New York State Medicaid Update - June 2012 Volume 28 - Number 7
In this issue…
- Policy and Billing Guidance
- State Awards $10.6 Million to Train Physicians in Ambulatory Care Settings
- Provider Enrollment Required for Ordering, Referring and Attending Practitioners
- New York Medicaid Electronic Health Records Incentive Program Update
- Practitioners Serving Nursing Home Medicaid Members page
- Mandatory Compliance Program Certification Requirement
- Compliance Program Guidance for General Hospitals
- Pharmacy Updates
- All Providers
Policy and Billing Guidance
State Awards $10.6 Million to Train Physicians in Ambulatory Care Settings

Awards under Doctors Across New York Program will help to meet need for highly trained providers in community-based settings
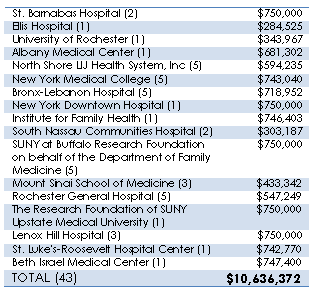
State Health Commissioner Nirav R. Shah, M.D., M.P.H., announced 17 awards totaling more than $10.6 million over three years for clinical training of medical residents and medical school students at freestanding ambulatory care sites.
The awards are being provided through the Doctors Across New York (DANY) program, which provides funding for the training and placement of physicians. The grants ar designed to help defray the costs of the clinical training provided at ambulatory care institutions, including diagnostic and treatment centers (D&TCs) and physician practices.
"As our health care system continues to evolve, we need to expand clinical training in ambulatory care settings where many patients receive care," Commissioner Shah said. "The Doctors Across New York program is an important resource to help train the next generation of physicians and these awards represent a critical and timely investment to ensure patients have access to high quality care.".
The award provided through the Ambulatory Care Training Program will facilitate clinical training for nearly 1,000 medical residents and students at 43 community based sites, preparing our future physicians for a changing health care system.
Under a Request for Application (RFA), applicants were eligible for awards ranging from $50,000 to $250,000 per year for three years. Institutions that provide physician training, including hospitals, medical schools, and at a federally qualified health center (FQHC), were eligible to apply for a grant provided they have an affiliation or agreement with a freestanding ambulatory care site.
For additional information on the DANY program, please visit: http://www.health.ny.gov/professionals/doctors/graduate_medical_education/doctors_across_ny/
Provider Enrollment Required for Ordering, Referring and Attending Practitioners
As reported in previous Medicaid Update articles; New Rules for Provider Screening and Enrollment, March 2011 and New Provider Enrollment and Screening Regulations, April 2011, Section 6401(a) of the Affordable Care Act (ACA) established new requirements surrounding provider enrollment. Specifically, 42 CFR, Section 455.410(b) requires providers to be enrolled in state Medicaid programs if they continue to order or refer services reimbursed by Fee-for-Service (FFS).
Requirements for Ordering/Referring/Attending
All FFS claims must include the NPI of the enrolled ordering, referring and/or attending provider, including:
- All FFS claims for ordered/referred services which are carved-out of the Medicaid Managed Care and Family Health Plus benefit packages;
- All FFS claims for services ordered/referred by out-of-state providers.
For further information, visit: http://www.medicaid.gov/Federal-Policy-Guidance/downloads/CIB-12-23-11.pdf.
Exemptions from Ordering/Referring/Attending
- Medicaid Managed Care and Family Health Plus encounters and services reimbursed by the plans;
- Services ordered/referred by residents and other practitioners that NYS Medicaid FFS does not authorize to enroll; these claims must include the NPI of the enrolled supervising physician.
As part of the Department's initiative to implement the ACA requirement, the following efforts will be rolled out in the coming months:
Provider Enrollment Process
Any practitioner who is eligible to enroll in NYS Medicaid FFS must be enrolled to continue to order or refer services that are paid by FFS. The Department is planning to offer a streamlined ordering/referring (non-FFS billing) practitioner enrollment process. Details will be announced in a future Medicaid Update.
Practitioners participating in Medicaid Managed Care plans who enroll in NYS Medicaid FFS may do so only for the purpose of ordering/referring for Medicaid FFS carved-out services and will not be required to accept Medicaid FFS members. Please refer to the Provider Enrollment materials at: https://www.emedny.org/info/ProviderEnrollment/index.aspx.
Verification of Provider Enrollment
System enhancements are underway to provide an online, real-time response for servicing providers to verify the enrollment status of ordering/referring/attending providers that will be announced in a future Medicaid Update and eMedNY LISTSERV® notifications. In the interim, to verify FFS Medicaid enrollment, servicing providers may:
- Contact the ordering/referring/attending provider;
- Check remittance advice (see below); or
- Contact CSC at (800) 343-9000 for further information.
Remittance Advice
A series of claim edits will be placed on a schedule of one week payment holds beginning in July 2012 to assist servicing providers with identifying non-enrolled ordering, referring and attending providers. The eMedNY edits/descriptions and HIPAA reason/status codes are:
- Edit 02042 - Referring MMIS Provider ID Can Not Be Derived (All Providers) CARC 208 - (NPI Denial Not Matched), RARC N286 (MISSING/INC/INV REF. PROVIDER PRIMARY IDENTIFIER), Status 562 (ENTITY'S NATIONAL PROVIDER IDENTIFIER (NPI))
- Edit 02043 - Attending MMIS Provider ID Can Not Be Derived (Institutional) CARC 208 (NPI DENIAL NOT MATCHED), RARC N253 (MISSING ATTENDING NPI), Status 562 (ENTITY'S NATIONAL PROVIDER IDENTIFIER (NPI))
- Edit 02071 - Ordering MMIS Provider ID Can Not Be Derived (Professional)CARC208 (NPI DENIAL NOT MATCHED), N265 (MISSING/INCOMP/INVALID ORDERING PROV PRIMARY ID), Status 562 (ENTITY'S NATIONAL PROVIDER IDENTIFIER (NPI))
Claims failing these edits will be released for processing after the one week payment hold. Remittance advice will indicate the edit failed and the pend status of these claims. The payment hold is a temporary measure: eventually, claims failing these edits will be denied. A provider Self Help Edit Search tool is also available at: https://www.emedny.org/HIPAA/5010/edit_error/index.aspx.
Please refer to your HIPAA 837D, 837I and 837P implementation guides for assistance on reporting of ordering and referring providers. Although a referring provider may be reported on the 837I, the attending provider must always be reported and is responsible for all ordered services.
Providers will be informed in advance of the specific payment hold rollout schedule by Provider Type through the eMedNY LISTSERV® system. To sign-up for the listserv (Provider Type and General), please visit: https://www.emedny.org/listserv/emedny_email_alert_system.aspx.
Prescribing Providers
The ordering/referring requirement extends to providers who prescribe prescription drugs for Medicaid FFS members. Future Medicaid Update articles will detail the implementation for pharmacy claims.
New York Medicaid Electronic Health Records Incentive Program Update
The New York State Department of Health (NYSDOH) is pleased to announce that as of June 15, 2012, the New York Medicaid Electronic Health Records (EHR) Incentive program has now paid over $138 million in federal incentive funds to nearly 1,350 New York State hospitals and healthcare practitioners.
NYSDOH continues to review applications for Payment Year 2011 incentive payments that were submitted prior to the April 29, 2012 deadline, and applications for Payment Year 2012 are currently being accepted from providers who are new to the incentive program. Applications for providers' second incentive payment (including Meaningful Use Attestation) will be accepted beginning in the fourth quarter of calendar year 2012.
If you have not yet registered for the New York Medicaid EHR Incentive program, we encourage you to visit the eMedNY.org website https://www.emedny.org/meipass/ or attend one of the informationalwebinars hosted by NYSDOH throughout the month of July.
| Tuesday, July 3 | 3:00-4:00PM | Eligible Professional Registration & Attestation |
| Thursday, July 5 | 12:00-1:00PM | MEIPASS Prerequisites |
| Tuesday, July 10 | 10:00-11:00AM | EP Support Documentation |
| Wednesday, July 11 | 3:00-4:00PM | Meaningful Use, Stage 1 (Eligible Professionals) |
| Wednesday, July 18 | 12:00-1:00PM | MEIPASS Prerequisites |
| Tuesday, July 24 | 10:00-11:00AM | Eligible Professional Registration & Attestation |
| Thursday, July 26 | 12:00-1:00PM | Meaningful Use, Stage 1 (Eligible Hospitals) |
| Tuesday, July 31 | 3:00-4:00PM | Meaningful Use, Stage 1 (Eligible Professionals) |
The webinar schedule is subject to change based on interest levels. To see the complete schedule or to register for one of the webinars, please view the webinar schedules posted on the eMedNY.org website at:
Current Month: https://www.emedny.org/meipass/webinar/Webinar.pdf
Next Month: https://www.emedny.org/meipass/webinar/NextMonth.pdf
Practitioners Serving Nursing Home Medicaid Members
When a medical service is provided to a Medicaid member residing in a nursing home and the practitioner bills Medicaid Fee-for-Service (FFS), it is the practitioner's responsibility to record and maintain all medical documentation supporting the medical claims billed to Medicaid.
Please see Title 18 of the Social Services law, Section 504.3 - Duties of the provider. By enrolling, the provider agrees:
(a) to prepare and to maintain contemporaneous records demonstrating its right to receive payment under the medical assistance program and to keep for a period of six years from the date the care, services or supplies were furnished, all records necessary to disclose the nature and extent of services furnished and all information regarding claims for payment submitted by, or on behalf of, the provider and to furnish such records and information, upon request, to the department, the Secretary of the United States Department of Health and Human Services, the Deputy Attorney General for Medicaid Fraud Control and the New York State Department of Health.
You may also refer to the "Record-Keeping Requirements" in the provider manual under "Information for All Providers - General Policy."
Questions? Please contact the Division of Program Development and Management at (518) 473-2160.
THIS IS A REMINDER FROM THE NEW YORK STATE OFFICE OF THE MEDICAID INSPECTOR GENERAL (OMIG) FOR ALL MEDICAID PROVIDERS WHO ARE SUBJECT TO THE MANDATORY COMPLIANCE PROGRAM REQUIREMENT.Mandatory Compliance Program Certification Requirement
RECOMMENDATION FOR SELF ASSESSMENT
The New York State Office of the Medicaid Inspector General (OMIG) highly recommends that all Medicaid providers conduct an annual self assessment of their compliance programs. A self assessment will maximize a provider's opportunity to make improvements, corrections or refinements to their compliance programs prior to the December 2012 certification period.
The following paragraphs identify those Medicaid providers that are required to have compliance programs. If a Medicaid provider is required to have a compliance program, the Medicaid provider is also required to certify on OMIG's website, www.omig.ny.gov, that its compliance program meets the requirements of the applicable law and regulations. The certification must occur in December of each year.
New York State Social Services Law(SSL) §363-d and Part 521, of Title 18 of the New York State Codes, Rules and Regulations (NYCRR), both entitled Provider Compliance Programs, has been actively enforced by OMIG since 2009. This regulation requires all Medicaid providers who fall under the following categories to certify in December of each year that they have adopted, implemented and maintain an effective compliance program.
- Persons subject to the provisions of articles 28 or 36 of the New York State Public Health Law;
- Persons subject to the provisions of Articles 16 or 31 of the New York State Mental Hygiene Law;
- Other persons, providers or affiliates who provide care, services or supplies under the Medicaid program, or persons who submit claims for care, services or supplies for or on behalf of another person or provider for which the Medicaid program is or should be reasonably expected by a provider to be a substantial portion of their business operations.
Under 18 NYCRR § 521.2 (b), "substantial portion" of business operations means any of the following:
- When a person, provider or affiliate claims or orders, or has claimed or has ordered, or should be reasonably expected to claim or order at least $500,000 in any consecutive 12-month period from the medical assistance program;
- When a person, provider or affiliate receives or has received, or should be reasonably expected to receive at least $500,000 in any consecutive 12-month period directly or indirectly from the medical assistance program; or
- When a person, provider or affiliate who submits or has submitted claims for care, services, or supplies to the medical assistance program on behalf of another person or persons in the aggregate of at least $500,000 in any consecutive 12-month period.
Each compliance program must contain the eight elements required under SSL § 363-d and 18 NYCRR §521.3 (c). Upon applying for enrollment in the medical assistance program, and during the month of December each year thereafter, 18 NYCRR 521.3 (b) requires providers to certify to the department and OMIG that a compliance program meeting the requirements of the regulation is in place.
The regulation, certification form, and FAQ's are available on the OMIG website at: http://www.omig.ny.gov/data/content/view/159/303.
Additionally, New York State Medicaid providers are encouraged to review OMIG"s website and review the Compliance Alerts that are published under the Compliance Tab on the OMIG's home page.
The following published Compliance Alerts may be helpful to Medicaid providers as they consider their obligations under this requirement:
Compliance Alert 2010-02: Effectiveness of Medicaid Provider's Compliance Program
Compliance Alert 2011-01: Annual Certification 2010
Compliance Alert 2011-05: Compliance Program Requirement for New Medicaid Providers
Lastly, OMIG will be updating New York Medicaid's Form for Provider Certification of Effective Compliance Programs during 2012 for use during December 2012. When the new form becomes available, it will be announced in the Medicaid Update and also on OMIG's website. The current form, and the form for 2012, allows the Medicaid provider the opportunity to inform OMIG that its compliance program does not meet the effectiveness requirements.
It is the Medicaid provider's responsibility to determine if:
- a. it has a compliance plan that meets the requirements of under SSL § 363-d and 18 NYCRR § 521.3 (c) and;
- b. its compliance program is effective.
How the Medicaid provider assesses its compliance program will determine whether the Medicaid provider can certify that its compliance program is effective or ascertain that its program is not effective.
New York Medicaid providers are urged to sign-up for e-mail notices from OMIG by subscribing to OMIG's listserv. Anyone may become a subscriber by signing up on OMIG's home page. The listserv is a great way to keep informed of the introduction of new compliance tools and information on compliance. As additional compliance alerts are published by OMIG, those on OMIG's listserv will receive notices of their publication.
Questions? Please contact the OMIG Bureau of Compliance at (518) 408-0401 or via e-mail at: compliance@omig.ny.gov
Compliance Program Guidance for General Hospitals
PUBLICATION ANNOUNCEMENTEffective, May 11, 2012, the New York State Office of the Medicaid Inspector General (OMIG) published the Compliance Program Guidance for General Hospitals.
The Guidance is available on OMIG's website at: http://www.omig.ny.gov/data/images/stories/compliance/compliance_program_guidance-general_hospitals.pdf.
Although the Guidance applies specifically to general hospitals, many other Medicaid providers required to implement and maintain an effective compliance program under New York State Social Services Law (SSL) §363-d and Title 18 of the New York State Codes, Rules and Regulations (NYCRR), Part 521 may find the Guidance to be helpful as they implement and maintain their compliance programs. The eight elements that are required of all Medicaid providers' compliance programs are the same, but how hospitals operate, provide care and are managed may be different from other Medicaid provider types.
The Compliance Program Guidance for General Hospitals is a guide and does not, on its own, carry the force of law or regulation. It was prepared to help general hospitals implement and maintain effective compliance programs required under SSL§ 363-d and 18 NYCRR Part 521.
New York's Medicaid providers are urged to sign-up for e-mail notices from OMIG by subscribing to OMIG's listserv. Anyone can become a subscriber by signing up on OMIG's home page. The listserv is a great way to keep informed of the introduction of new compliance tools and information on compliance.
Questions? Please contact the OMIG Bureau of Compliance at (518) 408-0401 or via e-mail at: compliance@omig.ny.gov
NYSMPEP Drug Information Response Center Addresses Use of Inhaled Corticosteroids in Pediatric Asthma Patients

The New York State Medicaid Prescriber Education Program (NYSMPEP) is a collaboration between the New York State Department of Health (NYSDOH) and the State University of New York (SUNY), as approved by state legislation. This program was designed to provide prescribers with an evidence-based, non-commercial source of the latest objective information about pharmaceuticals. In conjunction, the Drug Information Response Center (DIRC) was developed to fulfill the mission of assisting clinicians in the delivery of health care to their Medicaid members by providing timely, evidence-based information on pharmacotherapy to prescribers and serving as a resource for NYSMPEP academic educators in their outreach to prescribers. A recent review was prepared by the DIRC in response to a request for information on the use of inhaled corticosteroids in pediatric asthma patients.
Inhaled corticosteroids (ICS) play an integral part to the management of asthma in pediatric patients. In 2007, the National Heart Lung and Blood Institute (NHLBI) issued guidelines for the diagnosis and management of asthma in which they assert that initiation of low-dose ICS as a long-term control therapy may significantly reduce overall symptom burden and frequency of asthma exacerbations in pediatric patients.1 Recommendations are categorized by patient age (0 to 4 years, 5 to 11 years, and =12 years); however, the NHLBI states that ICS are the preferred therapy for initial long-term control in children of all ages. These drugs have been shown to consistently control and prevent asthma symptoms, reverse airflow obstruction, improve quality of life, and decrease the number and severity of asthma exacerbations.2 Additionally, ICS are deemed to be generally safe, especially when given at low doses, even for extended periods.1 Of note, while ICS are effective in controlling symptoms, their administration will not alter the underlying disease progression or severity, as demonstrated by worsening of symptoms and airway responsiveness when treatment is withdrawn.
Several ICS are commercially available. In their 2007 guidelines, the NHLBI outlines then-available ICS with estimated comparative daily dosages in children less than 11 years of age.1 The NHLBI cautions that the preparations are not absolutely interchangeable on a mcg or per puff basis. Also, different delivery devices may offer greater or lesser amounts of drug to the airways, affecting the dose.
Based on the recommendations of the NHLBI, it appears that while the ICS differ in potency and dosage form, they may not differ in efficacy.1 The differences in potency may be overcome with dose conversion or comparative dosing. Adherence-related issues should be noted, however, as these may factor into the relative benefits of ICS therapy. From a search of the literature, several comparative clinical trials and clinical reviews were identified that discuss potential clinical differences among available ICS. A detailed discussion of the relevant literature is available on the NYSMPEP website at: http://nypep.nysdoh.suny.edu/dirc.
Medicaid Pharmacy Prior Authorization Program Update
On April 19, 2012, the New York State Medicaid Pharmacy & Therapeutics Committee (P&TC) recommended changes to the Medicaid pharmacy prior authorization programs. The Commissioner of Health has reviewed the recommendations of the committee and has approved changes to the Preferred Drug Program (PDP) within the Fee-For-Service (FFS) Pharmacy Program. Effective July 12, 2012, prior authorization (PA) requirements will change for some drugs in the following PDP classes:
- Antipsychotics -Second Generation*
- Central Nervous System (CNS) Stimulants
- Direct Renin Inhibitors
- HMG-CoA Reductase Inhibitors (Statins)
- Inhaled Anticholinergic/COPD Agents
- Inhaled Corticosteroid/Beta2-Adrenergic Agents (Long-Acting) Combinations
- Inhaled Short Acting Beta2 Adrenergic Agents
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) - Prescription
- Proton Pump Inhibitors (PPIs)
- Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs)
*Commissioner of Health approval of this class is pending further review. The final determination will be communicated at a future date.
The PDP has also expanded to include an additional drug class. Non-preferred drugs in the following drug class will require PA:
- https://www.emedny.org/info/formfile.aspx
- Hepatitis C Agents - Ribavirins
Please note that PA requirements are no longer dependent on the date a prescription is written. New prescriptions and refills on existing prescriptions require PA even if the prescription was written before the date the drug was determined to require PA. Note: Patients stabilized on atypical anti-psychotics will continue to obtain their medications without prior authorization. The Preferred Drug List (PDL) and additional information, such as updated PA forms and clinical criteria for the PDP and Clinical Drug Review Program (CDRP) are available at the following websites:
http://www.nyhealth.gov OR http://newyork.fhsc.com OR http://www.eMedNY.org
To obtain a PA, please contact the prior authorization clinical call center at (877) 309-9493. The clinical call center is available 24 hours per day, 7 days per week with pharmacy technicians and pharmacists who will work with you, or your agent, to quickly obtain PA. If you have any questions, wish to obtain additional information regarding the PDP or would like to receive the PDL, please contact the clinical call center at (877) 309-9493. Thank you for your continued support of our efforts to maintain a quality pharmacy program for Medicaid fee-for-service members.
Temporary Medicaid Authorizations
When an applicant is determined eligible for Medicaid and has an immediate need for a prescription drug the local social service district (LDSS) may issue a temporary paper Medicaid authorization (DSS-2831A) to make certain that the applicant receives needed services. When this occurs please refer to the following information.
Providers should ensure that temporary paper authorizations presented at the pharmacy are filled out completely. Providers must also make a copy of all temporary Medicaid authorizations for their records.
Claims for drugs dispensed to members with temporary paper Medicaid authorizations cannot be submitted through the online Pro-DUR/ECCA program since eligibility is not yet on file. However, it is important to note that temporary paper Medicaid authorizations are a guarantee of coverage for the time period indicated on the card. Once the local district has updated eligibility in the system, the provider will be able to bill Medicaid as long as the dispensed medication was not identified as having prior authorization requirements.
Currently, temporary paper Medicaid authorizations cannot be used for medications that require a prior authorization. Drugs that require a prior authorization are identified on the eMedNY formulary file with a PA code = G and can be found at: https://www.emedny.org/info/formfile.aspx. Pharmacy providers are also encouraged to check the Preferred Drug List (PDL) prior to dispensing to members with temporary authorizations. If the online claim adjudication results in a denial for member ineligibility, providers may contact the NYSDOH Local District Support Unit at:
- Upstate members: (518) 474-8887
- New York City members: (212) 417-4500.
If the online claim adjudication results in a denial because the drug required prior authorization, providers may contact the NYSDOH Bureau of Program Implementation and Administration at (518) 486-3209.
E-Prescribing Incentive Reminder
The New York Medicaid e-prescribing incentive program applies only to non-facsimile electronic transmissions when compliant with Medicare Part D data standards. E-Prescribing incentive checks are being returned by prescribers who claim they do not e-prescribe.
PLEASE NOTE: Electronic Prescription Definition:New York State Pharmacy Regulations http://www.op.nysed.gov/prof/pharm/part63.htm recognizes two distinct types of electronically-transmitted prescriptions:
- a prescription transmitted electronically by facsimile;
- a prescription transmitted electronically by means other than facsimile; such non-facsimile prescriptions are required by regulation to be electronically encrypted, meaning protected to prevent access, alteration or use by any unauthorized person.
The New York State Medicaid program accepts both types of electronically-transmitted prescriptions for standard claim reimbursement. However, pharmacies must verify a prescription is compliant with Medicare Part D data standards and requirements and NYS Pharmacy Regulations before submitting for the e-prescribing incentive.
Claims for prescriptions transmitted electronically by means other than facsimile and not Medicare Part D compliant are recognized by New York State Medicaid for claim reimbursement purposes, but do not qualify for the e-prescribing incentive reimbursement.
The e-prescription must originate from the prescriber's computer system (an electronic health record, electronic medical record, or stand-alone e-prescribing software) and must be transmitted to the retail pharmacy's computer system.
Additional information is available online at:
http://www.health.ny.gov/health_care/medicaid/program/update/2009/2009-11spec.htm.
All Providers
eMedNY Provider Support
eMedNY offers a variety of support options for providers who may be experiencing problems or need assistance with transaction submissions or resolving outstanding billing issues. Support is available for the New York State Medicaid program including but not limited to these major areas:
- Provider Enrollment
- Billing
- Eligibility Verification
- Prior Approval Requests
- The Electronic Provider Assisted Claim Entry System (ePACES)
- Electronic Responses/Remittance and Claim Denial Interpretation
The eMedNY Call Center may be reached by telephone at (800) 343-9000.
For provider inquiries pertaining to non-pharmacy billing or claims, or provider enrollment:
Monday through Friday: 7:30 a.m. - 6:00 p.m., Eastern Time (excluding holidays)
For provider inquiries pertaining to eligibility, service authorizations, DVS, and pharmacy claims:
Monday through Friday: 7:00 a.m. - 10:00 p.m., Eastern Time (excluding holidays) Weekends and Holidays: 8:30 a.m. - 5:30 p.m., Eastern Time
Additionally, the Call Center can refer a helpdesk ticket for technical inquiries about electronic file rejections and electronic HIPAA formatting of files to Computer Sciences Corporation (CSC).
Regional Representatives are available to assist providers with individual requests for training.
Registration is available at www.emedny.org, click on Training.
Requests for individual training can be made through the Call Center number above or via e-mail to: eMedNYProviderRelations@csc.com.
The eMedNY website offers information on all aspects of the eMedNY claims processing system including, provider self-help documents, provider manuals and links to other websites.
We welcome your inquiries and appreciate your continued participation in the New York State Medicaid program.
eMedNY Training Schedule and Registration
- Do you have billing questions?
- Are you new to Medicaid billing?
- Would you like to learn more about ePACES?
If you answered YES to any of these questions, consider registering for a Medicaid seminar or webinar. Computer Sciences Corporation (CSC) offers various educational opportunities to providers and their staff. Training sessions are available to new providers and specific provider types. These include information for claim submission, Medicaid Eligibility Verification, and the eMedNY website.Many of the sessions planned for the upcoming months offer detailed instruction about Medicaid's web-based billing and transaction program ePACES.
You may also register for a webinar in which training would be conducted online and you can join the meeting from your computer and telephone. After registration is completed, just log in at the announced time. No travel time or expenses are involved.
ePACES is the Electronic Provider Assisted Claim Entry System which allows enrolled providers to submit the following type of transactions:
- Claims
- Eligibility Verifications
- Claim Status Requests
- Prior Approval/DVS Requests
Physician, Nurse Practitioner, DME and Private Duty Nursing claims may even be submitted in "REAL-TIME" via ePACES. Real-time means that the claim is processed within seconds and professional providers can get the status of a real-time claim, including the paid amount without waiting for the remittance advice.
Fast and easy seminar/webinar registration, locations, and dates are available on the eMedNY website at: http://www.emedny.org/training/index.aspx.
CSC Regional Representatives look forward to having you join them at upcoming meetings!If you are unable to access the Internet to register or have questions about registration, please contact the eMedNY Call Center at (800) 343-9000.
Provider Directory
- Office of the Medicaid Inspector General: For general inquiries or provider self-disclosures, please call (518) 473-3782. For suspected fraud complaints/allegations, call 1-877-87FRAUD (1-877-873-7283), or visit www.omig.ny.gov.
- Provider Manuals/Companion Guides, Enrollment Information/Forms/Training Schedules: Please visit the eMedNY website at: www.emedny.org.
- Providers wishing to hear the current week's check/EFT amounts: Please call (866) 307-5549 (available Thursday PM for one week for the current week's amount)
- Do you have questions about billing and performing MEVS transactions? Please call the eMedNY Call Center at (800) 343-9000.
- Provider Training: To sign up for a provider seminar in your area, please enroll online at: http://www.emedny.org/training/index.aspx. For individual training requests, call (800) 343-9000 or e-mail: emednyproviderrelations@csc.com.
- Enrollee Eligibility: Call the Touchtone Telephone Verification System at (800) 997-1111.
- Address Change? Address changes should be directed to the eMedNY Call Center at (800) 343-9000.
- Fee-for-Service Providers: A change of address form is available at: https://www.emedny.org/info/ProviderEnrollment/allforms.aspx.
- Rate-Based/Institutional Providers: A change of address form is available at: https://www.emedny.org/info/ProviderEnrollment/allforms.aspx.
- Does your enrollment file need to be updated because you've experienced a change in ownership? Rate Base/Institutional and Fee-for-Service providers, please call (518) 474-3575, Option 4
- Do you have comments and/or suggestions regarding this publication?
- Please contact Kelli Kudlack at: medicaidupdate@health.state.ny.us.