State Systemic Improvement Plan (SSIP)
What is the State Systemic Improvement Plan (SSIP)?
The State Systemic Improvement Plan or SSIP, is required by the U.S. Department of Education, Office of Special Education Programs (OSEP). The New York State Department of Health Bureau of Early Intervention (Department) is required to report SSIP progress annually to OSEP. Each state's Early Intervention Program (EIP) was charged with developing an SSIP that focused on either improving child outcomes or improving family outcomes. The New York State (NYS) Early Intervention Coordinating Council (EICC), which is the Bureau of Early Intervention's (BEI) governor-appointed advisory council, unanimously supported the selection of family outcomes for the NYS SSIP. The SSIP project undertaken by the NYS EIP is also known as Improving Family Centeredness Together (IFaCT).
SSIP Project Phases
Three phases from 2014 to 2020:
- First phase: data analysis and select measure (completed April 1, 2015)
- Presented Outcome Data and Infrastructure Analysis to the EICC in March 2015
- Second phase: plan to align infrastructure and evaluate (completed April 1, 2016)
- Third phase: implementation (report on progress each year)
- Report submitted to OSEP on April 1, 2020
You can find the submitted reports for all phases as part of our submitted Annual Performance Reports here: https://www.health.ny.gov/statistics/community/infants_children/early_intervention/
What is IFaCT?
The Department is working with each county and borough to improve the EIP experience for families and children. Over the course of three years, the Department has partnered with three New York University Centers for Excellence in Developmental Disabilities (UCEDDs) to use an evidenced-based learning collaborative model to improve family outcomes by ensuring the program and the services provided are family-centered. UCEDD staff, municipal administrators, EIP providers, and parents have shared experiences, plan strategies, and develop innovative ideas to further support children and families within the EIP. Together, we aim to improve the quality of EI services, increase parent satisfaction, and improve health and developmental outcomes for the children we serve.
Why did NYS and the EICC choose to focus on family outcomes?
The Department completed an analysis of both family and child outcomes data in the EIP. In response to a State survey sent to families from 2008-2013, only 65% of families reported receiving enough help on family outcomes. For this reason, the focus of the SSIP is on family outcomes, as increased family-centeredness can lead to improved child outcomes. For more information about the family outcomes survey, please see the BEI Family Outcomes Page.
What are family outcomes?
Family outcomes are defined as a benefit experienced by families as a result of services received. By "families" we mean "the people who think of themselves as part of the family, whether related by blood or marriage or not, and who support and care for each other on a regular basis" (Poston, Turnbull, Park, Mannan, Marquis, & Wang, 2003).
How will the State improve family outcomes?
The State will improve family outcomes by improving the quality of the NYS EIP by ensuring the Program and the services provided are family-centered. The main objectives of the SSIP, which are supported by the evidence-based literature on family-centeredness, include:
- Enhancing parents' knowledge, skills, and access to resources
- Ensuring providers collaborate with parents
To promote family-centeredness, the State has identified the family-directed assessment, which is completed as part of multidisciplinary evaluations, as a tool to be used to improve family outcomes. The Department developed the following form, to assist providers with completing the family-directed assessment with families:
How does the Department measure improvements in family outcomes during the SSIP?
The SiMR is to increase the percentage of positive responses from families on the “New York Impact of Early Intervention services on Your Family” Scale (NYIFS). New York State (NYS) has identified improving family outcomes as the focus of the State Systemic Improvement Plan (SSIP), Improving Family Centeredness Together (IFaCT). The State will improve family outcomes by ensuring the Program and the services provided, are family-centered.
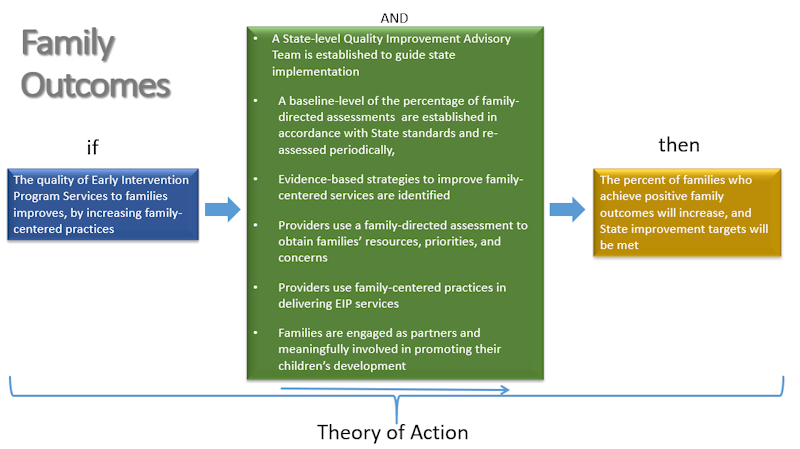
Our Updated Theory of Action (see Figure 1.) proposes that greater family-directed assessment completion will result in greater family outcomes scores. To collect data on the SiMR, the NYS Department of Health (Department) will continue to annually survey families using the Family Outcome Survey (FOS), developed by the National Center for Special Education Accountability Monitoring (NCSEAM). The survey results will be used to evaluate the Theory of Action and progress toward the SiMR and the goal of improving positive family outcomes.
Figure 1. Theory of Action
What evidence-based improvement strategy was used to implement SSIP?
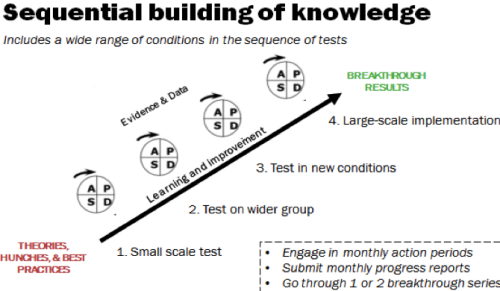
The Department has selected a well-tested and proven improvement strategy to work with local EIPs and service providers to increase the percent of families receiving family-centered services: the breakthrough series approach developed by the Institute for Healthcare Improvement (IHI). IHI uses the science of improvement to assist health care organizations in making "breakthrough improvements" in the quality and value of health care services. Improvement science is an applied, multidisciplinary approach that emphasizes innovation, rapid-cycle testing in the field, and the concept of "spread" to generate learning about what changes, in what settings and contexts, to yield improvement in the quality of service delivery (http://www.ihi.org/about/Pages/ScienceofImprovement.aspx ). The science of improvement draws on clinical science, systems theory, statistics, and other fields in its approach to working with health care organizations to improve the quality of care.
The "breakthrough series" is an evidence-based approach to working with organizations and professionals to achieve improvements in the quality of service delivery through "Learning Collaboratives." A Learning Collaborative is a systematic, time-limited approach to quality improvement in which multiple organizations come together with faculty to learn about and create improved processes in a specific topic area. The expectation is that the teams share expertise and data with each other; thus, "everyone learns, everyone teaches." Teams engaged in healthcare "Learning Collaboratives" have achieved dramatic results, including reducing waiting times by 50% percent, reducing worker absenteeism by 25%, reducing intensive care unit costs by 25%, and reducing hospitalizations for patients with congestive heart failure by 50%. (See The Breakthrough Series: IHI's Collaborative Model for Achieving Breakthrough Improvement. IHI Innovation Series white paper. Boston: Institute for Healthcare Improvement; 2003; available on www.IHI.org).
Figure 2. The Breakthrough Series Framework
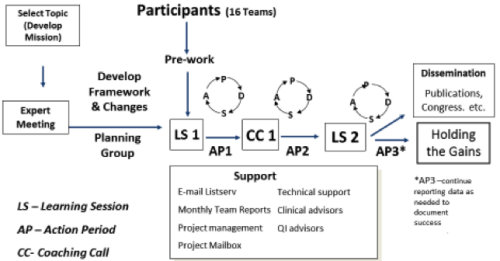
Ref: The Breakthrough Series: IHI's Collaborative Model for Achieving Breakthrough Improvement. IHI Innovation Series white paper. Boston: Institute for Healthcare Improvement; 2003; available on www.IHI.org
Who guided the State's implementation of SSIP?
Establish a State-level Quality Improvement Advisory Team to guide the state implementation
The SSIP advisory group was established during Year 1 of SSIP. The SSIP Advisory Group includes Department staff, representatives of the EICC and Early Childhood Advisory Council (ECAC), parent representatives, state agency partners, NYS EIP local program staff (Early Intervention Official (EIO) or Early Intervention Manager (EIM)) and service provider representatives. The SSIP Advisory Group is responsible for advising and assisting the Department in all aspects of implementation of the SSIP Family-Centered Practices Learning Collaboratives. The members are informed of Department proposed plans for SSIP implementation through webinars and other communications.
Examples of how the Advisory Group was involved in the implementation of the SSIP:
- Aided the Department in creating brochures for the recruitment of participants in the Learning Collaboratives for both cohorts. Based on their feedback, the brochures were individualized for the four different types of participants (i.e., a parent brochure, a provider brochure, a service coordinator brochure, and an EIO/EIM/EIOD brochure). The Advisory Group provided the content for the materials and provided feedback on the design of the brochures. The brochures for parents were also translated into Spanish and Chinese.
- Advised the Department to ask that parents and providers who wished to participate in SSIP to complete an application. The Advisory Group provided feedback on the questions that should be included and the formatting of the applications.
- Advised the Department to create a more family-friendly name for SSIP. After multiple brainstorming sessions and discussions with other Department staff and experts, the Advisory Group agreed to the name, Improving Family Centeredness Together (IFaCT).
Who did the Department partner with to implement the SSIP?
Centers of Excellence to? Implement the SSIP
Three Universities of Excellence in Developmental Disabilities (UCEDDs) were chosen to implement SSIP with oversight from the Department based on their experience and work in the field of children with disabilities, as well as their locations in the state:
- The Rose F. Kennedy University Center for Excellence in Developmental Disabilities (RFK)
- The Westchester Institute for Human Development (WIHD)
- The Strong Center for Developmental Disabilities (SCDD) at the University of Rochester Medical Center.
The Department, in collaboration with the three UCEDDs, successfully implemented the breakthrough series approach with teams of early intervention stakeholders. Due to the size of the State and the complexity of this project, the State was split into two cohorts. These cohorts were formed based on regions of New York State and proximity to one of three UCEDDs. Each county in NYS had at least one team. There were 34 teams in Cohort 1 and 33 teams in Cohort 2. The first cohort in each region started in January and February 2018, and the second cohort started in October and December 2018.
Figure 3. Regions by University Centers of Excellence in Developmental Disabilities (UCEDDs)
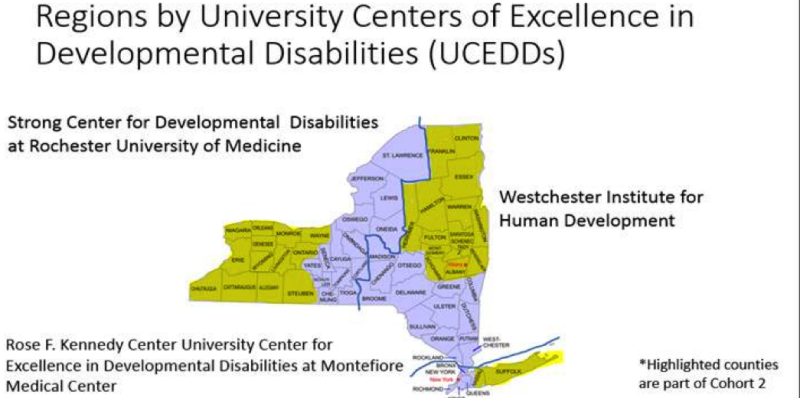
| UCEDD | Regions supported by UCEDD | Cohort 1 Counties | Cohort 1 Teams (n) | Cohort 2 Counties | Cohort 2 Teams (n) |
|---|---|---|---|---|---|
| RFK | New York City and Long Island | Bronx, Kings, New York, Queens, Richmond | 6 | Bronx, Kings, Nassau, New York, Queens, Richmond, Suffolk | 7 |
| SCDD | Central and Western | Cayuga, Chemung, Cortland, Jefferson, Lewis, Oneida, Onondaga, Oswego, Schuyler, Seneca, St. Lawrence, Tioga, Tompkins, Yates | 14 | Allegany, Cattaraugus, Chautauqua, Erie, Genesee, Livingston, Monroe, Niagara, Ontario, Orleans, Steuben, Wayne, Wyoming | 13 |
| WIHD | Hudson Valley, Capital Region, and up to Canadian border | Broome, Chenango, Columbia, Delaware, Dutchess, Greene, Madison, Orange, Otsego, Putnam, Rockland, Sullivan, Ulster, Westchester | 14 | Albany, Clinton, Essex, Franklin, Fulton, Hamilton, Herkimer, Montgomery, Rensselaer, Saratoga, Schenectady, Schoharie, Warren, Washington | 13 |
Learning Collaborative Process
Overview
The Department is working with each county and borough to improve the EIP experience for families and children. Over the course of three years, the NYS DOH has partnered with three UCEDDs to use an evidenced-based learning collaborative model to improve family outcomes by ensuring the program and the services provided are family-centered. UCEDD staff, municipal administrators, EIP providers, and parents will share experiences, plan strategies, and develop innovative ideas to further support children and families within the EIP. Together, we aim to improve the quality of EI services, increase parent satisfaction, and improve health and developmental outcomes for the young children we serve.
Each Learning Collaborative lasted approximately 12 months. Each of the three NYS UCEDDs held a regionally based collaborative each year for two years (6 Learning Collaboratives). The Learning Collaborative in Year 1 is called Cohort 1. The Learning Collaborative in Year 2 is called Cohort 2. Within each collaborative, there were county-based teams comprised of EI stakeholders including parents, EI practitioners, and municipal EI staff. Over two years, every county in NYS had one team except for NYC and Nassau and Suffolk County, which had multiple teams.
Over the course of a year, teams collected data to study the impact their improvements made, and then act on it. If the change improved family outcomes the team would increase its use, and if the change does not help, the team would reevaluate and adjust their plan accordingly.
Once the local projects were completed, the UCEDDs analyzed the data and used the information to develop web-based training and resource materials on best practices for family centeredness.
The NYS DOH integrated some of these best practices into State-sponsored professional development and training to reinforce family centeredness, and update policies and procedures to support family-centered practices in the EIP.
Cohort 1 and Cohort 2 Learning Collaborative Breakdown
In total there were 67 teams formed across NYS. For the first cohort, WIHD and SCDD both had 14 teams for each county involved, while RFK had six teams, across the five boroughs. For the second cohort, WIHD had 13 teams, SCDD had 13 teams, and RFK had seven teams across the five boroughs and Long Island. During Cohort 2, three of RFK's eight teams were focus non-English speaking communities – Spanish and Mandarin. There was one Spanish-speaking team and one Mandarin- speaking team.
| Cohort 1 | RFK | WIHD | SCDD |
|---|---|---|---|
| Region | New York City | Hudson/Capital/NE | Central/Western |
| Number of counties | 5 | 13 | 14 |
| Number of teams | 8 | 13 | 14 |
| Total number of participants | 52 | 75 | 68 |
| EIO/D/Ms | 12 | 24 | 16 |
| Service providers/coordinators | 32 | 34 | 32 |
| Parents | 8 | 17 | 20 |
| Cohort 2 | RFK | WIHD | SCDD |
|---|---|---|---|
| Region | New York City/ Long Island | Hudson/Capital/NE | Central/Western |
| Number of counties | 7 | 13 | 13 |
| Number of teams | 8 | 13 | 12 |
| Total number of participants | 64 | 65 | 69 |
| EIO/D/Ms | 10 | 21 | 19 |
| Service providers/coordinators | 36 | 29 | 36 |
| Parents | 18 | 15 | 14 |
In-person Learning Sessions - Kick off Events
Each UCEDD hosted an in-person Learning Session where all participating stakeholders were asked to attend. The objectives of the Learning Sessions were to:
- Provide an overview of IFaCT
- Review NYS's current performance related to family outcomes
- Discuss family centered practices and high quality IFSPs
- Describe the quality improvement process
- Help teams develop a plan for the upcoming year. At the kickoff participants were formed into teams based on geographic proximity.
- Table 4. UCEDD In-person Learning Collaborative Sessions (Cohort 1)
- Table 5. UCEDD In-person Learning Collaborative Sessions (Cohort 2)
- Table 6. Kick off Events - Dates & Location
At each Learning Session a parent of a child with developmental disabilities, who received EI, presented on their family perspective of the EIP and how they felt EI services could be improved to have a greater focus on family-centeredness. There was also an opportunity for team members to ask the parent speaker questions. Each speaker was powerful, moving, and was well received.
The first group activity involved teams reflecting on their experiences in the EIP and their current practice. Participants were provided with pre-work to complete prior to the in-person Learning Session. During the in-person session, parents shared their experiences in planning their child's services and connecting with their community. Providers shared how they involve parents in planning services and connecting families to their community. The teams also brainstormed ideas for improving family involvement in services and connecting families to their community.
In the next group activity, the county teams worked together to formulate their team's AIM statement. The AIM statement is a goal that is specific to what the team wants to achieve, can be measured, is attainable, relevant to family outcomes, and is timely. The teams reviewed and selected evidence-based strategies that support the expected high-quality services included in the Family-Centeredness Survey Scale (FCSS) scale.
Figure 4. Sample Cohort 2 AIM Statement
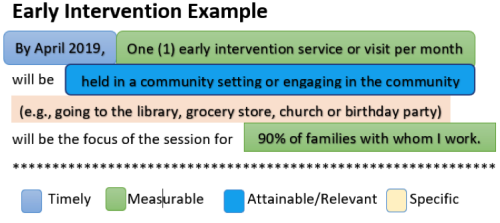
Once the team completed their AIM statement and established the goal of what they wanted to achieve, they then moved on to create their Plan, Do, Study, Act (PDSA) Plan. Each team used the PDSA methodology to decide what small change would be made to improve family outcomes, how it would be done, study the impact the change has made, and then act on it. If the change improved family outcomes the team would increase its use, and if the change does not help, the team would re-evaluate and adjust their plan accordingly. The teams then finalized how they would measure and track their challenges, successes, and any needed modifications to their plans.
Figure 5. PLAN-DO-STUDY-ACT (PDSA) Cycle
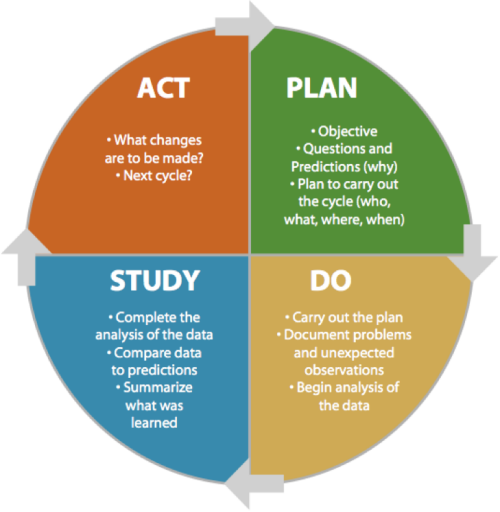
Ref: The Breakthrough Series: IHI's Collaborative Model for Achieving Breakthrough Improvement. IHI Innovation Series white paper. Boston: Institute for Healthcare Improvement; 2003; available on www.IHI.org
At the end of the in-person Learning Sessions, teams shared their AIM statements and what they planned to do to improve family outcomes in their local programs with the other county teams.
Project Implementation
After each in-person Learning Session, the county teams began working on their projects. Each team made small changes using the strategies that their team laid out in their PDSA.
Table 8. Sample of PDSA Cycle
| PDSA Cycle 1 | PDSA Cycle 2 | PDSA Cycle 3 |
|---|---|---|
| AIM Create a resource (e.g., online library, brochure, list) detailing parent networking opportunities within/near county to be distributed to at least 80% of new EI parents each month |
AIM Create a resource (e.g., online library, brochure, list) detailing parent networking opportunities within/near county to be distributed to at least 80% of new EI parents each month |
AIM Create a resource (e.g., online library, brochure, list) detailing parent networking opportunities within/near county to be distributed to at least 80% of new EI parents each month |
STEPS
|
STEPS
|
STEPS
|
MEASUREMENT
|
MEASUREMENT
|
MEASUREMENT
|
The UCEDDs held monthly coaching calls with all teams present to discuss each team's plans, accomplishments, barriers encountered during implementation of their plan, and any changes they made to their plan. Each month the teams followed their PDSA and completed a cycle, which includes implementing family-centered practices with a few of the families they serve in a short period of time. After reviewing data, the teams determined whether they should abandon (i.e., it did not work at all or had negative outcomes), adapt (i.e., it worked but needs to be modified), or adopt (i.e., implement with more families or across different settings). These cycles happened for a twelve-month period with coaching and mentorship from the UCEDD and peer support and collaboration with other teams in their region.
Figure 6. Institute for Healthcare Improvement Model for Improvement
Ref: The Breakthrough Series: IHI's Collaborative Model for Achieving Breakthrough Improvement. IHI Innovation Series white paper. Boston: Institute for Healthcare Improvement; 2003; available on www.IHI.org
Figure 7. Learning Collaborative Process
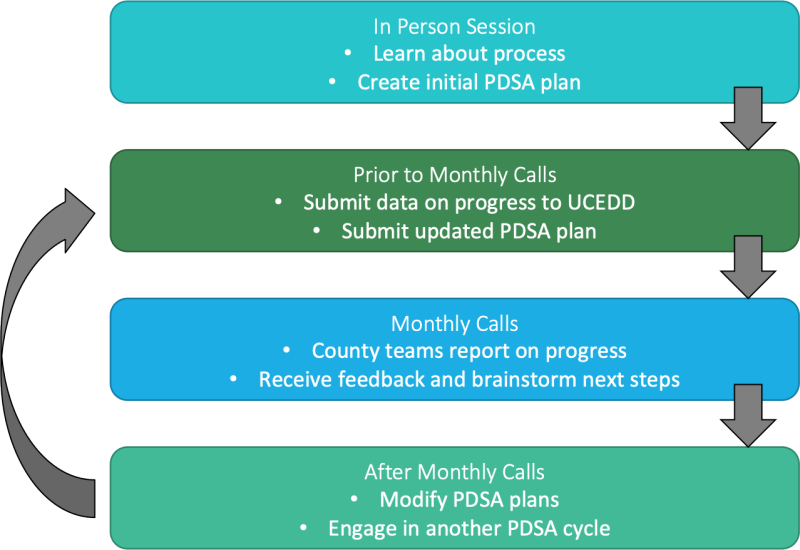
Cohort 1 & 2 Projects
Evaluation Plan
- SSIP Evaluation Plan (PDF)
The current strategy of the SSIP is focused on promoting the use of the Family-Directed Assessment (FDA). The State has developed this evaluation plan to determine if the strategy is successful. If it is successful, it is expected that the percent of eligible children whose families completed an FDA would increase over time. It is also expected that the percent of positive responses should be higher among families who completed an FDA, as their providers have a greater understanding of their strengths and needs.
Scale-Up
Two projects from the SSIP that were successful for the counties, have now been implemented at the State level.
Family Listserv: The State has now created a Family Listserv where the Department can send out information pertaining to families, like relevant trainings, resources, events, policies, and more, directly to families. You can learn how to subscribe to this listserv here: https://www.health.ny.gov/community/infants_children/early_intervention/mailing_list.htm
Facebook: The Department has created a Facebook Group called "NYSDOH – Early Intervention Community of Families" . The group will be used for the State to engage with families, connect them with other families, and promote trainings, resources, events, and more.
The Department has also created postcards to promote both of these initiatives that can be given to the families of the Early Intervention Program:
- Stay Connected Postcard – English (PDF)
- Stay Connected Postcard – Bengali (PDF)
- Stay Connected Postcard – Chinese (PDF)
- Stay Connected Postcard – Haitian-Creole (PDF)
- Stay Connected Postcard – Korean (PDF)
- Stay Connected Postcard – Russian (PDF)
- Stay Connected Postcard – Spanish (PDF)
*If you would like to request hard copies of these postcards, please e-mail OGS.SM.GDC@OGS.NY.GOV. Make sure to include the publication number which is found at the bottom left corner of the postcard, as well as your name, address to send the document to, and quantity.
Trainings for Families and Professionals
Training on Best Practices
- Training for Families (PDF)
- Training for Providers (PDF)