaid providers. ePACES allows for the following types of transactions:
- Claims
- Claim status requests
- Prior approval requests
- Eligibility requests
- Utilization Threshold service authorizations
Some advantages of using ePACES are:
- Professional "real-time" claims are processed instantly and the status of the claim and, if approved, the amount paid are available immediately after submission.
- ePACES provides data validation to reduce errors and time consuming resubmissions.
- The status of any claim regardless of the mode of submission is available via ePACES.
ePACES enrollment also enrolls a provider in eMedNY eXchange. If a provider wishes to receive electronic remittance via eXchange, he/she should call Computer Sciences Corporation (CSC) to have the eXchange inbox activated and to submit an Electronic Remittance Request Form. The form is available on the same website page as the ETIN Application referenced above. The advantage of electronic remittances is that they are delivered two and a half weeks earlier than paper remittances.
Please note electronic remittances are delivered in a HIPAA-compliant "835" format and software will be needed to interpret the remittance information. Software is available from a number of software vendors posted on the eMedNY website at:
http://www.emedny.org/HIPAA/Vendors/NYSDOH%20SOFTWARE%20VENDOR%20LIST.pdf
To find a vendor with software to interpret a HIPAA remittance, look in the Transaction Capabilities column of the vendor list for "835".
Questions about ePACES enrollment, or eXchange activation should be directed to the eMedNY Call Center at:1-800-343-9000.
ATTENTION
PRIVATE DUTY NURSING PROVIDERS
BILLING REMINDERS
Return to Table of Contents
The Private Duty Nursing manual is updated frequently with information regarding Medicaid policy, procedures and billing requirements. The manual is available online at: http://www.emedny.org/ProviderManuals/NursingServices/index.html
As a provider, it is your responsibility to check this website on a regular basis to ensure you are current with the latest policy and billing information.
If you do not have access to the internet, you must contact Computer Sciences Corporation at: (800) 343-9000 to receive a hard copy of the provider manual.
Please keep the following billing guidelines in mind when billing for Private Duty Nursing services.
- Medicaid regulations require that claims for payment of medical care or services to eligible recipients be initially submitted within 90 days of the date of service, unless the claim is delayed due to circumstances outside the control of the provider. Claims over 90 days from the original date of service require a 90 day cover letter for paper claims or a valid delay reason code for electronic claims. Acceptable reasons for a claim to be submitted beyond 90 days can be found at the following websites:
- Under certain circumstances, your procedure code must be expanded by a two-digit modifier to further explain or define the nature of the procedure.
- The modifier "U1" must be added to indicate services approved by Care at Home Waiver Program.
- The modifier "TT" must be added to indicate "concurrent/shared" cases (one nurse providing services to more than one recipient in the same setting).
- When two patients are simultaneously under the care of one private duty nurse (concurrent/shared cases), the normal hourly fee should be multiplied by 1.5 and divided by 2.
The resulting amount is the maximum that can be billed for each patient.
Example: An RN services two Medicaid patients simultaneously for 8 hours (procedure code S9123 - modifier TT). The associated example hourly $20.00 fee should be adjusted as follows for each patient:
$20 x 1.5 divided by 2 = $15 x 8 hours = $120 Total Charge
- Nurses providing "concurrent/shared" services through the Care At Home Program must indicate both modifiers "U1" and "TT" on claims.
- The total number of hours of service provided to a patient during the same day by the same nurse should be entered in one claim line even if the service was provided in separate shifts.
Example: An RN works two four-hour shifts (7AM to 11AM and 6PM to 10PM) for a total of 8 hours on July 1st. There would only be one claim line for July 1st and it would contain 8 units (hours). One hour of nursing service equals one unit.
- If the total number of hours of service provided to a patient extends over a period of two days, enter each date with the appropriate number of hours on separate lines.
Example: An RN works an 8-hour shift starting at 10PM on July 1 and ending at 6AM on July 2. The claim line for July 1 would contain two units (hours) and the claim line for July 2 would contain six units (hours). If the next shift of care started at 10PM on July 2, those two hours must be included on the same claim line as the other hours worked earlier on that date (a total of eight hours for July 2).
For billing questions, please contact Computer Sciences Corporation at (800) 343-9000
Medicaid Recipients with Medicare Managed Care (HMO/MCO) Coverage
Return to Table of Contents

- Medicare Advantage Plans are identified by a Claim Filing Indicator Code of 16 - Health Maintenance Organization (HMO) Medicare Risk - in loop 2320, data element SBR09. This code value will satisfy eMedNY's Medicare editing requirements.
- A new eMedNY edit number 2016, "Medicare MCO Qualifier 16 conflicts with Part A/B Qualifiers" is scheduled for implementation February 1, 2007. This edit will fail when the claim contains a Claim Filing Indicator Code of 16 along with a code of MA - Medicare Part A or MB - Medicare Part B.
- If the patient is enrolled in a Medicare Advantage plan there should be no Part A or Part B coverage for the same period.
- Claims spanning a period of time where the patient did have Medicare coverage under both fee-for-service and a managed care plan must be split billed.
- Inpatient DRG claims that span Medicare coverage types (fee-for-service and Advantage plan) need to be directed to Medical Review and Payment at 518-474-8161.
Instructions for Claims other than Nursing Home
- Medicaid will recognize the following Claim Adjustment Reason Codes (CARCs) as Patient Responsibility: 1 - Deductible, 2 - Coinsurance, 3 - Co-payment, and 122 - Psychiatric Reduction. The Claim Adjustment Group Code must be PR, "Patient Responsibility". All other CARCs with Claim Adjustment Group Code of "PR" will be treated as coinsurance.
- For all claim types except Nursing Home claims, when the Claim Filing Indicator Code of 16 is sent, the Medicaid payment amount will equal the Patient Responsibility total amount.
- When payer code is 'CI' then all claim types except Nursing Home will use the lower of
- Patient Responsibility amount (as requested by the commercial insurance); or
- The Medicaid price minus the prior payer's payment.
Nursing Home Claims
- If all days on the claim are reported as Medicaid Covered Days (loop 2300, QTY*CA) the system will determine the Medicaid value of the claim (Rate * Days = the amount Medicaid would have paid as the primary payer) and subtract the total of all prior payers' payments to receive the remaining balance.
For Medicaid recipients with nursing home inpatient coverage through a Medicare Managed Care plan, the Patient Responsibility - Deductible, Coinsurance, and Copay as appropriate can be billed. All the days must be entered as Medicare Coinsurance Days (loop 2320, QTY*CD). The reimbursement amount will be the total Patient Responsibility (deductible, coinsurance and copay).
- A new eMedNY edit number 2059, "Medicaid Days invalid on Medicare Managed Care Claim" is scheduled for implementation February 1, 2007. If a Nursing Home claim has both Medicaid full days and Coinsurance days with MCO involvement, then the claim will be denied for edit 2059. The claim must be split and two claims must be billed separately.
Medicaid Recipients with Commercial Insurance Coverage
Instructions for Claims other than Nursing Home
- The patient responsibility amount will be determined by adding the commercial insurance amounts as reported under the Adjustment Group Code for Patient Responsibility, 'PR' (in loop 2320, CAS segment) with Claim Adjustment Reason Codes 1 - Deductible, 2 - Coinsurance, and 3 - Co-payment (any other Patient Responsibility amounts will be treated as Coinsurance).
- The system will determine the Medicaid value of the claim (the amount Medicaid would have paid as the primary payer) and subtract the commercial insurance payment to get the remaining balance.
- The balance will be compared to the Patient Responsibility total and the lower of the two amounts will be paid. If insurance paid more than Medicaid would have paid as primary, the claim will pay zero.
Nursing Home Claims
- The system will calculate the Medicaid value of the claim, subtract the insurance paid amount, and pay the balance. There is no comparison to the Patient Responsibility amount.
Medicaid Recipients with Commercial Insurance and Medicare Managed Care (HMO/MCO) Coverage
Instructions for claims other than Nursing Home
- Pricing will use the Patient Responsibility entered for the last payer.
- For Enhanced Clinic pricing, the paid amounts of the Commercial payer and MCO will be added to the patient responsibility of the last payer to derive the approved amount.
Nursing Home Claims
- The system will subtract the total of the paid amounts for all payers from the Medicaid value of the claim.
Please note: in conjunction with the previously described claim valuation and payment calculation changed, the Office of the Medicaid Inspector General will be issuing recovery projects (through our third party liability vendor - Health Management Systems) that identify past system generated overpayments. The recovery projects will be targeted to Medicaid payments made with commercial coverage involvement.
Questions regarding Medicaid Managed Care should be referred to the Office of Managed Care at:
(518) 486-9015
or via email at: omcmail@health.state.ny.us omcmail@health.state.ny.us
Seminar Schedule and Registration
Return to Table of Contents
- Do you have billing questions?
- Are you new to Medicaid billing?
- Would you like to learn more about ePACES?
If you answered YES to any of these questions, please consider registering for a Medicaid seminar.
Computer Sciences Corporation (CSC) offers various types of seminars to providers and their billing staff. Many of the seminars planned for the upcoming months offer detailed information and instruction about Medicaid's web-based billing and transaction program the electronic Provider Assisted Claim Entry System (ePACES).
ePACES seminars are designed for specific provider types.
ePACES

ePACES allows enrolled providers to submit the following type of transactions:
- Claims
- Eligibility Verifications
- Utilization Threshold Service Authorizations
- Claim Status Requests
- Prior Approval Requests
Professional providers such as physicians, nurse practitioners, durable medical equipment providers, etc., and private duty nurses can even submit claims in "Real-Time" via ePACES.
Real-time means that the claim is processed within seconds and professional providers can get the status of a real-time claim, including the associated paid amount, without waiting for the remittance advice to be delivered.
Registration
Seminar locations and dates are available at the eMedNY website. Seminar registration is fast and easy. Seminars are free to enrolled Medicaid providers.
To find and register for the eMedNY Training Seminar appropriate for your provider category and location, go to:
http://www.emedny.org/training/index.aspx
Review the seminar descriptions carefully to identify the seminar appropriate to meet your training needs. Registration confirmation will be instantly sent to your email address.
If you are unable to access the internet to register, you may also request seminar schedule and registration information by contacting CSC's Fax on Demand at:
800-370-5809.
Request document number 1000 for a list of seminars and registration information to be faxed to you.
CSC Regional Representatives look forward to meeting with you at upcoming seminars!
Please contact the eMedNY call center (800) 343-9000, if you questions about registration.

Missing Issues?
The Medicaid Update, indexed by subject area, can be accessed online at the New York State Department of Health website:
http://www.nyhealth.gov/nysdoh/mancare/omm/main.htm
Hard copies can be obtained upon request by emailing:
Most Integrated Setting Coordinating Council Authorizes Initial Report
Return to Table of Contents
On November 20, 2006, the Most Integrated Setting Coordinating Council (MISCC), chaired by the Office of Mental Retardation and Developmental Disabilities Commissioner Thomas Maul, unanimously agreed to send its first report to the Governor and State Legislature.
The Council consists of representatives from eleven State agencies, consumers of services for individuals with disabilities, persons with expertise in community services for individuals with disabilities, and with expertise in, or recipients of, services available to senior citizens with disabilities.
The report, entitled Addressing the Service and Support Needs of New Yorkers with Disabilities, is available on the following website:
http://www.opwdd.ny.gov/MISCC/
The report establishes generally accepted "Principles and Guidelines" in keeping with the State's policy to provide long term care (LTC) services in the least integrated setting appropriate, and includes Council subcommittee ad hoc group recommendations for State action in the areas of:
- Assessment;
- Community Services;
- Data;
- Quality Assurance; and
- Transportation.
Final sections of the report set the Council's Operational Plan and describe State initiatives already underway that address the Council recommendations. Annual updates to the Operational Plan will reflect the progress and accomplishments of the Department and other State agencies.
Department staff will continue to participate in the quarterly Council meetings and activities consistent with the Department's ongoing efforts to rebalance the State's long term care Medicaid system.
The Council, established by law in 2004, is responsible for developing and implementing a comprehensive State Plan guided by the principles set forth under the federal Olmstead decision to empower individuals with disabilities of all ages to live more independently within their home community.
During the summer of 2004, the MISCC held four Constituent Forums around the State to gain input from consumers and providers to inform future program and service development. The forums focused discussion on existing natural community supports, the formal care system, local and/or networked transportation venues, and a shared constructive vision for a collaborative future approach to providing community-based services to the disabled. Since then, MISCC committees studied the presentations, related their findings to the Council at open public meetings, and continued discussions among the Council and ad hoc participants.
Questions? Please contact the Division of Consumer and Local District Relations at:
(518) 474-5271

Announcement From Medicaid Inspector General
Kimberly O'Connor
Return to Table of Contents
Medicaid Inspector General Kimberly A. O'Connor has announced the Office of the Medicaid Inspector General's (OMIG) new website:
The OMIG website contains such features as:
- An online complaint reporting mechanism.
- Current comprehensive listing of banned Medicaid providers.
- Significant news of OMIG initiatives and actions.
- Useful links to State and federal resources in the Medicaid field.
The OMIG consolidated staff and other Medicaid fraud detection, prevention, and recovery functions into a single more efficient and accountable Office, dramatically reorganized and streamlined the State's process of detecting and combating Medicaid fraud, waste, and abuse, and will seek to maximize the recovery of improper Medicaid payments.
The OMIG coordinates the Medicaid fraud, waste and abuse control activities of State executive agencies whose patients and clients are served by Medicaid, including:
- the Department of Health;
- the Office of Mental Health;
- the Office of Mental Retardation and Developmental Disabilities;
- the Office of Alcoholism and Substance Abuse Services;
- the Office of Children and Family Services; and
- the State Education Department.
The OMIG also works in a coordinated and cooperative manner with:
- the Deputy Attorney General for Medicaid Fraud Control;
- the Welfare Inspector General;
- federal prosecutors;
- district attorneys within the State;
- the special investigative units maintained by each health insurer operating within the State; and
- the Office of the State Comptroller.
Suspicions of possible Medicaid fraud, waste and abuse can be reported to the New York State OMIG Fraud Hotline at:
1-877-87FRAUD.
First in Nation
Oral Health Care During Pregnancy and Early Childhood
Practice Guidelines Issued
Return to Table of Contents
Oral health care during pregnancy is safe and, in most cases, very much in the best interest of both the mother and the baby. The practice guidelines, "Oral Health Care during Pregnancy and Early Childhood" stress the need for all health care professionals to recognize the importance of good oral health and to ensure that the need for dental care during pregnancy and early childhood is met.
Pregnancy is also an opportune time to educate women about preventing dental caries in young children, one of the most common childhood problems. Evidence suggests that most young children acquire caries-causing bacteria from mothers. Improving the oral health of expectant and new mothers and providing oral health counseling may reduce the transmission of such bacteria from mothers to children, thereby delaying the onset of caries.

ALL HEALTH CARE PROFESSIONALS should Advise women that:
- Dental care is safe and effective during pregnancy. Oral health care should be coordinated among prenatal and oral health care providers.
- First trimester diagnosis and treatment, including needed dental x-rays, can be undertaken safely to diagnose disease processes that need immediate treatment.
- Needed treatment can be provided throughout the remainder of the pregnancy; however, the time period between the 14th and 20th week is ideal.
- Elective treatment can be deferred until after delivery.
- Delay in necessary treatment could result in significant risk to the mother and indirectly to the fetus.
Advise women that the following actions will improve their health:
- Brush teeth twice daily with a fluoride toothpaste and floss daily.
- Limit foods containing sugar to mealtimes only.
- Choose water or low fat milk as a beverage. Avoid carbonated beverages during pregnancy.
- Choose fruit rather than fruit juice to meet the recommended daily fruit intake.
- Obtain necessary dental treatment before delivery.
Advise women that the following actions may reduce the risk of caries in children:
- Wipe an infant's teeth after feeding, especially along the gum line, with a soft cloth or soft bristled toothbrush.
- Supervise children's brushing and use a small (size of child's pinky nail) amount of toothpaste.
- Avoid putting the child to bed with a bottle or sippy cup containing anything other than water.
- Limit foods containing sugar to mealtimes only.
- Avoid saliva-sharing behaviors, such as sharing a spoon when tasting baby food, cleaning a dropped pacifier by mouth or wiping the baby's mouth with saliva.
- Avoid saliva-sharing behaviors between children via their toys, pacifiers etc.
- Visit an oral health professional with child between the six and 12 months of age.
The panel developed separate recommendations for prenatal, oral health and child health professionals. While specific treatments require attention to individual clinical situations, these recommendations are intended to bring about changes in the health care delivery system and to improve the overall standard of care.
Please visit the New York State Department of Health website at
http://nyhealth.gov/publications/0824.pdf
to download a copy of the practice guidelines.
If you have difficulty downloading the guidelines or if you do not have access to the internet, please contact us at: (518) 474-1961 or
oralhealth@health.state.ny.us

The Department of Health operates the Growing Up Healthy Hotline, which provides information about health care, nutrition and other health and human services.
The Hotline provides information and referral 24 hours a day, seven days a week in English, Spanish and other languages.
Anyone can contact the Hotline by calling (800) 522-5006 or through TTY access at (800) 655-1789.
All calls are confidential.
Sickle Cell Disease in New York's Medicaid Population
An Underutilization of the Drug Therapy Hydroxyurea
Return to Table of Contents
Sickle Cell Disease (SCD) has affected at least 2,844 New York Medicaid patients in 2005!
- Though it is a rare, genetically inherited disease, it greatly shortens patients' life span and decreases their quality of life.
- Patients with SCD suffer a variety of complications including painful crises, fever, infection, stroke and acute chest syndrome.
Hydroxyurea is currently the only drug that is approved by the Food and Drug Administration for the prevention of these crises.

Hydroxyurea has been studied in many clinical trials, the largest being the Multicenter Study of Hydroxyurea in Sickle Cell Anemia (MSH). This double-blind, placebo controlled, study examined 299 patients with sickle cell disease who were 18 years or older and had reported three or more crises within one year.
Hydroxyurea was found to:
- decrease the need for transfusions;
- the number of crises; and
- the incidence of acute chest syndrome.
The only adverse effect shown was bone marrow suppression, mostly mild neutropenia.
Of the Medicaid recipients with SCD, it appeared that 479 would meet the entry criteria of three or more crises for the MSH study. However, only 96 (20%) received hydroxyurea!
Thus, it appears that hydroxyurea is underutilized. This possible underutilization of hydroxyurea is not only costly to the Medicaid system, but costly to those patients that are not receiving drug therapy that may improve their quality of life.
One question asked is whether hydroxyurea use is related to the severity of the patient's illness.
The following graph examines hydroxyurea use in these 479 patients based on different measures of illness severity over the last five years. Illness severity was categorized as patients with:
- greater than two hospitalizations due to a crisis;
- those with any sickle cell crisis hospitalization; and
- all active recipients with SCD.
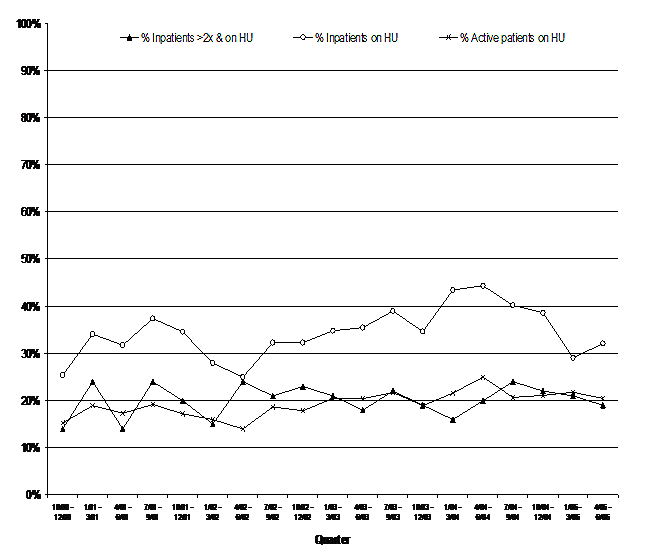
The prevalence of hydroxyurea use is similar in all active patients.
- Those patients requiring frequent hospitalizations showed around 20% use.
- Among those with one hospitalization, the prevalence seems to be slightly higher at about 35%.
In an effort to call attention to this apparent under treatment, the RetroDUR program will send letters to providers who care for recipients with SCD who are not receiving hydroxyurea.
The Drug Utilization Review (DUR) program welcomes your opinions and questions regarding this therapy.
For additional DUR information, please call 518-474-6866.
Juvenile Arthritis
Return to Table of Contents
Arthritis literally means joint inflammation. Juvenile arthritis refers to arthritis or a related condition that occurs by age 15. About 285,000 children in the United States under the age of 17 have a form of juvenile arthritis. The most common form of juvenile arthritis is juvenile rheumatoid arthritis, affecting up to 50,000 children.
Other common types of juvenile arthritis and related conditions include:
- juvenile spondyloarthropathies,
- juvenile psoriatic arthritis,
- juvenile dermatomyositis,
- juvenile vasculitis, and
- juvenile non-inflammatory disorders.
The major symptoms for all forms of arthritis in children are:

- pain,
- fatigue, and
- stiffness and swelling in the joints.
Arthritis can interfere with growth, causing children to be small for their age. The disease can attack one or more joints, including:
- fingers,
- wrists,
- neck,
- shoulders,
- elbows,
- hips,
- knees, and
- feet.
Arthritis may lead to permanent joint damage.
Although there is no cure for juvenile arthritis, there are many treatment options available.
Treatment is based on the type of arthritis a child has, as well as his or her symptoms. Every treatment program for juvenile arthritis focuses on controlling inflammation, relieving pain, preventing joint damage and maximizing functional abilities. Typically a treatment program for an individual with juvenile arthritis includes medication, eye and dental care, and proper nutrition.
In addition to treatment, community support services are available for children with juvenile arthritis and their families.
The American Juvenile Arthritis Organization (AJAO) is a Council of the Arthritis Foundation devoted to serving the specific needs of children, teens and young adults with childhood rheumatic diseases and their families. Its members are parents, family members, doctors, nurses, occupational and physical therapists, social workers, young adults, and anyone else with an interest in arthritis in young people. The four New York chapters of the Arthritis Foundation offer scholarships to attend AJAO conferences and/or arthritis camp or other recreational activities.
Additionally, the New York chapters of the Arthritis Foundation each have their own programs that focus on juvenile arthritis. The Northeastern New York Chapter sponsors a Juvenile Arthritis Club for Kids (JACKS). This group brings families of children suffering from a rheumatic disease together for local area activities.
The Upstate New York Chapter offers a one-time $500 college scholarship to high school seniors with arthritis or a related disease.
The New York Chapter has created the Kids Get Arthritis Too website as well as a semi-annual Family Day. The website provides information and resources specifically aimed at children and families affected by juvenile arthritis. The Family Day is a multi-tiered program for children with arthritis and their families with specific sessions targeting parents, children and teens. The Chapter also participates in National Juvenile Arthritis Awareness Week (JAAW) in March and has created special activities focusing on children in different ages and grades for faculty and students.
The Long Island Chapter provides parent-to-parent peer counseling and periodically conducts one-day symposiums for families that have a child with arthritis or a related disease. The symposiums are open to parents, teens and children. The Chapter also advocates for services for children with arthritis in the community on behalf of families.
Information for this article is from the Arthritis Foundation booklets "Arthritis in Children" and "When Your Student has Arthritis," and from the Arthritis Foundation website.
For more information on juvenile arthritis and programs in your area, please visit the Arthritis Foundation online at
http://www.arthritis.org
or call your local chapter of the Arthritis Foundation.
Dialysis Providers
Please copy and give to patients
WEATHERING THE STORM
Important Advice to Individuals Receiving Dialysis Treatment
Return to Table of Contents

The Commissioner of Health offers the following advice for individuals with End Stage Renal Disease (kidney disease) who cannot keep their scheduled dialysis appointments because of inclement weather, such as the October 2006 snowstorm that hit western New York and the June 2006 flood that hit the southern tier:
- Call your health care provider as soon as possible for guidance about what you should do.
- Be more careful than ever about following your dietary restrictions and limiting fluid intake.
- Consume no more than two cups of fluid every 24 hours, and do not eat fresh fruit or vegetables since many of these - especially bananas - are high in potassium.
- If you are running out of prescription medications and can't leave your home, ask a friend, relative or neighbor for help.
- If you must go to a shelter, tell the person in charge about your special needs.
- If you have to leave home, make sure your dialysis facility knows where to find you.
The Guide for People on Dialysis: Preparing for Emergencies is a booklet which provides a three-day emergency diet and other helpful information. It is available online at:
http://www.rsnhope.org/resources/PreparingforEmergenices.pdf.
Source: http://www.health.state.ny.us/press/releases/2006/2006-10-13_snowstorm_dialysis_advice.htm
Attention Practitioners
Please copy and give to vunerable patients
Older Adult Falls Can Be Prevented!
Return to Table of Contents
Older adults are frequently at risk for serious injuries as a result of a fall. The injuries are often the beginning of what then spirals into other health problems as a result of the lack of mobility.
How Big Is The Problem?

In New York State, fall related injuries are the leading cause of hospitalizations among persons 65 years and older.
- Over 800 older adults die each year as a result of a fall.
- Approximately 43,000 older adults are injured seriously enough to require hospitalization each year.
- Risk increases exponentially with age. New Yorkers aged 85 and older suffer the most severe consequences of a fall.
What Are The Most Serious Consequences Of A Fall ?
- Fractures, especially to the hip
- Traumatic brain injury
- Long-term disability
- Death
Who Is Most At Risk For A Fall?
Although a fall can happen to anyone, older adults, aged 65 and older are most at risk for the serious injuries that can threaten their mobility and their quality of life. Males are most at risk of dying from a fall with a diagnosis of a traumatic brain injury. Females are most at risk for sustaining a hip fracture.
Where Do Most Falls Occur?
Falls of course can happen anywhere, but the majority of them occur at home.
What Are The Most Common Risk Factors For A Fall?
- Medications that affect balance and cognitive abilities
- Loss of lower body strength
- History of falling in the past year
- Chronic diseases such as Parkinson's, arthritis and history of strokes
- Environment
How Can Falls Be Prevented?
There is usually more than one contributing factor when a fall occurs. Assessing various factors and making modifications will help reduce the risk of a fall related injury. Here are some tips to consider for preventing falls:
- Discuss all medications you are taking with your medical professional, including over the counter medications. Check for drug interactions, as well as possible side effects such as light headedness, loss of balance, or impaired vision.
- Discuss potential physical and mental limitations of any chronic disease or condition with a medical professional.
- Get routine eye exams to assess vision and wear glasses if you need them. When your prescription changes, go slowly until you adjust.
- Practice weight training to increase body strength. Use light weights to start, even lifting cans of corn can work! Also, Tai Chi and simply walking can help increase strength and promote good balance.
- Wear sturdy shoes. Avoid thick soft shoes and high heels. Wear a heel less than one inch for the best balance.
- Examine your home for potential problems that could lead to a fall. Check your home for the following:
- Be sure to have adequate lighting throughout the house. Do you have light switches at the top and bottom of all stairways? Are there nightlights to light your path to the bathroom? Keep a flashlight by the bed and within easy reach in case the power goes out.
- Are scatter rugs removed or secured to the floor with non-slip under mats?
- Bathtub and toilet grab bars assist you in moving around safely in the bathroom.
- Be sure all clutter is picked up so it does not become a tripping hazard.
- Although pets bring companionship, be careful when they are underfoot.
- Spills should be cleaned up immediately so the floor is not slippery.
- Use a step stool if you must reach to a higher shelf. Never use a chair! Keep items used frequently on lower shelves.
- Do all stairways have hand rails?
Fall injuries are preventable and the risk can be reduced by considering the possible contributing factors before it is too late.
For more information, please go to:

PROVIDER SERVICES
Return to Table of Contents
Missing Issues?
The Medicaid Update, now indexed by subject area, can be accessed online at the New York State Department of Health website:
http://www.nyhealth.gov/medicaid/program/update/main.htm
Hard copies can be obtained upon request by emailing: MedicaidUpdate@health.state.ny.us
Do You Suspect Fraud?
If you suspect that a recipient or a provider has engaged in fraudulent activities, please call the fraud hotline at: 1-877-87FRAUD. Your call will remain confidential.
As a Pharmacist, Where Can I Access the List of Medicaid Reimbursable Drugs?
The list of Medicaid reimbursable drugs is available at: http://www.eMedNY.org/info/formfile.html
Questions About an Article?
For your convenience each article contains a contact number for further information, questions or comments.
Do You Want Information On Patient Educational Tools and Medicaid's Disease Management Initiatives?
Contact Department staff at (518) 474-9219.
Questions About HIPAA?
Please contact CSC Provider Services at (800) 343-9000.
Patient Eligibility
Call the Touchtone Telephone Verification System (800) 997-1111, (800) 225-3040 or (800) 343-9000.
Address Change?
Questions should be directed to CSC at (800) 343-900, option 5.
Fee-for-service Provider Enrollment
A change of address form is available at:
http://www.emedny.org/info/ProviderEnrollment/Provider%20Maintenance%20Forms/6101-Address%20Change%20Form.pdf.
Rate-based/Institutional Provider Enrollment
A change of address form is available at:
http://www.emedny.org/info/ProviderEnrollment/Provider%20Maintenance%20Forms/6106-Rate%20Based%20Change%20of%20Address%20Form.pdf
Billing Question? Call Computer Sciences Corporation:
Provider Services (800) 343-9000.
Comments and Suggestions Regarding This Publication?
Please contact the editor, Timothy Perry-Coon at MedicaidUpdate@health.state.ny.us or via telephone at (518) 474-9219 with your concerns.
The Medicaid Update: Your Window Into The Medicaid Program
The State Department of Health welcomes your comments or suggestions regarding the Medicaid Update.
Please send suggestions to the editor, Timothy Perry-Coon:
NYS Department of Health
Office of Medicaid Management
Bureau of Program Guidance
99 Washington Ave., Suite 720
Albany, NY 12210
(e-mail MedicaidUpdate@health.state.ny.us)
The Medicaid Update, along with past issues of the Medicaid Update, can be accessed online at the New York State Department of Health web site:http://www.health_care/medicaid/program/update/main.htm